Indications
•Anteroseptal myocardial infarction
•Congestive heart failure
•Depressed ejection fraction %
•Large area of akinesis/dyskinesis
–Asynergy of >30 % of LV surface
•Enlarged ventricle
–End-diastolic volume index >120 cc/m2
–End-systolic volume index >60 cc/m2
•Retained basilar heart function
•Candidate for revascularization
•Candidate for valve repair/replacement
•Good right ventricular function
Relative contraindications
•Multiple areas of infarction
•Loss of basilar myocardial function
•Pulmonary hypertension and right ventricular dysfunction
•Unreconstructable coronary artery disease
Absolute contraindications
•Viable myocardium anterior wall
•Active ischemia with unreconstructable coronary artery disease
Surgical Procedures
There is no one SVR operation. Although all of the different procedures generally referred to as SVR have the same surgical goals and achieve the same or similar morphological results, they do so via different techniques.
All require median sternotomy and cardiopulmonary bypass. Bicaval cannulation is preferred when there is a possibility of valve intervention. It is a good idea to place a femoral arterial line in the event that an intra-aortic balloon pump is necessary. Concomitant coronary artery bypass grafting (CABG) is usually performed; the standard approach for CABG at that institution is utilized, including myocardial protection.
The sequence of procedures performed is a matter of personal preference. We generally use a variation of the Dor technique of endoventricular circular patch plasty but have used most of the major described techniques [10, 11]. Our approach is to perform the CABG first, followed by the mitral repair and the SVR last. The mitral valve repair can be performed in a standard trans-atrial fashion or via a left ventricular approach [12]. Our preference is to perform the entire procedure under full cardioplegic arrest. If the cardiac function is poor, we will complete the proximal anastomoses, remove the cross clamp, and perform the SVR after the heart has been reperfused and in extreme cases have done the entire operation beating.
What follows is a description of the primary SVR procedures.
Dor Procedure
This procedure was named after Dr Vincent Dor who first described it as endoventricular circular patch plasty. This procedure is what people generally are referring to when they use the terms SVR, remodeling, or reconstruction or the surgical anterior ventricular endocardial reconstruction (SAVER) procedure. The technique was introduced to improve geometric reconstruction compared to standard linear repair of left ventricle (LV) aneurysms [10]. Subsequently, Dor and colleagues showed that it was applicable not only to classic aneurysms but also to large akinetic ventricles. Results with the Dor procedure have changed the approach to patients with CHF. SVR has become a standard part of the heart failure surgical armamentarium in patients with advanced heart failure and dilated and dysfunctional ventricles [13, 14].
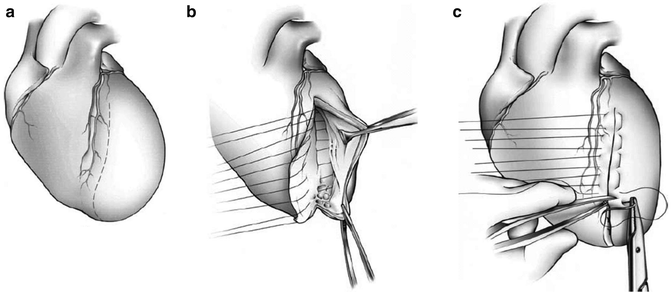
The procedure begins with CABG and valve repair if indicated, on an arrested heart. The heart is vented through the aortic root which results in a collapsed left ventricle in patients with the classic thinned-out anterior wall (Fig. 6.1a). In patients without full-thickness infarction and thinned-out walls, collapse may not occur. A ventriculotomy is then made in the anterior wall parallel to the left anterior descending coronary artery through the center of the scarred tissue (Fig. 6.1b). It is extended proximally and distally as necessary. Retraction sutures are then placed to aid in exposure.
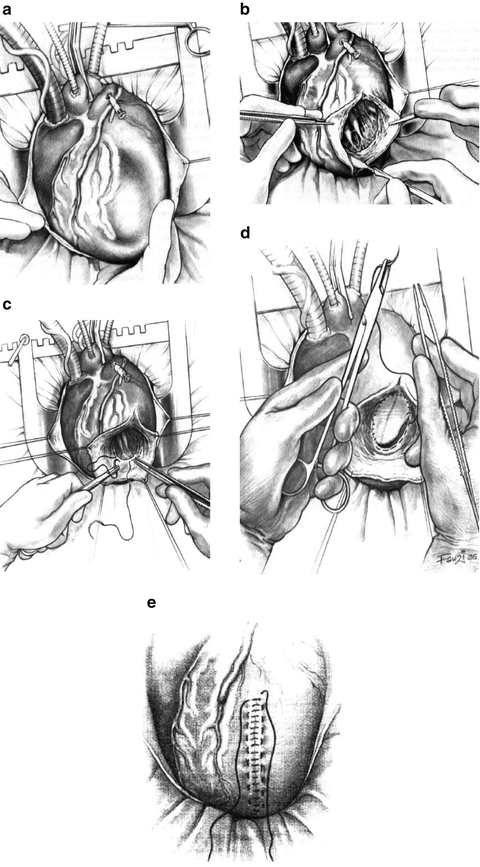

Fig. 6.1
(a) Anterior wall of infarcted left ventricle with sunken appearance while on suction. (b) Ventriculotomy parallel and lateral to left anterior descending coronary artery through scar tissue on anterior wall exposing left ventricular chamber. (c) Circumferential purse string (“Fontan stitch”) outlining border of new anterior wall and apex of left ventricle. (d) Patch closure of anterior left ventricular opening. (e) Final two-layered closure of residual scar over patch. (Reprinted from Operative Techniques in Cardiac & Thoracic Surgery, Vol. 2, Dor V, Surgical management of left ventricular aneurysms by the endoventricular circular patch plasty technique, pages 139–150, copyright 1997, with permission from Elsevier)
The LV is assessed by visualization and palpation to identify the presence or absence of ventricular thrombus, the extent of septal anterior, lateral, and inferior wall infarction, papillary muscle infarction and the interpapillary muscle distance.
An encircling stitch is then placed which outlines the margins of the reconstructed anterior wall (Fig. 6.1c). It runs from the point selected as the new apex cephalad along the septum and then crosses over the most superior margin of the anterior ventriculotomy and down the anterolateral wall back to the new apex. This is commonly referred to as the “Fontan stitch” after Dr Francis Fontan [15]. I routinely use two stitches. Many select the location of this stitch at the visual border of the infarcted and normal tissue; some will perform the ventricular reconstruction on a beating heart and will use the border of the beating and non beating myocardium or between the palpably thinned-out and normal tissue as a guide. Many others will use homemade or commercially available sizing devices. The concept of ventricular sizing was introduced by Dr Dor who used an inflated balloon to size the ventricles. I routinely use a device inflated to a volume of 50–60 cc/m2 body surface area to estimate the patients’ own end-diastolic volume. As a general rule of thumb the height of the septum is not reduced greater than 50 % regardless of the extent of septal infarction.
The encircling stitch is tied to reduce the size of the opening. If the residual opening is greater than 3 cm, a patch is used to close the opening (Fig. 6.1d). If smaller, a linear closure is then performed (Fig. 6.1e). If the quality of the remaining tissue is suboptimal, the linear closure is reinforced with wither bovine pericardium or felt strips.
Modified Linear Closure Technique with Septoplasty
This technique is very similar to a standard linear closure technique for ventricular aneurysms. In this technique, the anterior wall is opened as described above. Once the margins of reconstruction of the anterior wall are identified, horizontal mattress sutures are placed externally through the anterior wall down through the scarred septum medially and continued laterally up through the endocardial scar of the anterolateral wall. These sutures are generally reinforced externally with felt or pericardial strips (Fig. 6.2a, b). A standard linear ventricular closure is performed in layers.
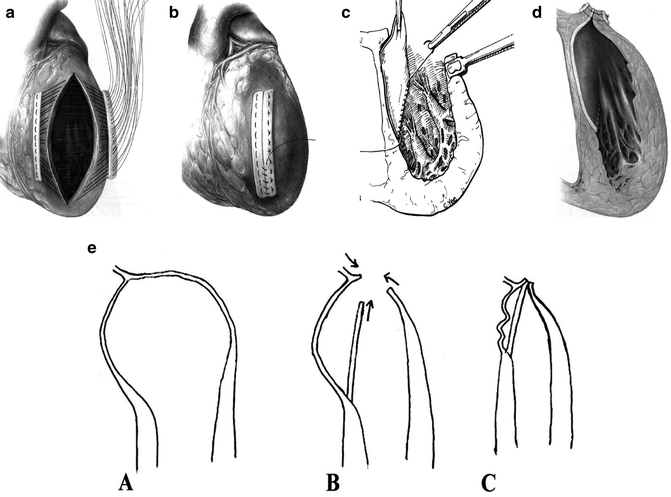

Fig. 6.2
(a) Reinforced linear closure of left ventricle. (b) Final reinforced linear closure of left ventricle. (c) Septal patch over infarcted septal scar. (d) Final view of reinforced linear closure with septal patch. (Fig. 6.2a–d reprinted from Operative Techniques Cardiac & Thoracic Surgery, Vol. 2, Mickleborough LL, Left ventricular aneurysm: modified linear closure technique, pages 118–131, copyright 1997, with permission from Elsevier.) (e) Longitudinal view of linear closure with septal patch. (Reprinted from The Journal of Thoracic and Cardiovascular Surgery, Vol. 128, Mickleborough LL, Merchant N, Ivanov J, Rao V, Carson S, Left ventricular reconstruction: early and late results, pages 27–37, copyright 2004, with permission from Elsevier)
What makes this technique unique is when a septoplasty is added in patients with large septal infarctions to reduce the volume of the septum. Dr Linda Mickleborough of Toronto has popularized this technique [16, 17]. A curvilinear patch of Dacron or pericardium is sewn along the margins of the septal wall along three sides (Fig. 6.2c). The anterior linear closure sutures are then placed in such a fashion to sandwich the remaining side of the patch between the medial and lateral walls creating a new septum and anterior wall (Fig. 6.2d). This can be seen diagrammatically in Fig. 6.2e.
Jatene Modified Septoplasty Technique
The technique introduced and popularized by Dr Adib Jatene [18]. This technique is similar to the Dor technique in that it utilizes a concentric purse string to demarcate the border of the new anterior wall and can be performed with or without a patch.
It is rendered a unique technique by the addition of a septoplasty to reduce the volume in the septum. The septoplasty is accomplished by imbricating the septum with several horizontal mattress sutures which are placed along the septum taking multiple bites of scar tissue beginning near the apex of the heart and running towards the base of the heart until normal tissue is encountered. Sutures are placed in the full height of the infarcted septal tissue and when tied reduce the length of the septum. The encircling stitch is then placed, and the remainder of the reconstruction and closure of the ventricle can proceed in a fashion with or without a patch analogous to the Dor procedure [19].
Septal Exclusion Technique
This technique was described by the French surgeon Guillmet in 1984 to treat aneurysms which primarily involved the septum [20]. This technique is quite unique in that it employs interrupted U-shaped stitches to reapproximate the anterior wall to the septum directly from within the ventricle. The procedure begins like any of the SVR procedures with an anterior ventriculotomy (Fig. 6.3a). A series of interrupted horizontal mattress or U-shaped sutures are placed from the most lateral portion of the anterior wall and anchored on the septal scar (Fig. 6.3b). The sutures are placed from the base towards the apex, and after all the sutures are placed, they are tied in the same sequence. The remaining tissue is reapproximated providing a hemostatic closure in a standard fashion (Fig. 6.3c) [21].