Chapter 4 Understanding the Normal ECG
Please go to expertconsult.com for supplemental chapter material.
As the sample ECG in Figure 3-2 showed, the patterns in various leads can appear to be different, and even opposite of each other. For example, in some, the P waves are positive (upward); in others they are negative (downward). In some leads the QRS complexes are represented by an rS wave; in other leads they are represented by RS or qR waves. Finally, the T waves are positive in some leads and negative in others.
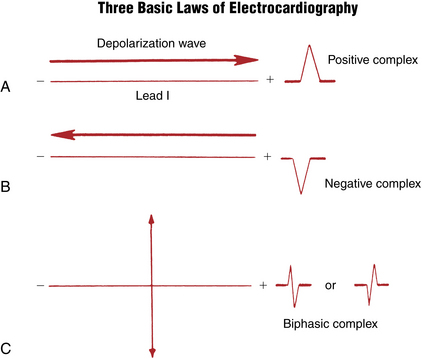
Three Basic “Laws” of Electrocardiography
To answer these questions, you need to understand three basic ECG “laws” (Fig. 4-1):
1. A positive (upward) deflection appears in any lead if the wave of depolarization spreads toward the positive pole of that lead. Thus, if the path of atrial stimulation is directed downward and to the patient’s left, toward the positive pole of lead II, a positive (upward) P wave is seen in lead II (Figs. 4-2 and 4-3). Similarly, if the ventricular stimulation path is directed to the left, a positive deflection (R wave) is seen in lead I (see Fig. 4-1A).
2. A negative (downward) deflection appears in any lead if the wave of depolarization spreads toward the negative pole of that lead (or away from the positive pole). Thus, if the atrial stimulation path spreads downward and to the left, a negative P wave is seen in lead aVR (see Figs. 4-2 and 4-3). If the ventricular stimulation path is directed entirely away from the positive pole of any lead, a negative QRS complex (QS deflection) is seen (see Fig. 4-1B).
3. If the mean depolarization path is directed at right angles (perpendicular) to any lead, a small biphasic deflection (consisting of positive and negative deflections of equal size) is usually seen. If the atrial stimulation path spreads at right angles to any lead, a biphasic P wave is seen in that lead. If the ventricular stimulation path spreads at right angles to any lead, the QRS complex is biphasic (see Fig. 4-1C). A biphasic QRS complex may consist of either an RS pattern or a QR pattern.
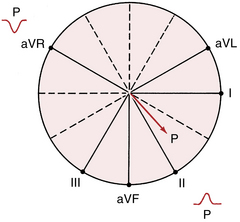
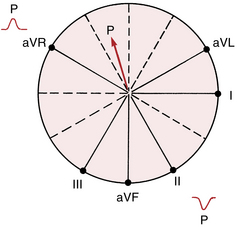
Figure 4-3 With sinus rhythm the normal P wave is negative (downward) in lead aVR and positive (upward) in lead II. Recall that with normal atrial depolarization the arrow points down toward the patient’s left (see Fig. 4-2), away from the positive pole of lead aVR and toward the positive pole of lead II.
Keeping the three ECG laws in mind, all you need to know is the general direction in which depolarization spreads through the heart at any time. Using this information, you can predict what the P waves and the QRS complexes look like in any lead.
Normal Sinus P Wave
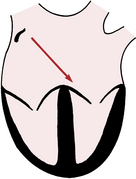
The P wave, which represents atrial depolarization, is the first waveform seen in any cycle. Atrial depolarization is initiated by spontaneous depolarization of pacemaker cells in the sinus node in the right atrium (see Fig. 1-1). The atrial depolarization path therefore spreads from right to left and downward toward the atrioventricular (AV) junction. The spread of atrial depolarization can be represented by an arrow (vector) that points downward and to the patient’s left (see Fig. 4-2).
Figure 3-7C, which shows the spatial relationship of the six frontal plane (extremity) leads, is redrawn in Figure 4-3. Notice that the positive pole of lead aVR points upward in the direction of the right shoulder. The normal path of atrial depolarization spreads downward toward the left leg (away from the positive pole of lead aVR). Therefore, with normal sinus rhythm lead aVR always shows a negative P wave. Conversely, lead II is oriented with its positive pole pointing downward in the direction of the left leg (see Fig. 4-3). Therefore, the normal atrial depolarization path is directed toward the positive pole of that lead. When sinus rhythm is present, lead II always records a positive (upward) P wave.
Four important notes about sinus rhythm:
1. Students and clinicians, when asked to define the criteria for sinus rhythm, typically mention the requirement for a P wave before each QRS complex and a QRS after every P, along with a regular rate and rhythm. However, these criteria are not necessary or sufficient. The term sinus rhythm answers the question of what pacemaker is controlling the atria. You can see sinus rhythm with any degree of heart block, including complete heart block, and even with ventricular asystole (no QRS complexes during cardiac arrest!).
2. As described later, you can also have a P wave before each QRS and not have sinus rhythm, but an ectopic atrial mechanism.
3. If you state that the rhythm is “normal sinus” and do not mention any AV node conduction abnormalities, listeners will assume that each P wave is followed by a QRS and vice versa. The more technical and physiologically pure way of stating this finding would be to say, “Sinus rhythm with 1:1 AV conduction.” Clinically, this statement is almost never used but if you try it out on a cardiology attending, she will be astounded by your erudition.
4. Sinus rhythm does not have to be strictly regular. If you feel your own pulse, during slower breathing you will note increases in heart rate with inspiration and decreases with expiration. These phasic changes are called respiratory sinus arrhythmia and are a normal variant, especially pronounced in young, healthy people with high vagal tone.
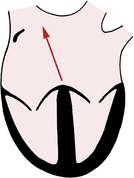
Using the same principles of analysis, can you predict what the P wave looks like in leads II and aVR when the heart is being paced not by the sinus node but by the AV junction (AV junctional rhythm)? When the AV junction (or an ectopic pacemaker in the lower part of either atrium) is pacing the heart, atrial depolarization must spread up the atria in a retrograde direction, which is just the opposite of what happens with normal sinus rhythm. Therefore, an arrow representing the spread of atrial depolarization with AV junctional rhythm points upward and to the right (Fig. 4-4), just the reverse of what happens with normal sinus rhythm. The spread of atrial depolarization upward and to the right results in a positive P wave in lead aVR, because the stimulus is spreading toward the positive pole of that lead (Fig. 4-5). Conversely, lead II shows a negative P wave.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree