Chapter 13 Sinus and Escape Rhythms
Please go to expertconsult.com for supplemental chapter material.
Sinus Rhythms
“Normal” Sinus Rhythm
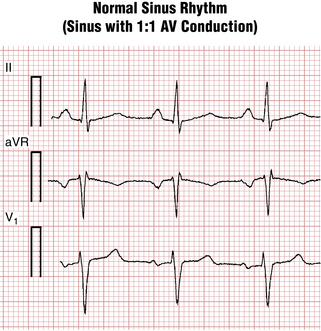
Sinus rhythm is the primary physiologic mechanism of the heartbeat. You diagnose it by finding P waves with a predictable polarity (see Chapter 4). When the sinus (also called the sinoatrial or SA) node is pacing the heart, atrial depolarization spreads from right to left and downward toward the AV junction. An arrow representing this depolarization wave points downward and toward the (patient’s) left. Therefore, with normal sinus rhythm, the P wave is always positive in lead II and negative in lead aVR (see Figs. 4-3 and 13-1).
Key Point
Recall the following from Chapter 4:
 If you state that the rhythm is “normal sinus” and do not mention any AV node conduction abnormalities, listeners will assume that each P wave is followed by a QRS complex and vice versa. The more technical and physiologically unambiguous way of stating this finding is to say: “Sinus rhythm with 1:1 AV conduction.”
If you state that the rhythm is “normal sinus” and do not mention any AV node conduction abnormalities, listeners will assume that each P wave is followed by a QRS complex and vice versa. The more technical and physiologically unambiguous way of stating this finding is to say: “Sinus rhythm with 1:1 AV conduction.”
 However, do not forget that sinus rhythm (i.e., the sinus node is the dominant or sole pacemaker of the atria) can exist not only with normal (1:1) AV conduction but with any degree of AV heart block (including complete or third degree) or even with ventricular tachycardia or asystole.
However, do not forget that sinus rhythm (i.e., the sinus node is the dominant or sole pacemaker of the atria) can exist not only with normal (1:1) AV conduction but with any degree of AV heart block (including complete or third degree) or even with ventricular tachycardia or asystole.
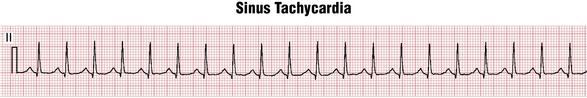
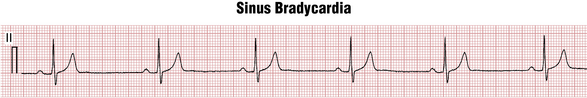
By convention, normal sinus rhythm in a resting subject is usually defined as sinus rhythm with a heart rate between 60 and 100 beats/min. Sinus rhythm with a heart rate greater than 100 beats/min is termed sinus tachycardia (Fig. 13-2). Sinus rhythm with a heart rate of less than 60 beats/min is called sinus bradycardia (Fig. 13-3). Some authors define sinus bradycardia based on a heart rate of less than 50 beats/min.
Regulation of the Heart Rate
The heart, like other organs, has a special nerve supply from the autonomic nervous system, which controls involuntary muscle action. The autonomic nerve supply to the heart (in particular, the SA and AV nodes) consists of fibers with opposing effects: the sympathetic nerves and the parasympathetic nerves. Sympathetic stimulation increases the heart rate and the strength of myocardial contraction. Sympathetic stimulation also occurs by secretion of circulating hormones called catecholamines (especially, norepinephrine and epinephrine), produced by the adrenal glands.
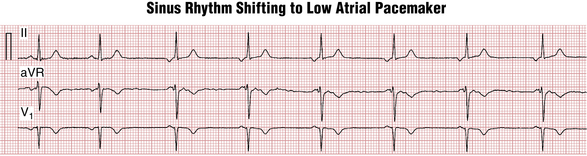
Parasympathetic stimulation (from the vagus nerve) produces slowing of the sinus rate as well as increased conduction time through the AV nodal area. It can also cause a pacemaker “shift” from the SA node to the low right atrial area producing so-called low atrial rhythm with negative P waves in leads II, III, and aVF (Fig. 13-4).
Sinus Tachycardia
Aging decreases the capacity to generate very rapid sinus rates. Elderly individuals (especially those older than 70 years) rarely show sinus tachycardia at rates above 140 to 150 beats/min even during maximal exertion. Indeed, heart rates above this range in the elderly, especially at rest, usually indicate the presence of a nonsinus tachycardia (e.g., atrial fibrillation or flutter, or a paroxysmal supraventricular tachycardia).
Figure 13-2 shows an example of sinus tachycardia. Each sinus P wave is followed by a QRS complex, indicating sinus rhythm with 1:1 AV conduction. Sinus tachycardia (or bradycardia), however, can occur with any degree of AV block. Notice that the P waves are positive in lead II. With sinus tachycardia at very fast rates, the P wave may merge with the preceding T wave and become difficult to distinguish.
In general, sinus tachycardia occurs with any condition that produces an increase in sympathetic tone or a decrease in vagal tone (Box 13-1
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree