(1)
Department of Medicine, Johns Hopkins University School of Medicine, Baltimore, MD, USA
Keywords
InfarctionIschemiaPathologicQ wavesST depressionST elevationT wave inversionReversibleReciprocalMyocardial infarction occurs when oxygen delivery to the myocardium is inadequate for metabolic requirements and remains inadequate to the point of cellular death. This is in contrast to myocardial ischemia, wherein there is also inadequate oxygen delivery to the myocardium, but it is only temporary and is not prolonged or severe enough to lead to cell death. There is clearly a spectrum of response to inadequate oxygen delivery to the myocardium, ranging from mild ischemia through moderate and finally severe ischemia, and, if not reversible, ultimately to myocardial infarction (Fig. 3.1). The electrocardiographic appearance one observes depends on where on this spectrum the patient’s oxygen compromise is located and which portion of the myocardium is affected.


Fig. 3.1
Spectrum of injury from cardiac oxygen deprivation
Ischemia
Ischemia is usually manifested by reversible ST segment depression. The reversibility of the changes is critical to the diagnosis of ischemia. The changes are reversible within a period of minutes, not weeks or months as may be the case with the changes of infarction. The ST segment depression may be downsloping, horizontal, or upsloping in configuration (Fig. 3.2). The most specific configuration for ischemia is downsloping ST segment depression, but this may occur in other situations as well (e.g., left ventricular hypertrophy—see Chap. 6) so it is not completely specific for ischemia. What is most specific for ischemia is reversible downsloping ST segment depression associated with symptoms of angina (e.g., substernal pressing chest pain, dyspnea, diaphoresis). Horizontal ST segment depression is not as specific as downsloping ST depression for ischemia, and upsloping ST depression is the least specific. But horizontal and even upsloping ST segment depressions which are associated with symptoms and are reversible do indicate ischemia. Upsloping ST segment depression can sometimes be seen at rapid heart rates without symptoms and does not indicate ischemia, but rather is due to atrial repolarization. These changes are called TA waves.
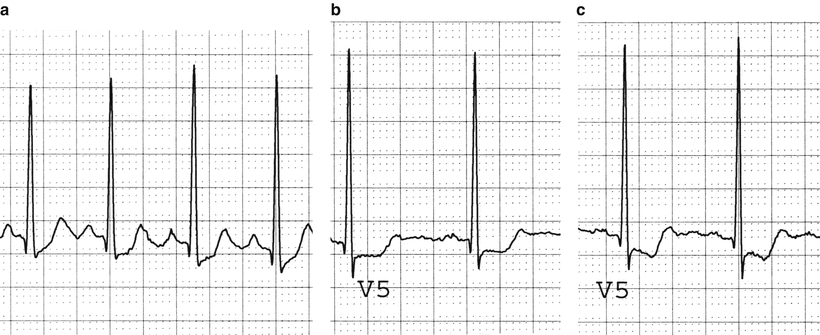

Fig. 3.2
Ischemia. (a) Upsloping ST segment depression. (b) Horizontal ST segment depression. (c) Downsloping ST segment depression
Two additional manifestations of ischemia should be mentioned. A less common form of ischemia than that described above is called Prinzmetal’s angina, and is associated with coronary artery spasm with or without underlying fixed obstructive atherosclerotic disease. In Prinzmetal’s angina, the ST segments are elevated, rather than depressed, and revert to normal over a period of minutes after the vasospasm-induced ischemia is resolved. The distinction between Prinzmetal’s angina and transmural infarction, which is also associated with ST segment elevation (see below), is the rapid reversibility of the ST changes with Prinzmetal’s angina as opposed to the persisting elevation in ST segments (hours to days) with transmural infarction. Finally, in rare circumstances, ischemia may be reflected on the electrocardiogram (EKG) by T wave inversions. This is very uncommon, and T wave inversions are more likely to be related to subendocardial infarction (see below). Nevertheless, when T wave inversions occur, are associated with symptoms of angina, and are reversible within minutes when symptoms resolve, that probably indicates ischemia.
Myocardial Infarction
There are two types of myocardial infarction, and the names have changed over the course of time, with three pairs of terms (Table 3.1).
Table 3.1
Designations of myocardial infarctions
Transmural | Subendocardial |
Q wave | Non-Q wave |
ST elevation | Non-ST elevation |
The oldest designation of the three is (1) transmural and (2) subendocardial, or non-transmural. These two categories imply an anatomical correlation between the appearance of the EKG and the extent of the damage to the heart wall. This implication, however, is not always correct, and hence the attraction to alternative terminology is based on the EKG changes. When the EKG shows the changes of transmural infarction, anatomical studies sometimes but not always confirm an infarction through the entire thickness (“trans-”) of the heart wall (“-mural”). Likewise, when the EKG shows a subendocardial infarction, the damage may not be limited to the subendocardium, but instead may be transmural, based on anatomical correlations [1]. In general, an anatomical transmural infarction associated with the electrocardiographic changes characteristic of “subendocardial” infarction is smaller in magnitude than a transmural infarction with typical transmural changes on the EKG.
Because of the discordance between anatomical findings and the electrocardiographic changes indicating “transmural” or “subendocardial” infarction, the terminology for infarctions changed to first “Q wave,” then “ST elevation” myocardial infarction (STEMI) vs. “non-Q wave” or “non-ST elevation” myocardial infarction (non-STEMI), respectively [2]. Under this classification, the anatomical overtones are dropped, but the association of Q wave or ST elevation infarctions with higher in-hospital mortality, reduced ejection fraction, greater evidence of left ventricular failure, and less postinfarction exercise-induced ischemia compared to non-Q wave or non-ST elevation infarctions is similar to the findings in previous studies comparing “transmural” and “non-transmural” or “subendocardial” infarctions, respectively [3]. STEMIs have a higher in-hospital mortality rate than non-STEMI [4]. That non-STEMIs carry a serious prognosis, however, is clear. Reports suggest that the overall long-term mortality of myocardial infarction patients is the same if not greater after non-STEMI compared to STEMI [3, 5–8]. Non-STEMIs probably represent smaller infarctions with a larger area of myocardium still at risk for future infarction [3, 7]. This notion is supported by studies showing a higher frequency of reinfarction in patients with non-STEMIs compared to patients with STEMIs. The reinfarctions frequently occurred within weeks of the initial infarction and carried a poor prognosis [9, 10].
Subendocardial/Non-Q Wave/Non-ST Elevation Myocardial Infarction
The electrocardiographic change of a non-STEMI is T wave inversion (Fig. 3.3). There is usually little or no depression of the ST segments. Over a period of weeks to months, the acute changes of T wave inversion may revert back to normal, with no residual change to indicate a previous infarction. Alternatively, the T wave inversion may persist in some degree indefinitely.
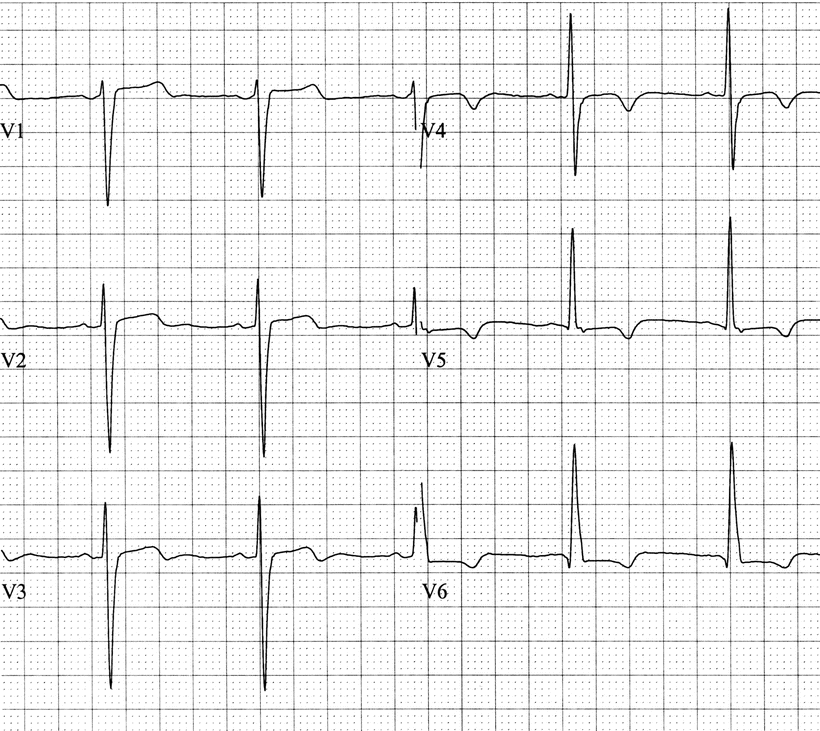

Fig. 3.3
Subendocardial infarction. These are the precordial leads in a patient with an acute anterior subendocardial infarction. Note that the ST segments are essentially normal, but the T waves are biphasic in V3 and inverted in V4–6
Transmural/Q Wave/ST Elevation Myocardial Infarction
The electrocardiographic changes associated with an acute STEMI follow a more complicated pattern (Fig. 3.4). The initial change is ST segment elevation, occurring usually within minutes of the interruption of oxygen delivery. The next change is the development of “pathological Q waves,” Q waves that are new and are of at least 0.04 s duration. The Q waves appear within several hours of the infarction. Over the next few days, the T waves become inverted and the ST segments become less elevated, usually reverting to normal. Over a period of weeks to months, the T wave inversions may resolve, leaving only the Q waves as the residual manifestation of the infarction. This series of changes is known as the evolution of an acute STEMI. Occasionally, the Q waves that remain are not wide and deep and may be indistinguishable from the q waves that can be found as a normal variant. Thus, following either a STEMI or a non-STEMI, it is possible for the EKG to revert to a pattern that is within normal limits and does not reflect the previous infarction. This is more likely to occur with non-STEMI than STEMI, but it can occur with both.
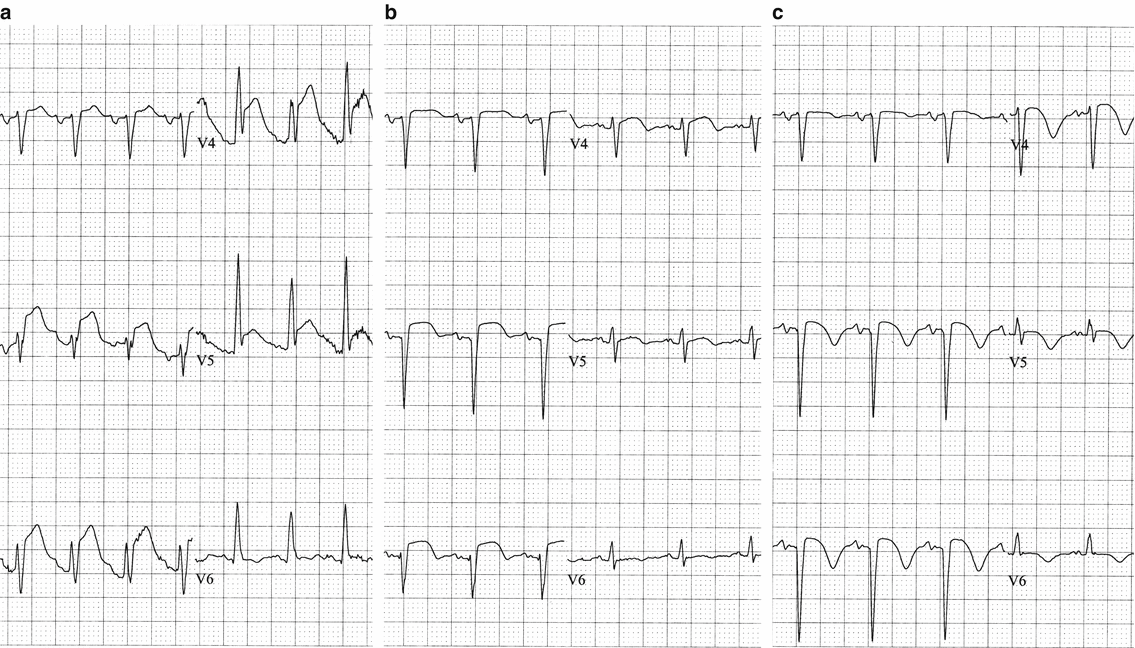

Fig. 3.4
Evolution of a transmural infarction. Precordial leads in a patient with an acute anterior transmural myocardial infarction. (a) At initial presentation the patient has acute ST segment elevation, only a small, nonpathological q wave in V5–6, and no T wave inversions.(b) Four hours later there is a new Q wave in V2 and less ST elevation remains.(c) One day after initial tracing the Q waves are in V2-3, slight ST elevation persists, and the T waves are now inverted in V2–6
Very rarely the first changes on the EKG seen with an acute STEMI are peaked T waves, the so-called hyperacute T waves. This is so rare as to only deserve mention for completeness. It is not a common finding, and when it does occur, it is soon supplanted by the far more typical ST segment elevations described earlier.
Sometimes patients are seen with myocardial infarction, suspected by the patient’s history and confirmed by a typical and significant elevation of cardiac enzymes, but without any electrocardiographic abnormalities [2]. These “electrically silent” or “normal electrocardiographic” infarctions are uncommon.
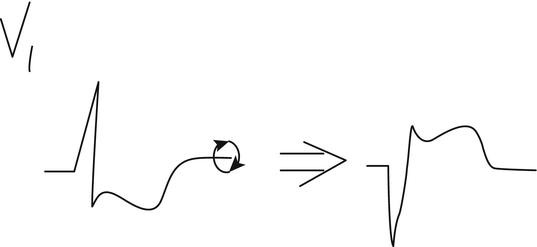
Location of Infarction/Ischemia
There are three general EKG locations for infarctions or ischemia: inferior, anterior, and posterior. The portion of the heart that is affected by infarction or ischemia may be suspected by the electrocardiographic leads in which the changes are found. Even if the correlation is imperfect between the leads reflecting ischemia or infarction and the part of the heart affected, the designation of the location quickly identifies the leads showing changes. As discussed in Chap. 2, leads II, III, and aVF are positive in the legs and negative in the arms, and therefore are most reflective of changes in the inferior wall of the heart and are called the inferior leads. Leads I and aVL, along with the precordial leads, reflect changes in the anterior wall of the heart. Therefore, when there is ischemia or infarction in the inferior wall of the heart, the electrocardiographic changes described earlier in this chapter are typically seen in the inferior leads—II, III, and aVF. When there is anterior wall ischemia or infarction, the changes are typically seen in leads I, aVL, and the precordial leads. Occasionally a distinction is made between the anteroseptal and anterolateral portions of the anterior wall. “Anteroseptal” and “anterolateral” are simply subsegments of the anterior wall, with changes limited to V1–3 or V4–6, respectively. I believe this subdivision of the anterior wall in reference to myocardial injury is of little practical importance, but an anteroseptal infarction with precordial changes limited to V1–3 probably does suggest a less extensive infarction than when the changes are seen in most or all of the precordial leads. The posterior wall of the heart is not reflected directly by any of the standard electrocardiographic leads because none of them are placed on the patient’s back. Instead, posterior wall injury is indirectly reflected by changes in leads V1–2. Since those two leads are directly anterior, they best show changes affecting the posterior wall of the heart, but the changes are reversed from the usual changes of damage described above. An acute posterior STEMI is reflected by ST segment depression and a tall R wave in V1–2 as opposed to ST segment elevation and a Q wave. This is because V1–2 are anterior leads, and in reflecting posterior wall injury these leads would be expected to have opposite changes compared to those seen when the area of injury is directly below the leads. Another way to look at this situation is that the complexes in V1–2 can be rotated around the baseline as an axis when considering the posterior wall of the heart, so ST segment depression becomes ST segment elevation, and the R wave becomes a Q wave in posterior infarction (Fig. 3.5). The presence of ST segment depression in V1–4 in association with changes of acute inferior STEMI is usually due to inferoposterior or posterolateral wall involvement of the infarction rather than a “reciprocal change” [11] (see below).