Chapter 45 Ventricular Tachycardia and Ventricular Fibrillation Without Structural Heart Disease
Idiopathic ventricular tachycardia (IVT) and idiopathic ventricular fibrillation (IVF) have been intermittently recognized and reported since the early 1900s. Since Vakil’s classic description of ventricular aneurysms and their association with ventricular tachycardia (VT), early literature defined VT as being associated with heart disease.1–3 The occurrence of paroxysmal VT in young patients and occasionally those with apparently healthy hearts, emerged from time to time.4,5 The availability of electrocardiographic recordings focused attention on the region of origin of ventricular arrhythmias, including ectopic beats as well as VT.6,7 In 1974, in a careful review of the literature of the twentieth century, investigators from the Chicago School of Electrophysiology noted that “cardiac stimulatory studies suggest the site of origin of ventricular ectopic beats can be identified by QRS configuration.” Ectopic beats were classified according to their bundle branch block–like configuration, with left ventricular origin being ascribed to right bundle branch configurations and right ventricular origin to left bundle branch configurations.8 The latter were credited with a more favorable outcome. However, occasional reports of deaths in young patients existed, disputing a uniform benign prognosis. With advances in the evaluation and management of ventricular arrhythmias, there now exists a far greater body of knowledge regarding these conditions. IVT and IVF have been studied for anatomic substrate, clinical electrophysiology, and outcomes with and without therapy. This chapter summarizes the current understanding of this constellation of conditions.
Definition and Classification
In current-day parlance, IVT refers to VT of unknown cause that occurs in the absence of significant structural heart disease or transient or reversible arrhythmogenic factors (e.g., electrolyte disorders, myocardial ischemia). IVF may include polymorphic VT evolving to VF or may initiate directly as VF. In practice, one cannot categorically exclude patients with evidence of structural heart disease because advances in diagnostic tests demonstrate structural changes in some patients with classic IVT syndromes.9–11 Magnetic resonance imaging (MRI) has shown subtle wall motion disturbances that may represent structural disease.12–15 In addition, a patient could have structural disease caused by a coexisting cardiac disorder. The term idiopathic is sometimes inappropriate given the depth of understanding that now exists for a few of the disorders. For the purposes of this discussion, the syndromes listed in Box 45-1 are assumed to be distinct IVT syndromes. However, it must be acknowledged that these syndromes consist of heterogeneous subtypes, and some share characteristics with other IVT syndromes so that clear distinctions are not always possible. Moreover, reports of “new” IVTs arise frequently.16,17 Some of these may be previously unrecognized syndromes, whereas others may be variants of established forms.
Box 45-1 Idiopathic Ventricular Tachyarrhythmia Syndromes
Monomorphic VT Syndromes
Epidemiology
Epidemiologic data on IVT syndromes are scarce because of difficulties in recognizing the syndrome and its demographics. The demographics of the clinical syndrome of IVT derived initial impetus from clinical and later electrophysiological studies (EPSs). Pietras et al analyzed 27 patients with chronic recurrent VT classified according to the electrocardiogram (ECG) classification and examined their clinical, ECG, and hemodynamic features.8 They further tabulated 73 reported cases in the then-existing literature. They noted that the mean age of right-sided VT was lower (32 years) than that of left-sided VT (43 years), with a similar trend in the previously reported data (36 vs. 53 years). Females predominated in the case of right-sided VT (52% and 66% in the two series, respectively) compared with left-sided VT (33% and 15% in the two series, respectively). Organic heart disease was almost invariably present with left-sided VT (100% and 85%, respectively) and absent or uncommon in right-sided VT (25% and 48%, respectively). Mortality rates were significantly lower in right-sided VT, with no deaths in their series and a 12% incidence in the reported literature. Chapman et al reported electrical and hemodynamic correlates in a series of patients with “idiopathic VT” in 1975.18 Subsequently, EPSs in this syndrome have defined the arrhythmia mechanisms, subgroups, novel clinical therapies, and their outcomes.9,19
Formal epidemiologic data are lacking, but IVT is considered rare. IVT syndromes arising in the right ventricular outflow tract (RVOT) or the left ventricular outflow tract (LVOT) are the most common forms of IVT. The RVOT origin predominates, accounting for more than 70% of referred patients, although LVOT origin is being increasingly recognized.20–22 Aortic cusp IVT has been reported to account for 17% to 21% of outflow tract IVT.23,24 Analysis of multiple-center experiences suggests that IVT constitutes approximately 10% of all VT referrals to electrophysiologists, but the true incidence in the community remains unclear.23 IVF is believed to represent 5% to 10% of sudden cardiac death (SCD) victims and implantable cardioverter-defibrillator (ICD) recipients.25–27 IVF populations are still being defined. Commonly recognized genetic syndromes include the long QT syndrome (LQTS), Brugada syndrome, and the more uncommon short QT syndrome (SQTS). Information regarding their prevalence is emerging and is discussed below. One important subgroup is associated with an early repolarization abnormality.28 Haissaguerre et al described an early repolarization abnormality in 31% of patients with IVF compared with 5% in control groups in a case-control study. Patients with this finding had a higher 5-year mortality rate. These early repolarization abnormalities have now been classified under the term J-wave syndromes.
Population data exist for some genetically based IVT or IVF syndromes. It has been estimated, for instance, that Brugada syndrome accounts for 4 to 10 cases of SCD per 10,000 inhabitants per year in Thailand and Laos, countries with an apparently high incidence. Nevertheless, the problem may be much larger. Autopsy series suggest that in 5% to 15% of cases of SCD, no evidence of heart disease or other likely cause exists.29–31 These observations raise the possibility that the IVT and IVF syndromes are common but insufficiently recognized. IVF syndromes with early repolarization have been studied in both IVF survivors and population studies. Tikannen et al studied more than 10,684 middle-aged subjects and noted that the early-repolarization pattern of 0.1 mV or more was present in 5.8% (3.5% in inferior leads and 2.4% in lateral leads).32 J-point elevation of at least 0.1 mV in inferior leads was associated with an increased cardiac mortality risk (relative risk [RR], 1.34; P = .03); J-point elevation of more than 0.2 mV in inferior leads occurred in 0.3% of patients, who had a markedly elevated risk of death from cardiac causes (RR, 2.98; P < .001) and from arrhythmia (adjusted RR, 2.92; 95% confidence interval [CI], 1.45 to 5.89; P = .01). Long Q-T interval and left ventricular hypertrophy were actually weaker predictors of this outcome. Juntila and Myerburg noted variations in the frequency of early repolarization ranging from 10% to 42% based on ethnicity in healthy athletes.33 Antzelevitch has proposed three subtypes of J-wave syndrome on the basis of these data.34 Type 1, an early repolarization pattern present predominantly in the lateral precordial leads, is common in healthy male athletes and is rarely seen in IVF survivors; type 2, which has the ECG pattern predominantly in inferior or inferolateral leads, has a higher risk; and type 3, which displays global findings and is associated with the highest IVF risk, is often associated with incessant VF.
A recent retrospective multi-center study evaluated the profile of pediatric patients with IVT. Mean age at first manifestation of the arrhythmia was 5.4 years, with a range of 0.1 to 15 years, and 27% of patients manifested the disorder in infancy.35
Mechanisms and Clinical Presentation
The clinical presentation of patients with IVT is highly variable. IVT arising in the outflow tract most often manifests in the third to sixth decade of life and has a female preponderance.36–38 Palpitations in an otherwise healthy young individual are a classic description in this entity. These can be exercise induced or may occur at rest. Salvos of nonsustained VT (NSVT) are common. Hormonal triggers have been reported, and more frequent arrhythmic events, ventricular ectopic beats, or VT events are seen during exercise or increased activity. These can culminate in near syncope or syncope, dysthymia and, on occasion, cardiac arrest. Cardiac arrest can be the primary presentation in some individuals, particularly if a family history of SCD exists. Others seek medical attention in the asymptomatic state with a family history of SCD or for an electrocardiographic abnormality such as LQTS or Brugada syndrome. Increasing awareness of the familial forms of the arrhythmia and symptomatic high-density ventricular ectopy or NSVT can lead to medical evaluation.
Electrocardiographic recordings and exercise testing frequently assist in the classification of IVT and should be routinely performed. These are discussed in the next section and more extensively in Chapters 53 and 70.
Electrocardiographic Features of Idiopathic Ventricular Tachyarrhythmias
Analysis of the surface ECG morphology is an essential aspect of localization of the origin of IVT. The ECG during sinus rhythm is often normal, although a right bundle branch block (RBBB) morphology has been described with outflow tract VT in 10% of patients.20 The primary forms of IVT include arrhythmias arising from the RVOT or LVOT, the aortomitral continuity, and intrafascicular re-entry. These four types of IVTs can be distinguished by characteristic ECG patterns that reflect the origin or mechanism of the arrhythmias. The electrocardiographic features of the RVOT and LVOT reflect the anatomic proximity of these structures. As shown in Figure 45-1, the RVOT is anterior to the right and left aortic cusps. Accurate ECG lead placement is essential to distinguish electrocardiographic features from these areas. Because of the proximity of these anatomic sites, small changes in lead position may have a substantial impact on the ECG morphology of arrhythmias arising from this region. In addition, the close anatomic relationships of the outflow tracts and the great arteries and coronary vasculature make exact localization potentially problematic. Other factors include the exact position of the aortic cusps relative to the RVOT, the axis of the heart, and the precise connections of muscle fibers connecting the tissue above the aortic cusps to the left ventricle.
Right Ventricular Outflow Tract
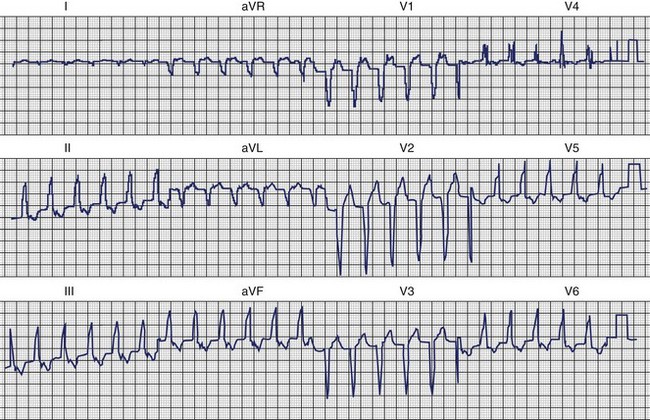
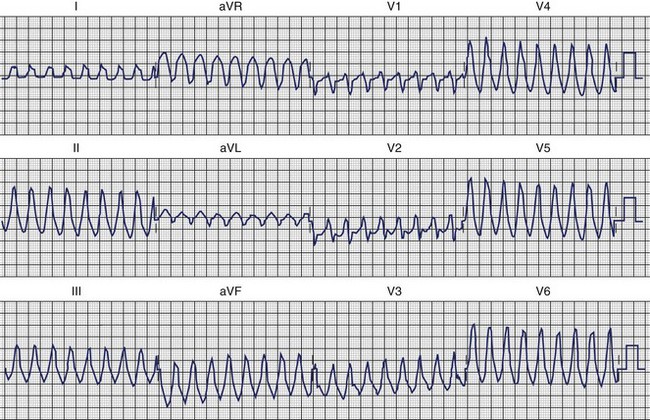
The clinical features and the general ECG characteristics of VT arising from the RVOT were described by Buxton in 1983.19 The ECG exhibits a morphology resembling left bundle branch block (LBBB) with an inferior axis. These arrhythmias are associated with exercise, and in many patients the arrhythmias are nonsustained and repetitive. Others may simply have frequent monomorphic ventricular ectopy. Figure 45-2 was recorded from a patient with repetitive VT arising from the RVOT. Jadonath determined the usefulness of the 12-lead ECG in localizing the origin of RVOT tachycardia in patients who underwent ablation of arrhythmias.39 They divided the RVOT into nine segments and assessed the QRS morphology recorded by pacing at each segment. A QS pattern in lead aVR and monophasic R waves in leads II, II, and aVF were noted in all patients at all nine sites. Pacing at anterior sites produced either a dominant Q wave or qR pattern in lead I, but a monophasic R or Rs complex was never observed. Conversely, a dominant R wave was observed in lead I during pacing from posterior sites. The QRS exhibited a QS pattern in lead aVL during pacing from anterior sites, but the R wave became progressively larger in lead aVL with more posterior sites. Early R-wave transition in the precordial leads was likely to be observed during pacing from the posterosuperior aspect of the septum. Similar results were reported by Yoshida and colleagues.40 Coggins observed that VT arising from the septal side of the RVOT had a negative QRS complex in aVL, whereas VT arising from the lateral aspect of the RVOT was associated with a positive QRS in aVL.21
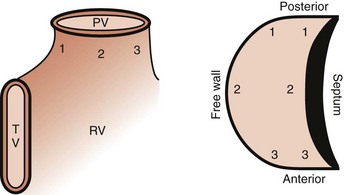
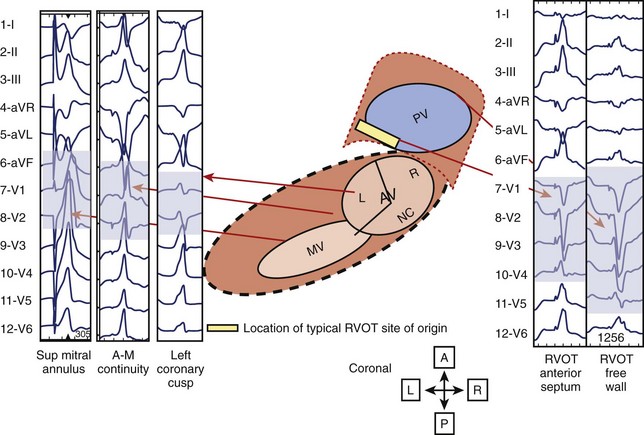
Electroanatomic mapping shows border regions as a low-voltage region in the RVOT at the breakout point or origin of the VT.41 An analysis by Dixit categorized RVOT arrhythmias as arising anterior and leftward on the septal side, as opposed to posterior and more rightward, and distinguished the electrocardiographic features of these arrhythmias from those arising on the free wall. Figure 45-3 displays the scheme used in this analysis.42
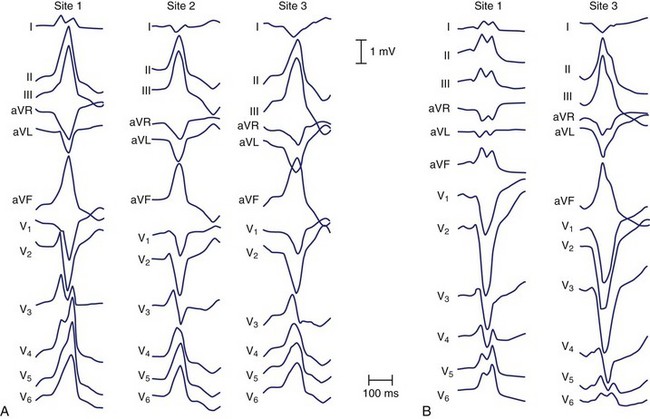
The electrocardiographic features corresponding to these sites are shown in Figure 45-4. As noted by other authors, the amplitude of the R wave in limb lead I depends on the origin being anterior or posterior. They observed that arrhythmias arising from the free wall of the RVOT show more delayed R-wave transition in the precordial leads and notching in the inferior leads.
Left Ventricular Outflow Tract
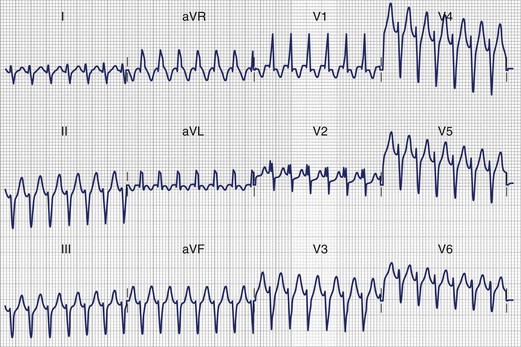
Ventricular arrhythmias arising from the LVOT are distinguished from RVOT arrhythmias by several differences in the QRS morphology. Earliest ventricular activation may arise in the sinus of Valsalva, below the aortic valve, or on the epicardium. Figure 45-5 was recorded from a patient with repetitive VT whose arrhythmia origin was just below the anterolateral aspect of the aortic valve. Callans et al described four patients with monomorphic VT mapped to the LVOT.43 Two patients, whose arrhythmias originated above the mediosuperior aspect of the mitral annulus, had VT that exhibited a right bundle, inferior-axis VT with a dominant R wave in lead V1. The ECGs of these patients resembled those recorded from the five patients studied by Lamberti; in these patients, intracardiac echocardiography had been used to demonstrate that in all of them, VT arose close to the left coronary cusp in the area of atriomitral continuity.44 The other two patients described by Callans had VT that arose from the basal aspect of the superior left ventricular septum. The ECGs recorded from these patients had a left bundle, inferior-axis QRS mapped to the LVOT. The ECGs recorded from these patients were distinguished from the ECGs of those with arrhythmias arising from the RVOT by an earlier precordial R-wave transition (median lead V3 vs. lead V5), more rightward axes, taller R waves inferiorly, and small R waves in lead V1. Absence of an R wave in lead V1 and late precordial transition suggested an origin in the RVOT. These results are similar to those reported by Kamakura and Krebs, who found that if the R/S ratio in lead V3 was 1 or more, the origin was likely to be in the LVOT.45,46 Kanagaratnam described a variant of LVOT VT in 12 patients whose arrhythmias arose from the aortic sinus of Valsalva.47 Two characteristic QRS morphologies were observed. ECGs recorded from all patients had (1) a left-bundle, inferior-axis, tall monophasic R waves inferiorly and (2) early precordial lead transition with rS or RS in lead V1 and Rs pattern in leads V2 or V3. Those in whom the tachycardia was ablated from the noncoronary sinus were distinguished by a notched R in lead I.
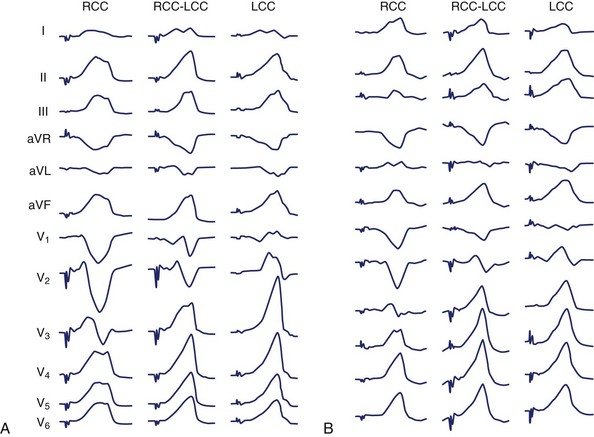
The use of intracardiac echocardiography and radiographic imaging has helped refine the origin of LVOT arrhythmias and their relationship to the coronary cusps and aortomitral continuity.48,49 Pacemapping from the aortic cusps can be difficult because of catheter stability and high thresholds; Figure 45-6 shows characteristic ECG patterns associated with this region. Recordings from the right coronary cusp typically exhibit notching in the downstroke of lead V1 and an R in limb lead I. A W pattern in lead V1 is observed near the commissure of the right and left coronary cusps. Arrhythmias arising from the left coronary cusp exhibit a qrS pattern and either a QS or rS in limb lead I. Each of these locations is associated with a prominent R wave in the inferior leads and an R-wave transition in leads V2 or V3.
Ventricular arrhythmias arising from the aortomitral continuity are characterized by a qR complex in lead V1 and an RS or rs complex in limb lead I. The relationship between aortic and mitral valves is shown in Figure 45-7. The R wave in lead V1 becomes more monophasic as the origin moves more leftward across the superior aspect of the mitral annulus. Figure 45-8 illustrates the differences among the paced or spontaneous beats arising from the RVOT, the left coronary cusp, the aortomitral continuity, and the superior aspect of the mitral annulus.
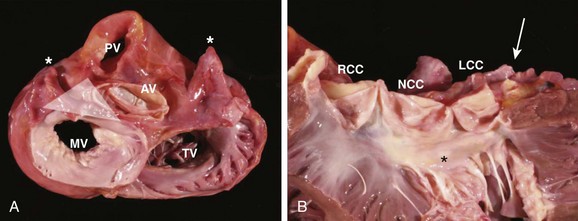
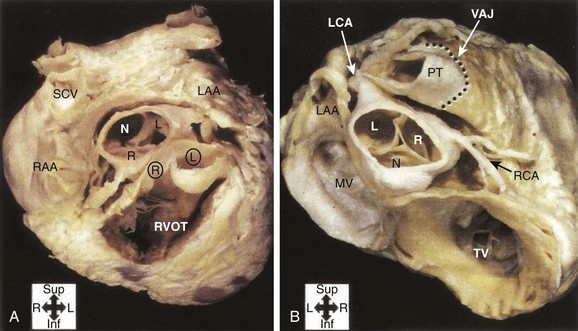
FIGURE 45-7 Gross anatomy of the heart. A, View from the atria toward the valvular apparatus showing the anatomic relationship between the aortic valve (AV), mitral valve (MV), pulmonary valve (PV), and tricuspid valve (TV). Asterisks indicate the left and the right atrial appendages, respectively. The white triangle represents the area of the aortomitral continuity corresponding to Figure 45-2. B, View of the anterior leaflet of the mitral valve (asterisk) after opening of the left ventricle and the aortic valve, showing the close relationship of the aortic valve and the anterior leaflet of the mitral valve. The arrow indicates the left main artery. LCC, Left coronary cusp; NCC, noncoronary cusp; RCC, right coronary cusp.
(From Steven D: Ventricular tachycardia arising from the aortomitral continuity in structural heart disease: Characteristics and therapeutic considerations for an anatomically challenging area of origin, Circ Arrhythm Electrophysiol 2:660–666, 2009.)
Idiopathic Verapamil-Sensitive Left Ventricular Tachycardia
Idiopathic verapamil-sensitive VT that has a QRS pattern of RBBB and left-axis deviation was described by Lin in 1983.50 This is typically seen in adolescents and young adults up to the age of 40 years, with a male preponderence.23 ECG morphologies can include a small r–deep S configuration in some precordial leads. Subsequent studies, which focused on the electrophysiological basis of the arrhythmia and ablation techniques, demonstrated that the QRS axis is usually leftward and superior, although it could be indeterminate or rightward. Electrophysiological data demonstrate that re-entry either is intrafascicular or involves abnormal Purkinje tissue with decremental conduction properties and is sensitive to verapamil.51–58 The exact QRS morphology depends on which branches of the fascicles provide the exit points, and unsuccessful attempts to ablate the arrhythmia have shown changes in QRS morphology that suggest the potential for multiple exit points. Re-entry in and exit points from the left bundle branches predominate, with more than 80% involving the left posterior fascicle as an exit. Anterior left fascicular exit has also been observed. Slowly rising “ rounded” ventricular potentials have been reported during VT, suggesting verapamil-sensitive regions. Sharp potentials have also been seen at exit points, possibly from Purkinje network cells.23 These have been targeted for catheter ablation. Figure 45-9 demonstrates idiopathic left-sided VT caused by fascicular re-entry that was ablated by applying radiofrequency (RF) energy at the site of a presystolic “fascicular” potential on the inferior aspect of the septum approximately 2 to 3 cm from the apex.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree