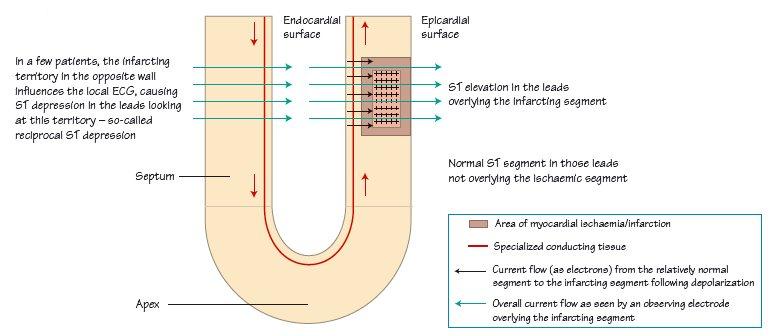
Fig. 31.2 (a) Data from GISSI 1, showing that more leads with ST elevation worsens outcome. This is true both for the index admission (data shown here), and also long term for those who survive the index event, i.e. for those who survive initially, the long-term outcome is best in those with fewest leads showing ST elevation at presentation. (b) Thrombolysis in myocardial infarction (TIMI) risk score for ST segment elevation myocardial infarction (STEMI). Age, haemodynamic data (heart rate, blood pressure) and haemodynamic status (Killip class) are amongst the most powerful adverse predictors of outcome.
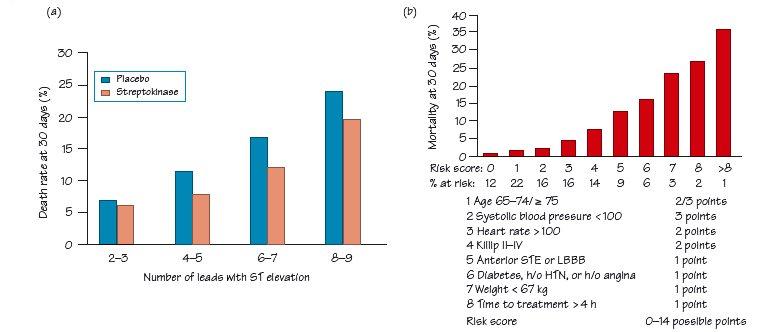
Fig. 31.3 Mechanism of ST elevation in ST segment elevation myocardial infarction (STEMI) (see text).
ST segment elevation myocardial infarctions (STEMIs) are dangerous and require early diagnosis and aggressive reperfusion therapy. They are recognized by characteristic ST elevation in the appropriate clinical setting, usually prolonged ischaemic chest pain, occasionally unheralded acute heart failure and, more rarely, arrhythmias (ventricular tachycardia [VT], ventricular fibrillation [VF], also atrial fibrillation [AF]). ST segment elevation myocardial infarctions are sometimes known as Q wave myocardial infarctions (MIs), or ‘full-thickness’ MIs, as they can progress to Q wave formation, though this is not inevitable.
The stages of a STEMI (Fig. 31.1)
Phase 0 (a non-classic phase): Not often talked about, is the onset of MI, when there maybe no ECG changes. This phase can be demonstrated during percutaneous coronary intervention (PCI) when prolonged balloon inflations sometimes (though not commonly) results in no ECG changes.
Phase 1:
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


