Pericardial Disease Interventions
Paul Sorajja MD, FSCAI
Cardiac tamponade is a life-threatening disorder that can result from any condition that causes a pericardial effusion. Although the most frequent cause is malignancy, tamponade may also occur from pericarditis (e.g., viral, uremic, inflammatory, or idiopathic), aortic dissection from disruption of the aortic annulus, ventricular rupture from myocardial infarction, and virtually any disorder that causes a pericardial effusion (1). In the cardiac catheterization laboratory, tamponade can result from cardiac perforation from a variety of invasive procedures and lead to rapid demise of the patient owing to the swift accumulation of fluid in a poorly compliant pericardial space. Prompt recognition of the salient hemodynamic features and immediate pericardiocentesis are elementary in the successful treatment of cardiac tamponade.
DIAGNOSIS OF TAMPONADE
Cardiac tamponade should be suspected in any patient in the cardiac catheterization laboratory with unexplained hypotension, elevated venous pressure, and a compatible history. Unusual manifestations can also occur. Tamponade may occur without elevated jugular venous pressure because of low intracardiac filling pressures (i.e., low-pressure tamponade), such as in dehydrated patients with malignant effusions. Localized tamponade can result from loculated pericardial effusions, such as those that may be present adjacent to the atria in the postoperative setting.
The hemodynamic effects of a pericardial effusion may be acute or gradual, depending on the amount and rate of fluid accumulation. Normally, the pericardial space contains 15 to 50 mL of fluid with an intrapericardial pressure that approximates intrapleural pressure (-5 to +5 cm H2O). Fluid accumulation and pericardial restraint leads to rises in intrapericardial pressure. Cardiac tamponade occurs when intrapericardial pressure exceeds intracardiac pressure, leading to impaired ventricular filling throughout the entire diastolic period, increases in pulmonary venous and jugular venous pressures, and reduction in forward stroke volume. With inspiration, there is a fall in the driving pressure to fill the left ventricle, subsequently leading to a reduction in ventricular filling and stroke volume. The fall in left ventricular stroke volume during inspiration manifests as a relative decrease in pulse pressure or peak systolic pressure, which is the hallmark finding of pulsus paradoxus in patients with cardiac tamponade.
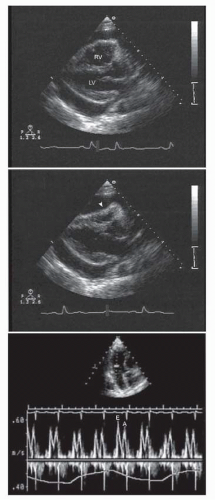
Two-dimensional and Doppler echocardiography is commonly used for diagnosing cardiac tamponade (2, 3). Specific signs of tamponade include diastolic inversion or collapse of the right atrium and right ventricle, ventricular septal shifting with respiration, and plethora of the inferior vena cava (Fig. 43-1). Respiratory variation in the Doppler mitral inflow is a highly sensitive measure that occurs early in tamponade, and may precede changes in cardiac output, blood pressure, and other echocardiographic findings.
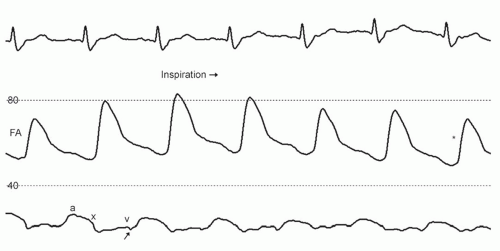
The invasive hemodynamic hallmark of cardiac tamponade is blunting of the y descent in the atrial pressure tracings or blunting
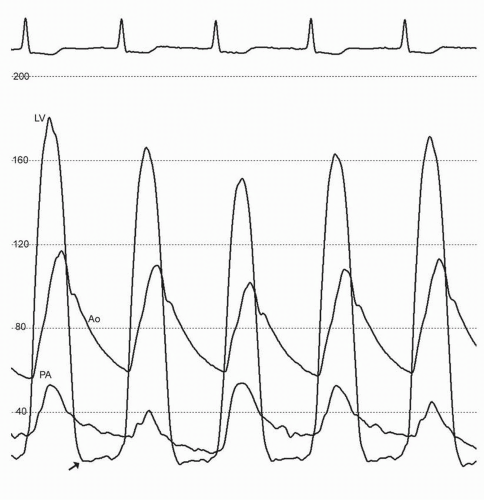
of the early diastolic filling wave in ventricular pressure contour. The x descent is usually preserved because of the decrease in intracardiac volume during systolic ejection, which leads to a temporary reduction in intrapericardial and right atrial pressures (Fig. 43-2). Elevated intrapericardial pressure impairs ventricular filling during the remainder of the cardiac cycle, resulting in blunting of the y descent. These hemodynamic consequences can also manifest in the left ventricular early diastolic (or early minimum) pressure, whose changes may be subtle (Fig. 43-3). The blunting or loss of the early rapid ventricular filling wave is the hallmark of cardiac tamponade that distinguishes it from other diastolic filling disorders (Fig. 43-4). The reduction in left ventricular filling and stroke volume manifests as a decrease in aortic pulse pressure during inspiration in a manner analogous to the bedside finding of pulsus paradoxus.
of the early diastolic filling wave in ventricular pressure contour. The x descent is usually preserved because of the decrease in intracardiac volume during systolic ejection, which leads to a temporary reduction in intrapericardial and right atrial pressures (Fig. 43-2). Elevated intrapericardial pressure impairs ventricular filling during the remainder of the cardiac cycle, resulting in blunting of the y descent. These hemodynamic consequences can also manifest in the left ventricular early diastolic (or early minimum) pressure, whose changes may be subtle (Fig. 43-3). The blunting or loss of the early rapid ventricular filling wave is the hallmark of cardiac tamponade that distinguishes it from other diastolic filling disorders (Fig. 43-4). The reduction in left ventricular filling and stroke volume manifests as a decrease in aortic pulse pressure during inspiration in a manner analogous to the bedside finding of pulsus paradoxus.
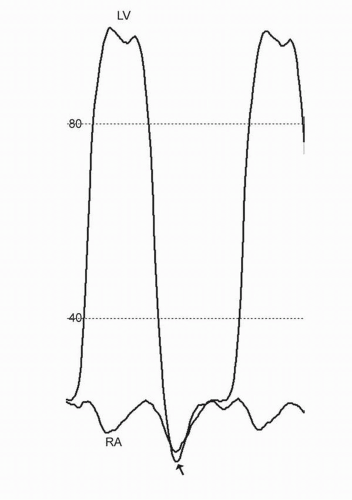 FIGURE 43-4 Early rapid ventricular filling. This figure illustrates the presence of early rapid ventricular filling and prominent y descents (arrow), which are a feature of constrictive pericarditis, restrictive cardiomyopathy, and other forms of heart failure. The preservation (or accentuation) of the y descent allows one to distinguish these entities from cardiac tamponade (see Figs. 43-2 and 43-3). LV, left ventricle; RA, Right artery. |
TECHNIQUE FOR PERICARDIOCENTESIS
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree