IMPLANTABLE DEVICE THERAPY FOR PROPHYLAXIS OF SUDDEN CARDIAC DEATH AND MANAGEMENT OF CONGESTIVE HEART FAILURE
Case presented by:
A 49-year-old male was admitted to the hospital with chest pain and shortness of breath in August 2008. He had noted dyspnea on exertion and decreased exercise tolerance for several years. He was clinically noted to have cardiomegaly and rales at both lung bases. Cardiac enzymes and ECG documented a non-ST-segment elevation myocardial infarction (MI). Cardiac catheterization showed a patent coronary stent and medical treatment was recommended.
The patient had a long history of hypertension and juvenile onset diabetes mellitus of 20 years duration. In 2006, he had an acute anteroseptal MI and underwent a percutaneous coronary intervention (PCI) procedure for revascularization with placement of an intracoronary stent. He had a history of chronic heart failure and prerenal azotemia. An echocardiogram showed moderate left ventricular (LV) dysfunction with an estimated ejection fraction (EF) of 30%, while monitoring and electrocardiography showed ventricular ectopics and nonsustained ventricular tachycardia (VT). He was referred for prophylactic implantable cardioverter-defibrillator (ICD) insertion for potential sudden cardiac death (SCD).
A.Prophylactic ICD insertion 40 days after discharge.
B.Prophylactic ICD insertion before hospital discharge.
C.Amiodarone.
D.None of the above.
Clinical Course
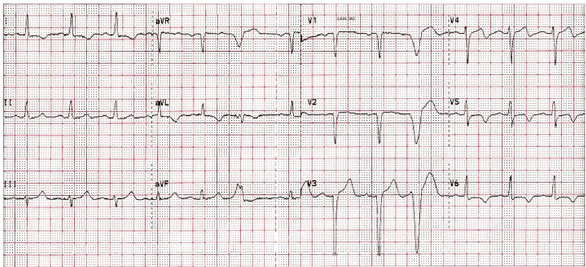
The patient was readmitted in October 2008. A preadmission ECG showed sinus rhythm with occasional premature ventricular contractions (PVC), QRS duration of 95 ms in sinus rhythm, healed anteroseptal MI QRS pattern, and a prolonged calculated QTc interval of 478 ms. Lateral T-wave inversions are consistent with ischemia (Figure 55.1). A gated blood pool scan showed LV dysfunction with a global EF of 40%. Electrophysiologic testing showed sinus rhythm with first-degree atrioventricular (AV) block, QRS duration of 130 ms, AH interval of 102 ms, and HV interval of 80 ms. Atrial extrastimulation showed further HV prolongation and intermittent intra-His block. Programed ventricular stimulation induced sustained monomorphic VT with a cycle length of 330 ms, right bundle branch block morphology, and was terminated by antitachycardia pacing (ATP) at 300 ms. A dual-chamber ICD was inserted. Five months later, sustained VT was terminated by ATP intervention from the ICD (Figure 55.2).
Figure 55.1. Sinus rhythm with evidence of a healed anteroseptal MI and lateral wall ischemia is present. Frequent PVC is noted.
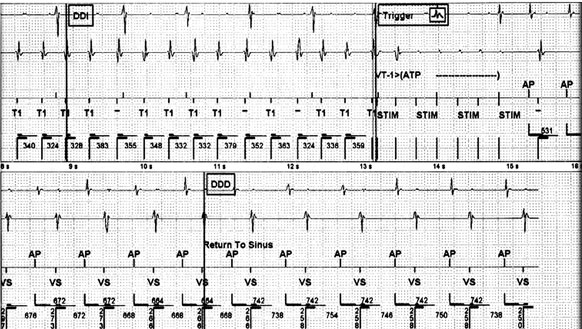
Figure 55.2. Spontaneous VT documented by intracardiac electrograms (EGMs) (upper panel) with a cycle length ranging from 324 to 379 ms is seen with AV dissociation. ATP commences (Trigger) and terminated the tachycardia. The patient returns to an atrial paced rhythm in the bottom channel. Upper panel: top EGM = right atrium; lower EGM = right ventricle (RV); top marker channel = interval and stimulation markers; bottom marker channel = ventricular events detection. Lower panel: top EGM = right atrium; lower EGM = RV; top marker channel = paced/sensed; bottom marker channel = A/V intervals.
A.It has no prognostic value after acute myocardial infarction (AMI).
B.MADIT II showed that frequency of ICD therapy delivery was not different in patients who had VT induced with noninvasive programed stimulation.
C.Moderate to severe reduction in left ventricular ejection fraction (LVEF) identifies all patients at risk for SCD after MI.
D.None of the above.
A.Depressed heart rate variability is a weak predictor of outcomes after AMI.
B.T-wave alternans during stress testing 6 weeks after MI is most predictive of the risk of sudden death when a patient can complete a maximal exercise test.
C.Induction of sustained VT > 10 days after AMI can predict recurrent VT, and ICD therapy can improve outcomes in these patients.
Question No. 4: In patients manifesting nonsustained VT after AMI and depressed LV function:
A.Immediate ICD placement is appropriate.
B.Beta-blocker therapy should be maintained.
C.Wearable defibrillator is an alternative to immediate ICD implant.
D.Amiodarone is the best choice.
Discussion
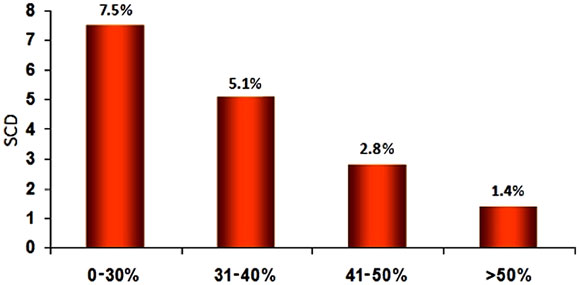
Patients with coronary artery disease make up the majority of ICD recipients in most studies. ICD implantation is accepted as reducing mortality and improving outcomes in patients with chronic ischemic heart disease. Patients with reduced LV function have increasing risk of sudden death with progressive impairment of ventricular function and have been shown to obtain greater benefit with ICD therapy than with drug therapy (Figure 55.3 and Table 55.1). A large number of clinical trials have demonstrated improvement in mortality with ICD therapy for secondary and primary prevention.
Figure 55.3. SCD incidences vary with degree of LV systolic dysfunction as assessed by EF. (Adapted from de Vreede-Swagemakers et al.7)
Table 55.1. ICD Therapy Clinical Trials
| Trial | Patients | Year | All-cause mortality | P value |
| AVID | 1016 | 1997 | 39% relative risk reduction Hazard ratio (HR) 0.62 | < 0.02 |
| CIDS |