Upper Extremity Embolic Disease
JUSTIN HURIE
Presentation
A 65-year-old woman, who had a cerebrovascular accident 6 weeks ago, presents to the emergency department with right upper extremity pain and numbness for 5 hours. She had been recovering well at home and had minimal residual right-sided weakness after her cerebrovascular accident. The patient notes having difficulty moving her right arm and has severe pain in her hand. Her past medical history includes tobacco use and hypertension. Her current medications included aspirin and hydrochlorothiazide. She has no prior history of a cardiac arrhythmia. On physical examination, her pulse is 120 beats per minute and irregular, and her blood pressure is 110/60 mm Hg. Her cranial nerves are intact, and she has no evidence of cerebral ischemia. Her right hand is cool, painful, and mottled. She has palpable left radial and brachial pulses. She has a strong right brachial pulse but has no arterial signal at her wrist when interrogated with a handheld Doppler. She has decreased strength and sensation in her right hand. Her abdomen is soft, and she has palpable femoral and pedal pulses in her legs.
Differential Diagnosis
The patient has evidence of upper extremity ischemia based on physical examination. Potential sources of upper extremity ischemia include the following:
1. Cardiac embolus
2. Acute on chronic upper extremity arterial disease
3. Embolus from a proximal aneurysm
4. Traumatic injury
5. Proximal dissection
Workup
The patient has evidence of a new cardiac arrhythmia, as well as acute limb ischemia (ALI). It is common for patients with ALI to have multiple acute and chronic medical problems that must be treated appropriately and contribute to a high short-term mortality rate. An electrocardiogram suggests atrial fibrillation without evidence of acute myocardial ischemia. Although the patient denies chest pain, a troponin level should be checked and may be trended in order to evaluate for underlying myocardial damage.
Approximately 80% of patients with ALI have an embolism from a cardiac source. Diagnostic tests, such as duplex, computed tomography angiography (CTA), and/or conventional arteriography, may be considered, but minimizing delay in treatment for severe ALI is essential. This patient needs prompt revascularization to keep the total ischemic time less than 6 hours in order to minimize the risk of permanent muscle and nerve damage. Arteriography with thrombolysis may be an option for patients with less advanced ischemia but may delay reperfusion that could be achieved more rapidly with surgery. Physical examination is critical to localize the site of occlusion in the setting of ALI. In the setting of normal contralateral perfusion, presence of a water-hammer pulse at the brachial artery on the affected limb suggests that she would be a good candidate for open brachial thromboembolectomy.
Diagnosis and Treatment
The patient should be started on full-dose intravenous (IV) heparin (100 U/kg bolus and 18 U/kg/h) to decrease the risk of recurrent cardiac emboli from atrial fibrillation. The patient’s heart rate is controlled with an intravenous beta-blocker. She is prepped for the operating room.
When the etiology of ALI is not as clear by history and physical examination, additional information may be gathered through performance of a CTA. CTA may further delineate the extent and level of embolism and be the best imaging modality to demonstrate an aneurysm. Conventional arteriography may provide an alternative option for diagnosis with the benefit of possible intervention. Arteriography only demonstrates luminal diameter so may not clearly show a proximal aneurysm. Due to the high level of spatial resolution, arteriography may demonstrate a subtle proximal lesion (Fig. 1).
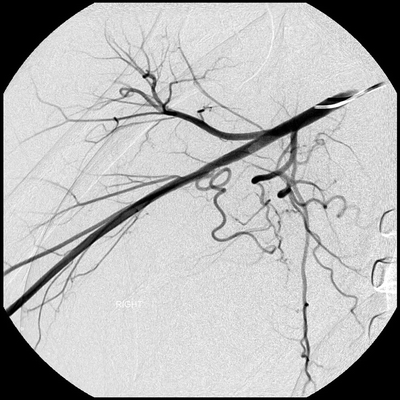
FIGURE 1 Angiography demonstrating a subtle proximal lesion involving the brachial artery.
Surgical Approach
The patient is taken to the operating room emergently (Table 1). Her right arm in entirety as well as one thigh are prepped and draped in the usual sterile fashion. The thigh may be interrogated with an ultrasound prior to prepping in order to assure access to the great saphenous vein should a bypass or vein patch be required. An open thromboembolectomy under local anesthesia with IV sedation may be performed if the patient is able to cooperate; otherwise general anesthesia may be required. The brachial artery may be exposed through a transverse or longitudinal incision. Care should be taken to avoid injury to the median nerve that courses with the brachial artery. Vessel loops may be used for proximal and distal arterial control and a transverse arteriotomy performed. A catheter embolectomy may be performed with 2- to 4-French Fogarty balloons based on the size of the vessel. The balloons should only be inflated while withdrawing the balloons in order to prevent injury to the vessel. The balloons should be passed until no additional thrombus is obtained and there is evidence of good inflow and adequate back bleeding. In this case, thrombus is extracted from the brachial artery, and the artery is repaired using interrupted 6-0 Prolene suture. The hand becomes pink, and the patient has a palpable pulse.
TABLE 1. Upper Extremity Embolectomy




