The role of the physical therapist in the community varies widely. Over the years, this role has changed in response to a range of factors, including epidemiological indicators of chronic conditions, advances in medical and surgical management, and policy changes. Lifestyle-related conditions and their associated comorbidity are health care priorities necessitating substantial community support, often for many years (Chapter 1). In addition, other chronic systemic conditions have well-documented cardiovascular and pulmonary consequences (Chapters 6 and 13). Policy changes during the 1980s resulted in the emergence of diagnostic-related groupings (DRGs), which led to patients being discharged from the hospital at more acute stages of illness. Further, the Balanced Budget Act of 19971 narrowed the criteria for those who qualified for prolonged inpatient postacute care, resulting in patients being transitioned home from extended care facilities sooner than they had been previously. The combination of these factors has changed the role of physical therapy in the community. Physical therapy is provided in all inpatient care settings, including subacute hospitals, Medicare or another form of insured care skilled nursing settings, long-term acute care facilities, and rehabilitation facilities with transitional care units to facilitate functional progression so that patients are able to return home within days or weeks. Thus rehabilitation, by increasing the number of patients who return home, rather than remaining or being placed in facilities, is a way of reducing cost while maintaining care standards.2 Changes in health care reimbursement from third-party payers affect patients’ access to physical therapy services. Although such policy may be viewed as reducing physical therapy access, new paradigms of health care delivery and models of care for people with chronic conditions may emerge. Epidemiological indicators support patient-centered health care delivery systems and self-care and self-management approaches. The incorporation of self-management principles of practice can improve patients’ quality of life and decrease hospitalization.3–14 This chapter describes how physical therapists can facilitate the management of chronic conditions, particularly lifestyle-related conditions, when practicing in the community and home settings. Because of dramatic increases in both patient longevity and prevalence of chronic illness, physical therapists see an ever-widening range of diagnoses in their patients in the community. Global aging is occurring at an unprecedented pace. Worldwide, the number of people age 65 and older is expected to increase from 500 million to 1 billion by 2030.15 Physical therapist interventions unique to aging populations need to be considered in relation to the available resources, as well as the challenges that present in the community practice setting more often now that patients are living longer (Chapter 38). Chronic conditions that were previously associated with later stages in life are now presenting earlier in life as a result of changing lifestyle behaviors (Chapter 1). Also, the medical community has improved its ability to quickly and effectively manage complicated acute medical situations—premature births, heart failure, cancer. More patients are surviving diseases once considered fatal and consequently requiring more services to safely and effectively manage the morbidity issues that result. Medical interventions in intensive care units have improved greatly, thus decreasing mortality, but morbidity related to myopathy of critical illness, cognitive impairments, and mental health sequelae has been found to have a significant impact on patients’ ability to resume their prior level of independence (Chapters 33–36).16–21 These patients return home more often and more quickly than in the past, but they often do so accompanied by unresolved cardiovascular and pulmonary impairments. For patients who are too medically fragile to return home or to obtain sufficient medical care at skilled nursing facilities, specialty hospitals have become necessary. These hospitals make it possible for ventilator-dependent or ventilator-assisted patients to receive physical therapy longer and at less cost than an acute care hospital.22 Practicing physical therapy in the community is distinct from practicing in acute care. When people with chronic conditions are living in the community, their focus is on health promotion and optimal health, rather than recovery from an acute episode of a condition or surgical procedure or trauma with frequent changes in their functional status, as is seen in acute care. In the community setting, the patient’s goals are less focused on safety and more on optimal health. Patients’ participation is vital in order to understand their definition of optimal health. Consistent with values of autonomy and independence, shared decision making should always be used— including the patient and family/caregiver in decisions regarding the patient’s care with guidance from the health care team.14,23 This model is at times challenging for health care team members who may feel more comfortable continuing to use a method in which they prescribe a task and tell the patient what to do, with little collaboration. However, the expected level of practice of every physical therapist is evidence-based practice (EBP) in decision making and treatment. The three aspects of EBP are weighted comparably: external clinical evidence, patient circumstances, and individual clinical expertise.24 In this approach to practice, the patient’s goals and his or her ability to carry out an effective plan are important. A patient cannot carry out an effective plan unless he or she is taught how to identify problems and manage or avoid them in daily situations when health care professionals are not present. Patients need a targeted and tailored education to understand how to make the best decisions about their health and to appreciate their responsibility in their own health management. Many people at home or in long-term care have chronic conditions, often related to lifestyle behaviors. Regardless of whether these conditions are the diagnoses for which they are receiving physical therapy, the related activity limitations and participation restrictions can limit their abilities to participate and progress in their therapy. Chronic conditions can affect the person’s physical capabilities, as well as his or her emotions, attitude, and motivation. Many patients with chronic conditions or functional decline lead full and rewarding lives, but doing so requires the active participation of the patient and the physical therapist to maintain the fullest level of function despite the changes. The choices patients make about their health care, exercises, and methods of self-management will largely determine their health-related quality of life (Chapter 1). Though people with chronic conditions have multiple impairments requiring adaptation of their lifestyles and schedules, the majority still accomplish what they want and need to do each day. The goal is to augment their knowledge about their symptoms and enable them to work within a collaborative, self-advocacy, and self-help model with their health care team to achieve optimal health. Positive self-management involves a combination of positive emotional outlook, active involvement in decision making, and maintenance of a lifestyle that is as optimal as possible. The interprofessional team needs to engage the patient in his or her care decisions. The physical therapist needs to be caring and fully present with the patient. Although the physical therapist can provide the initial stimulus for the process, effective self-management comes only from within the patient. The physical therapist can continue to be a resource and provide interventions as needed, but the goal is for the patient to be his or her own case manager and decision maker, whenever possible, regarding health care and optimal function (Chapter 1).14,23 Actively playing a role in decision making (i.e., self-management) empowers patients, making them more motivated, positive, active, and successful than passive patients who do only what the physical therapist and other health professionals advise.23,25 A decrease in the number of visits allowed by third-party payers has forced a necessary change towards patient self-management and empowerment, which has led to improved efficiency and effectiveness in treatment. The promotion of positive self-management strategies for a more active, healthy lifestyle is one of the most important competencies of contemporary physical therapists. The physical therapist facilitates this process by being caring, supportive, and respectful of patient goals and priorities. This has been referred to as a “healing presence,” which may lead to a beneficial, therapeutic, positive experience for the patient.26,27 The American Physical Therapy Association promoted this practice philosophy with the phrase “the science of healing, the art of caring.” One example is a patient with coronary artery disease, who is fully independent in his or her day-to-day activities but not at a maximal functional level because of limited education on how to further improve function. Another example is a patient who cannot resume his or her prior level of independent function after an acute bout of illness or hospitalization because of limits resulting from primary and/or secondary cardiovascular and pulmonary dysfunction. Both of these examples illustrate the resultant decrease in such patients’ tolerance for, and ability to independently perform, activities of daily living. Because of these decreases, patients must acquire continued support to maintain their safety and improve their level of function. Those with the least ability to care for themselves after an acute bout of illness transfer into nursing homes or alternative long-term care, and those with higher levels of function move into assisted living facilities or return home with assistance and therapy. Such patients may present with decreased strength, endurance, and balance, leading to decreased independence, mobility, and activity level. Returning home with a decrease in independent functioning may be associated with negative emotions, which may further decrease appetite, activity level, motivation, and social/community interactions (Chapter 1). Functioning depends on the ability of the patient to maintain all of the components of oxygen transport to support activity. One example is a patient who fell in the parking lot of a hospital where she had been attending a pulmonary rehabilitation program. She was fitted with a long leg cast and discharged home. She reported being short of breath with sit-to-stand transfers, and soon she was hardly able to ambulate across the room with the standard walker she used before. When the physical therapist observed this patient using her bronchodilator metered-dose inhaler, she was using it improperly. After she was instructed on how to use the bronchodilator therapy effectively before activity, the patient’s transfers and her walking ability improved markedly. She was able to coordinate her breathing with her activity, and her endurance further improved. Case reports and professional experiences such as this provide important information for the physical therapist to use in conjunction with the findings of research studies when planning and prescribing interventions for patients at home using evidence-based practice.24 The patient’s ability to participate in therapy may be driven by multiple system impairments. Nutritional concerns are a priority. It is important to monitor whether the patient is losing or gaining weight. Poor denture fit and the impact of medications on taste and appetite can affect the patient’s ability to eat. The patient may be depressed, also limiting appetite. The patient may not want to drink because of difficulty getting to the bathroom independently. Determine whether the patient is taking a diuretic and whether he or she has urinary incontinence. Patients who have difficulty managing urination because of frequency or urgency may be less likely to drink sufficient fluids, increasing the risk for hypovolemia, hypotension, decreased cerebral perfusion, and falls.28 Functional gains may be achieved sooner when physical therapy is incorporated into the patient’s daily living with the help of the nurses and aides. This can improve physical capabilities by aiding the learning process, as well as increasing the number of repetitions performed for motor planning. For example, if the patient is taught to use ventilatory strategies with movement, such as inspiring when extending the trunk (Chapter 23), this should be communicated to other caregivers and encouraged during movements that extend the trunk, such as dressing. If the goal is for the patient to walk to meals, the physical therapist and caretakers can have the patient transition from walking as far as he or she can toward the dining room for one meal each day, then walking to two meals each day, and finally, to all meals. The next progression would be to set more functional goals, such as walking to daily activities, to social settings, to the car, and so on; thus walking is no longer associated only with therapy. In-services for nurses and care staff that help reinforce physical therapy interventions can be conducted individually and in formal classes. Instruction can be incorporated into the staff competencies upon hire and annually. One-on-one therapist/aide education sessions should not be replaced by the competencies; rather, they should occur as needed when unique patient needs arise. Educational opportunities such as this can help to make patient education more consistent.
The Patient in the Community
Chronic Conditions and Self-Management
Cardiovascular and Pulmonary Concerns in the Community
Long-Term Care Facilities and Nursing Homes
Thoracic Key
Fastest Thoracic Insight Engine

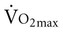 can be attributed to labored breathing, which places considerable metabolic demand on the patient simply to breathe, let alone the challenge of pausing breathing to eat. A nutrition consult can be initiated to assess the patient’s caloric intake and supplement this intake if indicated.
can be attributed to labored breathing, which places considerable metabolic demand on the patient simply to breathe, let alone the challenge of pausing breathing to eat. A nutrition consult can be initiated to assess the patient’s caloric intake and supplement this intake if indicated.

