Fig. 4.1
Formation of QRS vector loop. (a) Divide the ventricular depolarization into nine parts, record the amplitude and direction of the instantaneous complex vector; (b) Draw a line to connect the termination of the vectors together in proper order and you get a QRS vector loop
Since the number and the position of the myocardial cells involved in the depolarization are constantly changing, the length and direction of the instant resultant vector vary at different moment of the ventricular depolarization. If we draw a line to connect the termination of the vectors together in an order, or record the process of the changes, we can get a curve, a vector loop in three-dimensional spaces (special QRS vector loop).
4.1.3 Formation of Normal QRS Complex in Limb Leads
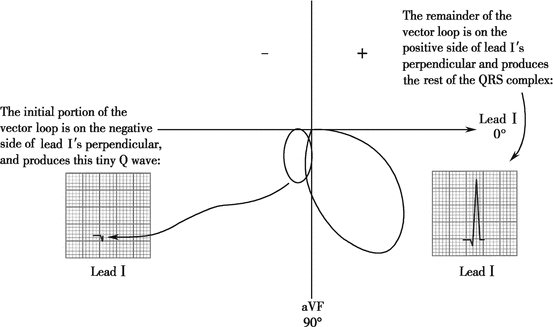
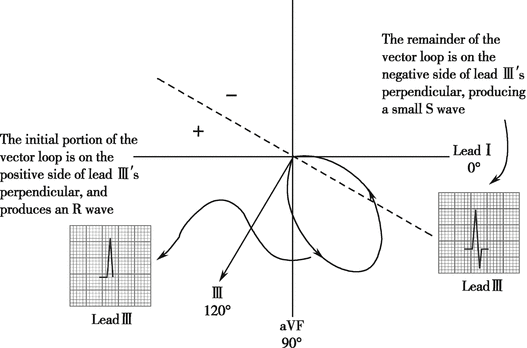
If we placed the QRS vector loop into hexaxial reference system that we’ve learnt before, we could easily understand the morphology of QRS complex in limb leads (Figs. 4.2, 4.3, 4.4, and 4.5).
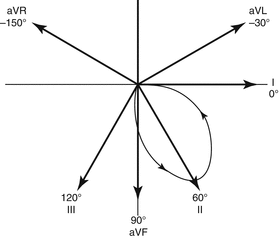

Fig. 4.2
Projection of QRS vector loop on axes in hexaxial reference system
Similar to the QRS complex in all limb leads, we can understand QRS complex in all six chest leads when the vectors in QRS vector loop are projected on chest lead axes (Fig. 4.6).


Fig. 4.6
QRS vector loop projected on chest lead axes (a) and QRS complex waveform in chest leads (b)
4.2 Abnormal QRS Complex
4.2.1 Abnormalities in QRS Complex Axis
The direction of ECG axis is usually measured by the angle between the axis and the positive direction of lead I axis. The diagnosis recommended by WHO guideline regarding electric axis is as follows:
[Axis Deviation] (Fig. 4.7)

Fig. 4.7
Axis deviation
−30° to +90°, no axis deviation; −30° to −90°, left axis deviation; +90° to +180°, right axis deviation; −90° to −180°, uncertain axis (axis of “no man’s land”)
To determine axis deviation, we should mainly focus on leads I and aVF.
4.2.1.1 No Axis Deviation
[ECG Recognition]
1.
The cardiac electric axis lies between −30° and +90°.
2.
Two common variants:
① Main wave is positive in both leads I and aVF (Fig. 4.8a): for the main wave in lead I is positive, the QRS axis is in the positive direction of lead I axis, that is, in the first or forth quadrant (of the frontal plane). For the main wave in lead aVF is positive, the QRS axis is in the positive direction of lead aVF axis, in other words, in the third quadrant or forth quadrant. Therefore, the QRS axis lies in the forth quadrant.
(0° to +90°). It is no axis deviation.
② The main wave is positive in leads I and II and negative in lead aVF (Fig. 4.8b): for the main wave in lead I is positive, the QRS axis is in the positive direction of lead I axis, that is, in the first or forth quadrant; for the main wave in lead aVF is negative, the QRS axis is in the negative direction of lead aVF axis, that is, in the first or second quadrant. Therefore, the QRS axis lies in the first quadrant.
(0° to −90°). Since the main wave is positive in lead II, the QRS axis is within 0° to −30°; in other words, it is no axis deviation.
[ECG Tracing] (Fig. 4.8)
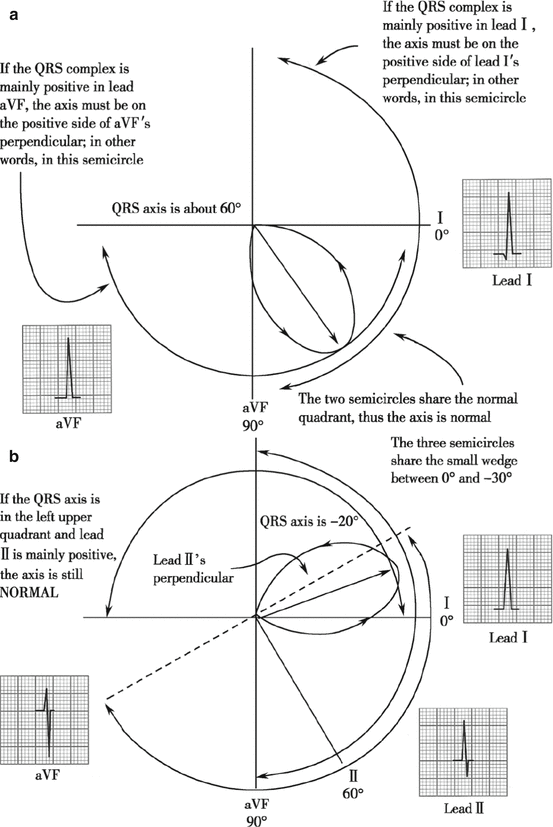
Fig. 4.8
Determination of no axis deviation. (a) Positive main wave in aVF; (b) negative main wave in aVF
4.2.1.2 Left Axis Deviation
[ECG Recognition]
1.
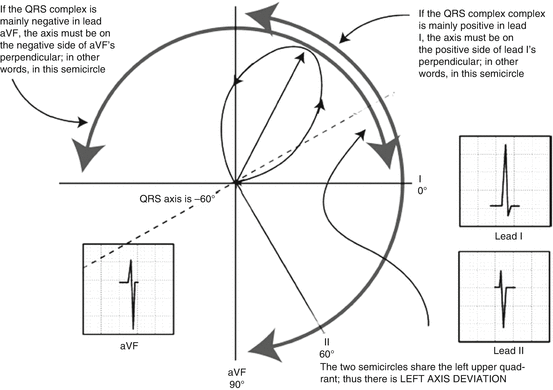
The angle of cardiac electric axis lies between −30° and −90°.
2.
The main wave is positive in lead I and negative in leads aVF and II. For the main wave in lead I is positive, the QRS axis is in the positive direction of lead I axis, that is, in the first or forth quadrant. For the main wave in lead aVF is negative, the QRS axis is in the negative direction of lead aVF axis, that is, in the first or second quadrant. Therefore, the QRS axis lies in the first quadrant (0° to −90°). Since the main wave is negative in lead II, the QRS axis is within −30° to −90°; in other words, it is left axis deviation.
4.2.1.3 Right Axis Deviation
[ECG Recognition]
1.
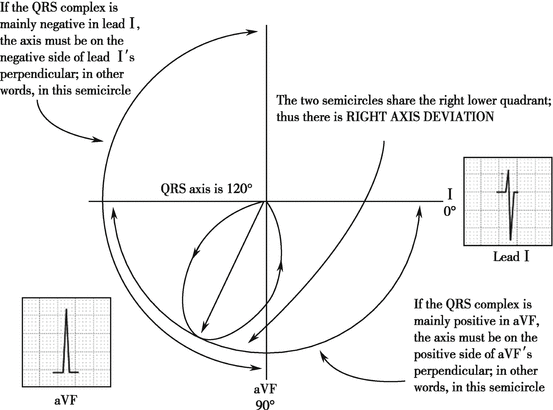
The cardiac electric axis lies between +90° and +180°.
2.
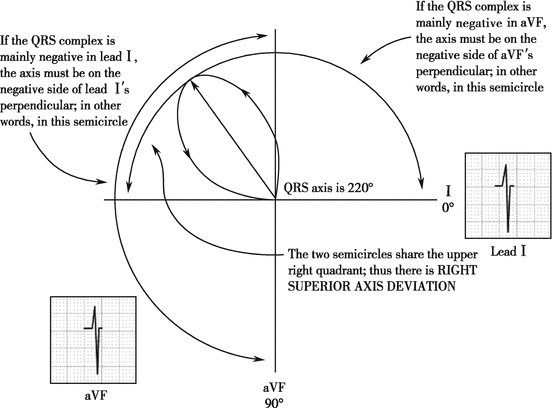
The main wave is negative in lead I and positive in lead aVF. For the main wave in lead I is negative, the QRS axis is in the negative direction of lead I axis, that is, in the second or third quadrant. For the main wave in lead aVF is positive, the QRS axis is in the positive direction of lead aVF axis, that is, in the third or fourth quadrant. Therefore, the QRS axis lies in the third quadrant (+90° to +180°). It is right axis deviation.
4.2.1.4 Uncertain Axis (No Man’s Land)
[ECG Recognition]
1.
The cardiac electric axis lies between −90° and −180°.
2.
The main wave is negative in leads I and aVF. For the main wave in lead I is negative, the QRS axis is in the negative direction of lead I axis, that is, in the second or third quadrant. For the main wave in lead aVF is negative, the QRS axis is in the negative direction of lead aVF axis, that is, in the first or second quadrant. Therefore, the QRS axis lies in the second quadrant (−90° to −180°). It is uncertain axis.
4.2.2 Abnormalities in QRS Complex Voltage
4.2.2.1 Excess QRS Voltages (High QRS Voltages)
Left Ventricular Hypertrophy
[ECG Recognition]
1.
QRS voltage changes: RV5 or RV6 voltage is greater than 2.5 mV; RV5 + SV1 is greater than 4.0 mV (for female is greater than 3.5 mV); RI voltage is greater than 1.5 mV; RI + SIII is greater than 2.5 mV; RaVL voltage is greater than 1.2 mV or RaVF voltage is greater than 2.0 mV.
2.
Prolonged QRS complex duration: QRS complex duration prolonged to 0.10–0.11 s but still less than 0.12 s.
3.
Left axis deviation: most patients with left ventricular hypertrophy show mild or moderate left axis deviation.
4.
Secondary ST-T change: in leads where the R wave predominates in the QRS (such as the left chest leads), the ST segment depression is greater than 0.05 mm with flat, biphasic, or inverted T wave; while in the leads where the S wave predominates (such as right chest leads), ST segment elevation can correspondingly appear with tall upright T wave. An increased QRS complex voltage with ST-T change is left ventricular hypertrophy with strain.
Right Ventricular Hypertrophy
[ECG Recognition]
1.
QRS complex morphology change: QRS complex shows qR pattern in V1, R/S is greater than 1 in leads V1 and aVR; R/S is less than 1 in lead V5; evident clockwise transposition can be seen, and QRS complex shows rS pattern from V1 to V4, even to V6 sometimes.
2.
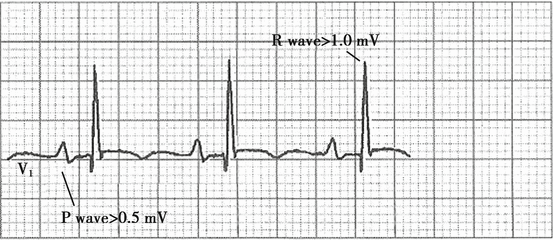
QRS complex voltage changes (Fig. 4.14): QRS complex voltage increases; voltage in RV1 is greater than 1.0 mV; RV1 + SV5 is greater than 1.2 mV; RaVR is greater than 0.5 mV.
3.
Right axis deviation.
4.
ST-T change: ST segment is depressed with biphasic or inverted T wave in V1. Tall R wave in lead V1 with ST-T change is defined as right ventricular hypertrophy with strain.
4.2.2.2 Low Voltage in QRS Complex
Common causes:
1.
Low voltage caused by myocardium: restrictive cardiomyopathy (amyloidosis, sarcoma, etc).
2.
Increased impedance between tissues (myocardium) that forms voltage and leads: fat (overweight), air (COPD, pneumothorax), and water (pericardial or pleural effusion, ascites).
3.
Hypothyroidism.
[ECG Recognition]
1.
No absolute voltage value of any QRS complexes in any chest leads ≥0.8 mV (8 mm)
2.
Or no absolute voltage value of any QRS complexes in any limb leads ≥0.5 mV (known as low voltage in limb leads)
4.2.3 Wide QRS Complex
Wide QRS complex has a duration greater than 0.12 s. Common causes include premature ventricular contraction, ventricular escape, implantation of artificial cardiac pacemaker, WPW syndrome, bundle branch, or fascicular block. Electrolyte and acid–base balance disturbances may also be included.
4.2.3.1 Premature Ventricular Contraction (PVC)
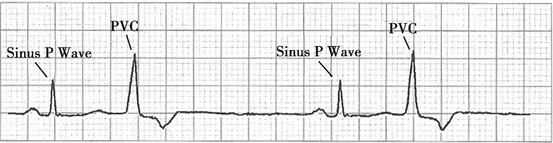
[ECG Recognition]
1.
QRS complexes have wide (>0.12 s in adults and >0.10 s in children) and bizarre appearance. T wave and QRS complex are in the opposite direction.
2.
No corresponding P waves are present before PVC.
3.
Retrograde P′ wave may appear after the QRS complex and R-P′ > 0.20 s.
4.
Usually PVC is followed by a full compensatory pause. However, a noncompensatory pause is also possible.
4.2.3.2 Ventricular Escape
[ECG Recognition]
1.
In combination with bradycardia, the delayed QRS wave is wide (>0.12 s in adults and >0.10 s in children) and bizarre. T wave and QRS complex are in the opposite direction.
2.
No corresponding P wave is present before the escape beat.
4.2.3.3 ECG Recognition with Artificial Cardiac Pacemakers
An artificial cardiac pacemaker (Fig. 4.18) is composed by a power source that generates regular, timed stimuli (the heart is stimulated by the electric current which is depicted as spike in ECG) and electrodes (can be classified into unipolar electrode with more stimulation and bipolar electrodes with less stimulation).
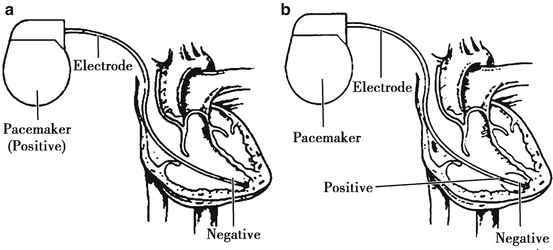

Fig. 4.18
Pacemaker with unipolar electrode and pacemaker with bipolar electrode. (a) Pacemaker is positive, electrode is negative; (b) electrodes have both positive and negative side
According to different principles, pacemakers can be divided into single-chamber pacemaker that has one lead placed in the heart and paces either right atrium or ventricle; dual-chamber pacemaker that has one lead placed in the right atrium and the other in the right ventricle, cardiac resynchronization therapy (CRT); or triple-chamber pacemaker that adds one more lead to the coronary sinus (Fig. 4.19).
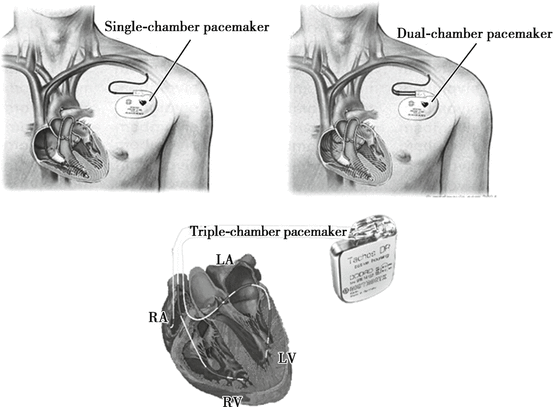

Fig. 4.19
Pacemakers
An international code called NBG code can be used to identify most of the pacemaking system, where A stands for the right atrium, V stands for the right ventricle, D stands for dual, O stands for none, I stands for inhibiting pacing, and R stands for triggering pacing.
The first letter describes the chamber paced (A, V, D).
The second letter describes the chamber sensed (A, V, D, or O).
The third letter describes the response to sensing (I, R, D, or O).
The forth letter describes the programmable functions.
4.2.3.4 Right Ventricle Pacemaker
Right ventricle pacemaker, otherwise called ventricular inhibited pacing (VVI), is the most common type of pacemakers, in which the electrode is usually placed in the apex (Fig. 4.20). This electrode can sense electrical activities in the right ventricle. If electrical activities by the heart itself are sensed, the pacemaker is inhibited. Otherwise, the pacemaker will pace the ventricle after a preset interval.
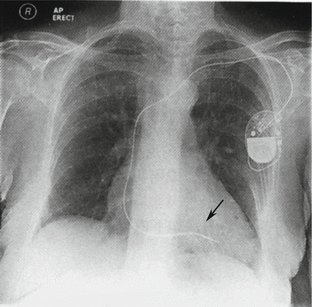

Fig. 4.20
X-ray shows right ventricle pacemaker that has been implanted under the left shoulder. The electrode passes through the subclavian vein while its head end in the apex
Indications for VVI pacemakers:
Slow ventricular rates or atrial fibrillation that causes asystole
Sinoatrial node diseases
Atrial ventricular block
Drawback: artificially atrioventricular dyssynchrony
[ECG Recognition]
1.
The spike is followed by a wide QRS complex which resembles left bundle branch block.
2.
The pacemaker spike is big in unipolar pacing while small in bipolar pacing.
3.
If electrical activities by the heart itself are sensed by the pacemaker, the impulse is inhibited in a preset interval. Intermittent pacing will be showed on ECG as non-equal ventricle pacing rhythm and patients’ own rhythm.
[ECG Tracing] (Fig. 4.21)

Fig. 4.21
Ventricular pacemakers. (a) Unipolar pacing in VVI (the pacemaker spike is big); (b) bipolar pacing in VVI (the pacemaker spike is small)
4.2.3.5 Right Atrium Pacemaker
Right atrium pacemaker is also known as atrial-inhibited pacing (AAI). This is a relatively rare type. The electrode is placed in the right atrium, usually the right auricle (Figs. 4.22 and 4.23). The pacemaker can sense patients’ own electrical activities in the right atrium. If the rate of sinus pulse is higher than the preset level, the pacemaker is inhibited. Otherwise, the pacemaker will work continuously.
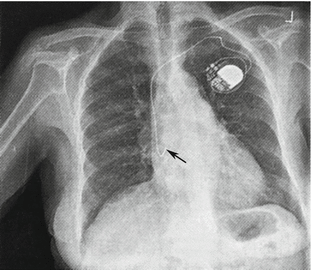

Fig. 4.22
X-ray shows the right atrium pacemaker that has been implanted under the left shoulder. The electrode passes through the subclavian vein while its head end in the right auricle
Indications for AAI pacemakers:
Sinoatrial node dysfunction without atrial ventricular node diseases
Young patients with history of carotid sinus syncope
Drawback: not suitable for patients with severe atrial ventricular block
[ECG Recognition]
1.
The spike is followed by a sinus P wave.
2.
The P-R interval and QRS complex are usually normal, indicating the atrial ventricular node is functioning well.
3.
If the pacemaker can sense patients’ own electrical activities, the pacemaker is inhibited during the preset interval, showing intermittent pacing on ECG.
[ECG Tracing] (Fig. 4.23)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree