Parameter
Score
0
1
2
Respiratory sounds
None
Rough
Delayed
Stridor
None
Inspiratory
Biphasic
Cough/voice
None
Dysphonic cry
Canine cough
Retraction
None
Suprasternal
1 + intercostal
Cyanosis
None
With air
With 40% O2
Level of consciousness
Normal
Lethargic
Obtunded
Indications for Airway Endoscopy
A severe stridor generally goes hand in hand with significant airway obstruction. It is important to know how much air the patient is moving. If there is no movement of air through the airway, because of a severe obstruction, the symptom of a stridor will not be noticeable. Whenever possible, flexible endoscopy should be considered as a first step in assessing the larynx in any patient with a moderate to severe stridor. This test can provide the diagnosis, and a rigid endoscope can be used if necessary.
The best way to make a good assessment is with laryngoscopy or with flexible or rigid bronchoscopy prior to endotracheal intubation, because afterward the opportunity for a good diagnosis decreases.
If the stridor and airway obstruction are progressive—and to this can be added a weight increase and difficulty in feeding—rigid endoscopy is generally indicated not only for diagnosing the pathology but also with the aim of applying immediate treatment. For example, this can occur with laryngomalacia.
Endoscopy is often complemented with x-rays, while computerized axial tomography can also be useful when the endoscopic study suggests the presence of an abnormality, such as a vascular ring. In children with symptoms of severe obstruction, radiographic or magnetic resonance tests that require sedation should not be done before the diagnosis has been established by means of rigid endoscopy. As with the diagnosis of a foreign object, upper airway lateral and anteroposterior plaques do not provide sufficient resolution to rule out a large number of common pathologies. Consequently, direct visual observation by flexible or rigid endoscopy is more useful than imagery for assessing the airway in pediatrics.
When Is Rigid Endoscopy, Rather than Flexible Endoscopy, Appropriate?
Rigid and flexible endoscopy are complementary. Flexible endoscopy is used to examine the larynx of a child who is awake, and it allows useful information to be obtained about cordal mobility and laryngeal dynamics.
Lesions in the pharynx and lower airway can be viewed only with rigid endoscopy. If necessary, with general anesthesia after suspension of the larynx, the vocal cords can be viewed with a binocular microscope, providing a stereoscopic view. Rigid endoscopy allows for a good and detailed view, while control of the airway is maintained. Flexible bronchoscopy does not allow for absolute control of the airway and can obstruct it entirely in small children. The quality of the image with a rigid Hopkins rod-type telescope is superior to that obtained with a flexible bronchoscope, and its documentation is undoubtedly much clearer.
Rigid Instruments
- 1.
Laryngoscopy and bronchoscopy
- 2.
Documentation and teaching
Laryngoscopy and Bronchoscopy
Laryngoscopes
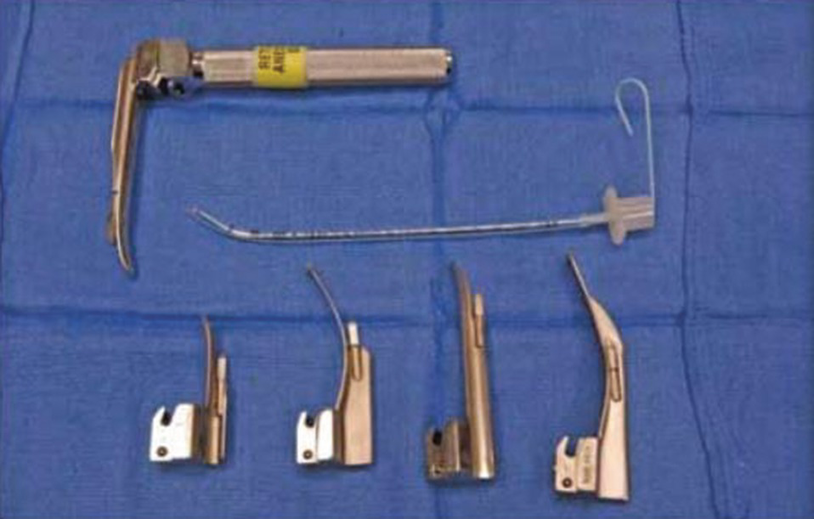
Laryngoscopes for intubation
Bronchoscopes
Telescopes
In 1966, Hopkins introduced the long telescope with different lenses, which improved the resolution and the angle of viewing, and revolutionized pediatric bronchoscopy, providing the potential to see into very small spaces. For example, a 4.0 mm by 20 cm zero-degree telescope is ideal for passing through a laryngoscope in the subglottis or trachea.
A Hopkins rod telescope alone (bare) or with a ventilating bronchoscope can be used for rigid assessment of the upper airway. Both visualize the larynx, trachea, and bronchi with magnification. The advantage of using the telescope alone is that it minimizes the trauma to the airway walls, given that the diameter of the endoscope is less than that of the ventilating bronchoscope. The diameters of Hopkins rod telescopes (the most widely used) are 1.9, 2.7, and 4 mm, while the lengths vary. There are also lenses with 30- and 70-degree angles. When a bare telescope is used, the patient cannot be actively ventilated, and so the endoscopy is usually conducted under spontaneous ventilation (see below for more information on this).
- 1.
Connection of a closed gas system to the anesthesia circuit so that the bronchoscope also acts as an endotracheal tube, which can serve to provide spontaneous ventilation and positive ventilation

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


