Studies comparing gender-specific outcomes in patients with atrial fibrillation (AF) have reported conflicting results. Gender differences in cerebrovascular accident/systemic embolism (CVA/SE) or major bleeding outcomes with novel oral anticoagulant (NOAC) use are not known. The goal of this analysis was to perform a systematic review and meta-analysis evaluating gender differences in residual risk of CVA/SE and major bleeding outcomes in patients with nonvalvular AF treated with either warfarin or NOAC. Sixty-four randomized studies were identified using keywords “gender,” “AF,” and “CVA.” Using the Preferred Reporting Items for Systemic Reviews and Meta-analysis method, 6 studies met criteria for inclusion in this meta-analysis. CVA/SE and major bleeding outcomes were separately analyzed in cohorts receiving warfarin and NOAC agents, comparing men with women. Women with AF taking warfarin were at a significantly greater residual risk of CVA/SE compared with men (odds ratio 1.279, 95% confidence interval 1.111 to 1.473, Z = −3.428, p = 0.001). No gender difference in residual risk of CVA/SE was noted in patients with AF receiving NOAC agents (odds ratio 1.146, 95% confidence interval 0.97 to 1.354, p = 0.109). Major bleeding was less frequent in women with AF treated with NOAC. In conclusion, women with AF treated with warfarin have a greater residual risk of CVA/SE and an equivalent major bleeding risk, whereas those treated with NOAC agents deemed superior to warfarin are at equivalent residual risk of CVA/SE and less major bleeding risk compared with men. These results suggest an increased net clinical benefit of NOAC agents compared with warfarin in treating women with AF.
Atrial fibrillation (AF) is the most common sustained arrhythmia in developed nations. The incidence and prevalence of AF are increasing both in the United States and across the world. Despite greater prevalence of AF among men, studies have shown that the risk of cerebrovascular accident (CVA) and systemic embolization (SE) is greater among women compared with men. A 2.5-fold increase in the prevalence of AF is projected by the year 2050, likely to affect nearly 5.6 million Americans. In nonanticoagulated patients with AF, female gender is an independent risk factor for CVA/SE. This is reflected in the recently validated CHADS 2 -VASc scoring system. Data on gender differences in efficacy of warfarin for stroke prevention are conflicting. NOAC theoretically provide a more stable anticoagulant effect ; however it remains unclear if this pharmacokinetic advantage translates into an outcome benefit. Gender differences in CVA/SE outcomes with NOAC agents are largely unknown. We sought to analyze gender differences in the residual risk of CVA/SE and major bleeding in patients with AF treated with warfarin and NOAC and evaluate effect size of the point estimates, in a pooled sample from randomized trials reported in the published literature.
Methods
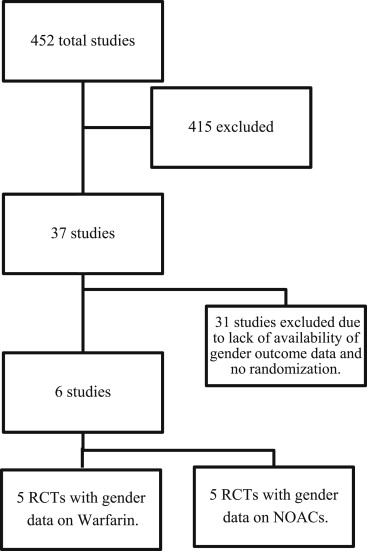
Using the keywords “atrial Fibrillation,” “gender,” “anti-coagulation,” and “outcomes,” we searched indexed studies recorded in major databases including PubMed, EMBASE, Cochrane Library, and Google Scholar. The method outlined in the Preferred Reporting Items for Systemic Reviews and Meta-analysis document was used. A total of 452 relevant studies were identified on search using these databases and reviewed independently by 4 investigators to check if they met inclusion criteria. We included all randomized trials of AF with data on gender and anticoagulation with the composite end point of all stroke and systemic embolization at ≥1 year. All identified studies were screened initially by the title and abstract, and 37 prospective studies were identified. Two sets of analyses were performed: first set of analyses evaluating gender differences in patients treated with warfarin and second set analyzing gender differences in patients treated with NOAC. After a detailed review of trials, a total of 6 randomized controlled trials met inclusion criteria. Five randomized controlled trials reported gender-specific outcome differences in warfarin-treated patients. Gender-specific outcome data on patients treated with NOAC was pooled from the NOAC arm of 4 randomized controlled trials comparing warfarin and NOAC and 1 study reporting gender-specific data on patients treated with NOAC or aspirin. The gender-specific data for patients treated with apixabanin in that trial were included in this analysis and data from the aspirin arm was not used in the analysis. Figure 1 depicts the flow of study evaluation (inclusion and exclusion) process. Using a standardized data collection form, the data were independently abstracted. Any discrepancies in data were resolved through a review and consensus. Baseline characteristics for both study groups were extracted from the studies. The absolute number of the composite end point events was used for analysis. Comprehensive Meta-Analysis software (Biostat, Englewood, New Jersey) was used to perform the analysis. Heterogeneity was assessed using the I 2 test, and an I 2 of <25% was considered consistent with low heterogeneity. All results were reported as odds ratios (ORs) and 95% confidence intervals (CIs). Publication bias was evaluated using Eggers method, and funnel plots were generated.
A pooled analysis of differences in event rates of CVA/SE between men and women treated with warfarin was performed. A primary analysis of differences in CVA/SE event rates between men and women treated with those agents that met superiority (in either intent-to-treat analysis or per-protocol analysis) compared with warfarin in the published literature was performed.
A pooled analysis of gender differences in major bleeding, defined using International Society of Thrombosis and Hemostasis definition was performed for the cohorts treated with warfarin and NOAC agents deemed superior to warfarin.
Results
A total of 6 studies met inclusion criteria. Baseline characteristics of patients from the included trials are listed in Table 1 .
| Study | Study Design | Number of Patients | Patient Characteristic | ||
|---|---|---|---|---|---|
| Mean Age (yrs) | Men (%) | CHADS 2 Score (%) | |||
| BAFTA | RCT, open-label, warfarin vs aspirin | 973 | 81.5 | 54.4 | 1–2 (72) |
| SPORTIF III/V | SPORTIF V, double-blind ximelegatran vs warfarin | SPORTIF III (3,410) and SPORTIF V (3,922) | 71 | 69.2 | NA |
| RE-LY | RCT, blinded, dabigatran vs unblinded warfarin | 18,113 | 71 | 63.6 | 2.1 (mean) |
| ROCKET-AF | RCT, double-blind rivaroxaban vs warfarin | 14,264 | 73 | 60.3 | 3.5 (mean) |
| ARISTOTLE | RCT, double-blind apixaban vs warfarin | 18,201 | 70 | 64.7 | 2.1 (mean) |
| AVERROES | RCT, double-blind, apixiban vs aspirin | 5,599 | 70 | 58.5 | 0–2 (72) |
Five studies reporting gender-specific annualized event rates of CVA/SE in patients with AF treated with warfarin prophylaxis were included in the first analysis. The pooled sample consisted of 26,260 patients, with 16,760 men and 9,500 women. A total of 478 men (2.85%) and 349 women (3.67%) developed CVA/SE. The forest plot demonstrating the differences in CVA/SE event rates between the 2 genders is shown in Figure 2 . Women had a significantly greater residual risk of CVA/SE compared with men while on anticoagulation therapy using warfarin (OR 1.279, 95% CI 1.111 to 1.473, Z = −3.428, p = 0.001). Heterogeneity was low with I 2 = 0. No significant publication bias was present, with 2-tailed p = 0.12, using Egger regression intercept method.
Analysis of a pooled sample from 4 studies reporting gender-specific annualized event rates of CVA/SE in patients with AF treated with NOAC showing superiority to warfarin prophylaxis was performed. The pooled sample consisted of 26,791 patients with 16,329 men and 10,462 women. A total of 345 men (2.1%) and 242 women (2.3%) developed CVA/SE. The CVA/SE event rates were comparable between men and women (OR 1.146, 95% CI 0.97 to 1.354, p = 0.109; Figure 3 ). Heterogeneity was low with I 2 = 0. No significant publication bias was found, with 2-tailed p = 0.38, using Egger’s regression intercept method.
Gender-specific annualized major bleeding event rates in patients with AF treated with warfarin prophylaxis were reported in 4 studies, and these were included in the analysis. The pooled sample consisted of 25,997 patients with 16,637 men and 9,360 women. A total of 911 men (5.48%) and 486 women (5.2%) developed major bleeding. The forest plot demonstrating the differences in major bleeding event rates between the 2 genders is shown in Figure 4 . The major bleeding event rates were comparable between men and women (OR 0.926, 95% CI 0.81 to 1.059, p = 0.26). Heterogeneity was low with I 2 = 25. No significant publication bias was found, with 2-tailed p = 0.83, using Egger regression intercept method.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


