Fig. 3.1
The two layers of the pleura
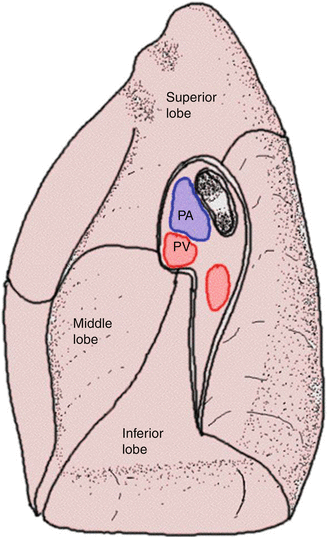
Fig. 3.2
The transition between the two layers at the level of the pulmonary hilum
Dissection of this ligament is usually one of the first surgical steps in thoracic surgical procedures and allows for a complete release and mobilization of the lung for further intervention. This pulmonary ligament contains several lymph nodes important in lung cancer staging. Indeed this area is an important part of the radical lymphadenectomy associated with pulmonary resection and is currently designated as station 9 in the international lymph node classification (Mountain 1997) (Fig. 3.3).
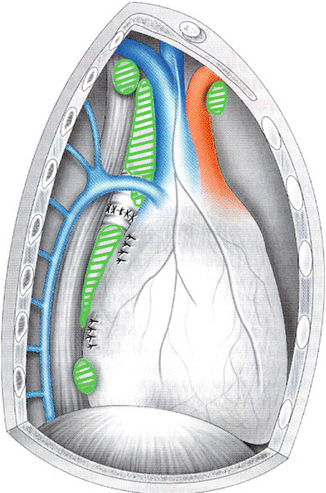

Fig. 3.3
Lymph node stations as approached by thoracoscopic
The space delineated by the two serosal layers of the pleura is commonly called the pleural space or pleural cavity. Both pleural surfaces have two layers: a superficial mesothelial cell layer facing the pleural space and an underlying connective tissue layer (Lee and Olak 1994).
The pleural space is a thin negative pressure cavity with a small amount of fluid. The amount of fluid is strictly regulated by processes of filtration and absorption. Indeed the lung has to change volume continuously during respiration. One of the primary roles of the pleural fluid is to transmit the transpleural forces occurring during the respiratory cycle and to ensure adequate coupling between the lung and the chest wall during normal breathing. The pleural cavity plays a major role in decreasing friction during respiration (Wang 1998).
3.2 Embryology
The pleural cavity is created between the fourth and the seventh week of embryologic development and at that stage is lined by the splanchnopleure and the somatopleure. These embryonic components of the visceral and parietal pleura develop different anatomic characteristics with respect to vascular, lymphatic, and nervous supply (Lee and Olak 1994; Wang 1998).
During the third week of gestation, there is differentiation of the embryonic mesoderm into three different parts; these are called the paraxial mesoderm, the intermediate mesoderm, and the lateral plates. The lateral plate is formed by two different layers: the first one is the somatic mesoderm or somatopleure and the second one is represented by the splanchnic mesoderm which is also referred to as the splanchnopleure. The somatopleure is the original membrane for the parietal pleura while the splanchnopleure will become the visceral layer of the pleura (Fig. 3.4).
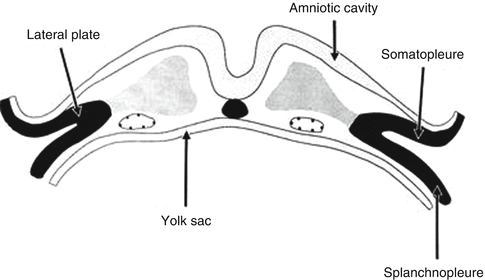

Fig. 3.4
The somatic mesoderm and the splanchnic mesoderm form the lateral plate
There is creation of the intraembryonic cavity by ventral migration of the somatopleure towards the midline. The intraembryonic coelom is the primitive cavity that will form the three major body cavities: pericardium, pleura, and peritoneum (Fig. 3.5). The pleural cavity is later separated by the diaphragm from the peritoneal cavity inferiorly. Superiorly the pleuropericardial fold divides into the heart and the lung buds at the end of the fifth week of gestation. There is midline fusion of the pleuropericardial folds and separation of the pleural cavity from the pericardial sac. The pleural cavity continues to expand until the end of the third month (Fig. 3.6).
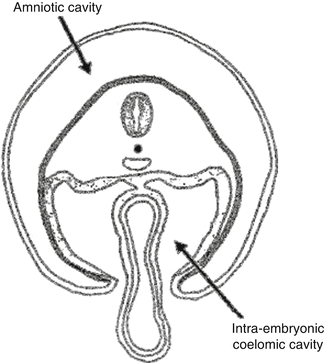
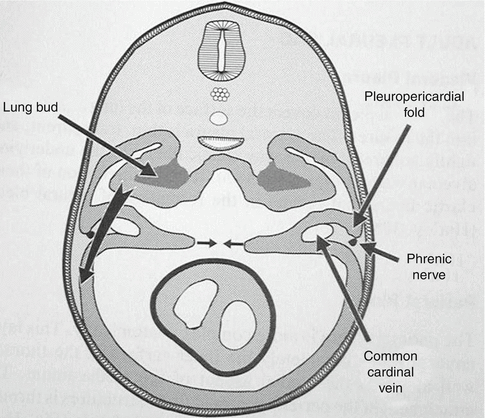

Fig. 3.5
The creation of the intraembryonic coelom

Fig. 3.6
The midline fusion of the pleuropericardial folds
3.3 The Visceral Pleura
The visceral pleura is a thin, transparent membrane which covers all the lung parenchymal surface and extends into the fissures. The visceral pleura is extremely adherent to the underlying lung parenchyma by elastic fibers. There is no plane between the alveolar tissue and the visceral pleura. Indeed the dissection of the visceral pleura, pleurectomy, results in lung damage by tearing the alveolar wall and inducing air leak from the alveoli. The disruption of the elastic fibers results in the formation of pleural blebs.
3.4 The Parietal Pleura
The parietal pleura is more complex anatomically. The parietal pleura almost completely covers the inner surface of the chest wall and the medial aspect of the mediastinum. The attachment of the parietal pleura to these structures is through a fibrous layer known as the endothoracic fascia. The parietal pleura is divided into three parts: the costal pleura, the diaphragmatic pleura, and the mediastinal pleura. The transition between each part produces several pleural sinuses. The first one is the anterior and posterior costomediastinal sinus, the second one is the costophrenic sinus, and the last one is the mediastinophrenic sinuses. The projection of the pleural sinuses is near identical on both sides. Anteriorly, laterally, and posteriorly the lung extends less inferiorly than the pleural sinuses. At the apex of the chest, the pleural space and the lung extend above the bony limits of the thorax (3 cm above the medial part of the clavicle). This data explains why injury in the neck can create pleural intrusion and in turn result in a traumatic pneumothorax.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


