Introduction to Breath Sounds
BREATH SOUND PRODUCTION
Three types of sounds are heard during auscultation—normal breath sounds, abnormal breath sounds (including voice sounds), and adventitious sounds. Breath sounds are produced by airflow patterns, by associated pressure changes within the airways, and by solid tissue vibrations within the lungs. Both normal and abnormal breath sounds have certain recognizable characteristics. Their intensity, duration, frequency, and quality are believed to be affected by airflow patterns, regional lung volume or distribution of air, body position, and the sound production site.
The sounds are normally diminished and filtered when they are transmitted through air-filled alveoli, fluid accumulations in the pleura, and solid structures, such as bone.
Breath sound origination
The sites where normal breath sounds originate aren’t clearly defined. For example, sounds heard over the trachea and large airways are characterized as high-pitched, harsh, loud, and tubular (hollow) with a long expiratory phase. These sounds are thought to reflect the turbulent airflow patterns in the first divisions of the large airways.
Sounds heard over other chest wall areas are softer and have a shorter expiratory phase. These sounds may also be produced by turbulent airflow in the first few divisions of the large airways; however, the fact that these sounds vary with changing airflow rates and distribution of ventilation in the lungs suggests that they are produced in the peripheral airways. Also, inspiratory sounds may be produced in the peripheral airways, and expiratory sounds may be produced in the larger airways. Breath sounds aren’t produced in the terminal bronchioles because of minimal airflow rates.
Disease
Disease processes that alter the airway or airflow dynamics produce abnormal breath sounds or adventitious sounds. These sounds are generated by the vibration of solid structures, by airflow through narrowed airways, or by abrupt changes in airway pressure.
Airway dynamics
The stability of an airway depends on the interaction of the elastic properties of the lung tissue, the intrapulmonary airways, and the pressures—both internal and external—exerted on the airways. During the respiratory cycle, a pressure gradient exists across the airway wall and between the trachea and alveoli. As the chest expands during inspiration, intrapleural pressure falls. At the same time, the lung’s elastic recoil increases, exerting traction on airway walls. This traction increases the airway’s diameter and decreases the resistance to airflow. The pressure gradient between the alveolar and atmospheric pressures increases, driving air through the airways toward the alveoli.
In older persons, pulmonary function decreases because of respiratory muscle degeneration or atrophy. Ventilatory capacity diminishes because the lungs’ diffusing capacity declines, decreased inspiratory and expiratory muscle strength diminishes vital capacity, and lung tissue degeneration causes a decrease in the lungs’ elastic recoil capacity, which results in an elevated residual volume. For these reasons, aging can cause changes consistent with emphysema.
Intrapleural pressure and alveolar elastic recoil pressures drive expiratory airflow. At the beginning of expiration, intrapleural pressure and the alveolar recoil force cause the alveolar pressures to rise and push the air through the airways and out through the upper airway. Air pressures fall as the air flows through the airways from the alveoli to the upper airway. A point is reached, particularly during forceful expiration, when intrapleural and intrapulmonary pressures are equal. Called the equal pressure point, it can occur anywhere within the thorax and is a function of the mechanical properties of the lung (elastic recoil, airflow resistance, and stiffness of the walls of the airway). Downstream from this point, pressures outside of the airways can compress and further narrow the airways, causing increased resistance to airflow.
Airflow patterns
Variations in airflow patterns are affected by the intricate network of branching airways, the various airway diameters, and the potential for irregular airway wall surfaces within the tracheobronchial tree.
Turbulent airflow
During rapid, or turbulent, airflow, air molecules move randomly, colliding against airway walls and each other. They may move across or against the general direction of airflow. The colliding air molecules produce rapid pressure changes within the airway, and these rapid pressure changes produce sounds. Turbulent airflow occurs in the trachea, mainstem bronchi, and other larger airways.
Transitional airflow
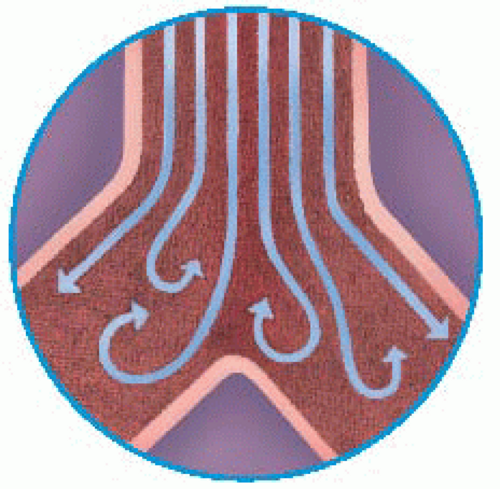
As airflow is forced to change directions abruptly in the branching airways, the airstream separates into layers and moves at different velocities.
Laminar airflow
In the terminal or small airways and respiratory bronchioles, airflow is slow and laminar, or nonturbulent. No abrupt changes in pressure or airway wall movements occur to generate sound. Consequently, air movement in these areas produces no sound.
Mechanical vibrations
Breath sounds are also produced by mechanical vibrations of solid tissue. These vibrations travel through the different media of air, fluid, or tissue at varying speeds. Their frequency, intensity, and duration can be measured.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree