Chapter 21 Chest Pain
Chest pain is a very common symptom, and its severity and etiology will depend, to a large extent, on the clinical circumstances in which it occurs. Chest pain is the most frequent new symptom reported by patients seen in outpatient clinics. Although it is an extremely nonspecific symptom (Box 21-1), it may be the presenting manifestation of a number of conditions, most of which will be relatively benign. Also, in many patients with such pain, a firm diagnosis may never be established. When chest pain is a presenting symptom in the emergency department setting, however, more serious, acute, and potentially life-threatening causes need to be considered. Accordingly, a complaint of chest pain requires thorough and careful investigation.
Box 21-1
Causes of Chest Pain
Cardiac System
Musculoskeletal Conditions
Differential Diagnosis
Myocardial Ischemia
A wide range of disorders other than angina may be the cause of chest pain. These potential alternative diagnoses are summarized in Box 21-2.
Musculoskeletal Pain
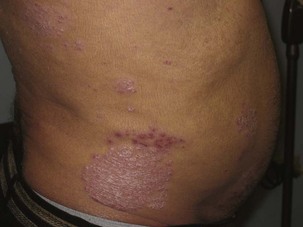
Costochondral and chondrosternal articulations are common sites of anterior and anterolateral chest pain. The articulations of the second, third, and fourth ribs are most commonly involved. When accompanied by swelling, redness, and heat, the condition is referred to as Tietze syndrome. Coughing or trauma can dislocate the costochondral junctions (most commonly those of ribs 10 to 12). The pain resulting from intercostal neuritis most frequently results from cervical osteoarthritis. Intercostal neuritis also is seen with herpes zoster infection, in which the onset of pain may precede the typical rash by 1 or 2 days (Figure 21-1). Thoracic roots most commonly are involved.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree