A. BT shunt
B. Classic Glenn anastomosis
C. Bidirectional cavopulmonary anastomosis
D. Extracardiac modified Fontan anastomosis
E. Unifocalization procedure
8. Which of the following operations carries the highest risk of post-operative sinus node dysfunction?
A. Atrial switch (Mustard) procedure
B. Repair of truncus arteriosus
C. Repair of tetralogy of Fallot
D. Repair of a large muscular VSD
E. Mitral valve mechanical prosthesis replacement
9. You are meeting with the family of a 1-month-old child with hypoplastic left heart syndrome prior to stage I of the hybrid Norwood procedure. Which of the following best describes the role of the interventional pediatric cardiologist in this procedure?
A. Balloon dilation of the pulmonary arteries
B. Stenting of the coarctation of the aorta
C. Endoluminal pulmonary artery banding
D. Stenting of the ductus arteriosus
E. Aortic balloon valvuloplasty
10. A 3-month-old patient is undergoing repair for tetralogy of Fallot and severe pulmonary stenosis. After initiation of cardiopulmonary bypass, using bicaval and aortic cannulation, the surgeon notes progressive left heart distention. This is most likely due to the presence of which of the following?
A. Persistent left superior vena cava
B. VSD
C. Patent foramen ovale
D. Aortic valve regurgitation
E. Aortopulmonary collaterals
11. A 17-year-old boy who had complete repair of a partial AVSD at 15 months of age presents with progressive shortness of breath. He has a 2/6 systolic crescendo–decrescendo murmur that is less prominent with Valsalva. Chest x-ray reveals mild cardiomegaly and mildly increased pulmonary vascularity. Which of the following is the most likely cause of his symptoms?
A. Mitral regurgitation
B. Primary pulmonary hypertension
C. LVOT obstruction
D. Mitral stenosis
E. Residual ASD
12. A 2-month-old girl is found to have a moderate-large perimembranous VSD with left-to-right shunt. She has mild left ventricular and left atrial enlargement and an estimated right ventricular systolic pressure of 38 mm Hg by Doppler echocardiography. She is growing appropriately and has no respiratory distress with feedings. In the absence of heart failure, by what age should she have surgical repair of her VSD?
A. 3 months
B. 12 months
C. 18 months
D. 2 years
E. 3 years
13. A 2-week-old infant is found to have anomalous left coronary artery from the pulmonary artery (ALCAPA). Which of the following pre-operative findings is most closely associated with post-operative mortality and need for late re-operation?
A. Mitral insufficiency
B. Tricuspid insufficiency
C. Aortic valve insufficiency
D. Pulmonary valve insufficiency
E. Pulmonary valve stenosis
14. What is the most common long-term complication in repaired Scimitar syndrome?
A. Atrial arrhythmia
B. Right ventricular systolic dysfunction
C. Pulmonary vein obstruction
D. IVC–RA junction stenosis
E. Pulmonary hypertension
15. A 3-year-old child has complex single ventricle, bilateral superior venae cavae, and interrupted IVC with azygous continuation to the right SVC. Initial palliation consisted of placement of bilateral bidirectional cavopulmonary anastomoses. Post-operatively his oxygen saturation is 87%. Now his saturation is 75%. Which of the following is most likely to have contributed to his progressive desaturation?
A. Erythrocytosis
B. Intrapulmonary shunting
C. Decreased chest wall compliance
D. Increased coronary sinus drainage
E. Increased pulmonary vascular resistance
16. You are asked to evaluate a 4-year-old child who recently moved to the USA from Russia. He has tricuspid atresia, normally related great arteries and pulmonary stenosis. At 3 weeks of age, he had a modified BT shunt. His height and weight are in the 15th percentile. The left ventricular impulse is slightly overactive. S1 is normal, S2 is single, and there is a 2/6 continuous murmur at the base of the heart. The liver is 1 cm below the right costal margin. The hemoglobin is 17 g/dL. The data in Table 11.1 are obtained at the time of cardiac catheterization.
Table 11.1 Cardiac Catheterization Data
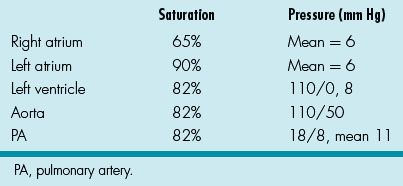
An angiogram reveals normal size and distributed pulmonary arteries. An echocardiogram reveals an LV ejection fraction of 60%. Which of the following would you recommend?
A. Perform a bidirectional Glenn and takedown of the BT shunt
B. Delay any operative intervention until the hemoglobin reaches 19 g/dL
C. Perform an atriopulmonary connection and closure of the ASD and takedown of the BT shunt
D. Perform an extracardiac fenestrated Fontan and takedown of the BT shunt
E. Perform an extracardiac nonfenestrated Fontan and takedown of the BT shunt
17. You are asked to evaluate a 4-year-old child who recently moved from Russia. He has tricuspid atresia, normally related great arteries and pulmonary stenosis. At 9 months of age, he had a classic Glenn anastomosis. An echocardiogram reveals normal left ventricular systolic function. The data in Table 11.2 are obtained at the time of cardiac catheterization.
Table 11.2 Cardiac Catheterization Data
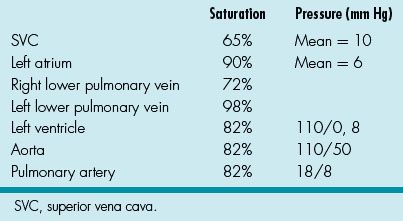
Which of the following is true?
A. The patient is not a candidate for a modified Fontan operation.
B. The right lower pulmonary vein should be allowed to drain to the systemic venous side after modified Fontan operation.
C. Completion of a lateral tunnel nonfenestrated Fontan will result in complete separation of arterial (oxygenated) and venous (deoxygenated) circulations.
D. Perfusion of the right lung with hepatic effluent blood should improve systemic arterial oxygen saturation.
E. The Glenn anastomosis should be left intact and a modified BT shunt should be placed from the left subclavian artery to the right pulmonary artery
18. A 1-day-old infant is diagnosed with tricuspid atresia, normally related great arteries and a large ASD. Oxygen saturation is 60% to 65% on room air. On examination, the child is cyanotic but well-perfused. Chest x-ray shows diminished pulmonary vascularity. Which of the following will this patient most likely require as the first palliative intervention?
A. Balloon atrial septostomy
B. Modified BT shunt placement
C. Pulmonary artery banding
D. Damus–Kaye–Stansel (DKS) anastomosis
E. DKS anastomosis with pulmonary artery banding
19. A neonate is diagnosed with tricuspid atresia and d-transposition of the great arteries (d-TGA). On examination, you note poor perfusion and a loud, harsh ejection-type murmur. Oxygen saturation is 85% on room air. Which of the following is the best initial palliation for this patient?
A. Surgical enlargement of VSD
B. Modified BT shunt
C. Pulmonary artery banding
D. DKS anastomosis with modified BT shunt
E. DKS anastomosis with pulmonary artery banding
20. A 2-year-old male undergoes successful surgical valvotomy for a stenotic dysplastic pulmonary valve resistant to balloon dilation. Post-operative echocardiography documents mild valvular regurgitation with a predicted gradient across the valve of 10 mm Hg. What is the likelihood that this child will need re-intervention on his pulmonary valve within the next 10 years?
A. 95%
B. 80%
C. 50%
D. 20%
E. 5%
21. A 4-year-old child has pulmonary atresia and intact ventricular septum. She had placement of a BT shunt as a neonate. Her pulmonary artery trunk diameter is 10 mm. Pulmonary arteriolar resistance is 2.5 WU*m2. Her hemoglobin is now 20 g/dL. Tricuspid valve Z-score is −4. Which of the following is the best next step in this patient’s management?
A. Partial exchange transfusion with a goal hemoglobin of 15 g/dL
B. Routine follow-up until symptoms develop
C. Bidirectional cavopulmonary anastomosis with takedown of the BT shunt
D. ASD closure, tricuspid valve repair or replacement, and RV outflow tract reconstruction
E. Modified (extracardiac) Fontan and BT shunt takedown
22. A 3-month-old infant has pulmonary atresia with intact ventricular septum and status a post-modified right BT shunt placement. His oxygen saturation is 70% on room air. An angiogram documents confluent pulmonary arteries with valvular atresia. The right ventricle is tripartite but diminutive. The tricuspid valve is well developed with moderate regurgitation and an annulus Z-score of −2.0. There is no evidence of right ventricle–dependent coronary circulation. Which of the following is the best next treatment choice for this patient?
A. Left-sided modified BT shunt placement
B. Central shunt placement
C. RV outflow reconstruction with BT shunt takedown
D. Unifocalization procedure with RV outflow reconstruction
E. Bidirectional cavopulmonary anastomosis with BT shunt takedown
23. The angiogram in Figure 11.2. is performed in a 4-month-old boy with pulmonary atresia with intact ventricular septum and a large patent ductus arteriosus. Pulmonary arteriolar resistance is 3 WU*m2.
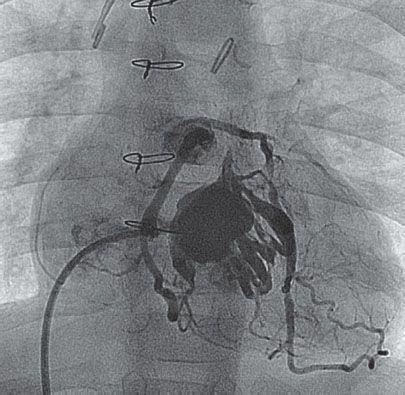
Which of the following operations is best for this patient at this time?
A. Pulmonary valvotomy, modified BT shunt placement
B. PDA ligation, bidirectional Glenn anastomosis
C. PDA ligation, RV to PA conduit placement
D. PDA ligation, pulmonary valvotomy with a bidirectional Glenn
E. PDA ligation, bidirectional Glenn anastomosis, RV to PA conduit placement
24. A 3-year-old child has pulmonary atresia with VSD. He has a history of hypoplastic central pulmonary arteries and multiple major aortopulmonary collateral arteries (MAPCAs), with multiple surgeries including a central shunt and bilateral unifocalization procedures. He undergoes reconstruction of the central confluence, placement of RV–PA conduit, ligation of two MAPCAs, and VSD closure. When cardiopulmonary bypass is discontinued, his blood pressure is 84/60 mm Hg on multiple inotropic agents. Arterial blood oxygen saturation is 87% on 100% inhaled oxygen. Right ventricular systolic pressure is 69 mm Hg by direct measurement. TEE demonstrates patency of the conduit. Which of the following is the best next step?
A. Placement of ECMO until hemodynamics improve
B. Re-opening the VSD
C. Takedown of RV–PA conduit and re-placement of a central shunt
D. Replacement of the RV–PA conduit with a larger conduit
E. Treatment with nitric oxide to improve pulmonary vascular resistance
F. Removal of the MAPCA ligatures
25. A neonate with prenatally diagnosed truncus arteriosus is born at 38 weeks gestation via uncomplicated vaginal delivery. On his post-natal echocardiogram, the pulmonary arteries arise from a common trunk and are unobstructed with increased, laminar flow. The aortic arch is right-sided. The truncal valve is quadricuspid with moderate regurgitation. There are no other complicating factors. Which of the following is the best initial surgical intervention for this infant?
A. BT shunt placement within the first week of life
B. Truncal valve repair by 1 month of age
C. Complete repair by 1 month of age
D. Bidirectional cavopulmonary anastomosis at 4 months of age
E. Pulmonary artery banding by 6 months of age
26. Which of the following is the most common indication for re-operation in a patient with a history of truncus arteriosus repair?
A. Neo-aortic valve regurgitation
B. Neo-aortic valve stenosis
C. RV–PA conduit failure
D. Residual VSD
E. Branch pulmonary artery stenosis
27. An asymptomatic 1-year-old child is referred for a murmur. Her blood pressure is 104/56 mm Hg (left arm) and 84/50 mm Hg (left leg). The echocardiogram confirms discrete coarctation of the aorta. Assuming the patient remains asymptomatic without progression of upper extremity hypertension, when would you recommend surgical repair?
A. Age 2 to 3 years
B. Age 5 to 7 years
C. Age 12 to 14 years
D. Only operate when systolic pressure gradient > 40 mm Hg
E. Only operate when she develops moderate or worse left ventricular hypertrophy
28. You are discussing the mortality risks to parents of a newborn with hypoplastic left heart syndrome. They ask about the risk of dying during the various stages of the surgical Norwood procedure. You explain that current data suggest that the highest risk of mortality is during which of the following periods?
A. Prior to stage 1 palliation
B. Between stage 1 and stage 2 palliation
C. During stage 2 palliation
D. Between stage 2 and stage 3 palliation
E. During stage 3 palliation
29. One day after a hybrid Norwood palliation procedure, a 7-day-old term neonate develops progressive cyanosis and metabolic acidosis. He is tachypneic with an oxygen saturation of 65% on room air. His heart rate is 160/minute, blood pressure is 65/42 mm Hg. His chest x-ray demonstrates increased pulmonary vascular markings. Which of the following best explains his worsening clinical status?
A. Pulmonary hypertension
B. PDA closure/occlusion
C. PA branch obstruction
D. Restrictive ASD
E. Hypovolemia
30. Which of the following is a goal of stage 1 surgical palliation (Norwood) for hypoplastic left heart syndrome?
A. Restriction of coronary artery blood flow
B. Creation of a nonrestrictive VSD
C. Establishment of an unrestricted source of pulmonary blood flow
D. Relief of ductal-dependent systemic blood flow
E. Unrestricted right-to-left atrial level shunt
31. Which of the following is the most common short-term complication of arterial level repair of d-TGA?
A. Supravalvular pulmonary stenosis
B. Supravalvular aortic stenosis
C. Neo-aortic root dilation
D. Neo-aortic valve regurgitation
E. Coronary artery occlusion
32. While being weaned off cardiopulmonary bypass following an arterial switch procedure for d-TGA, a neonate has persistent hypotension and poor left ventricular function with regional wall motion abnormalities. Which of the following best explains this patient’s clinical status?
A. Presence of ASD/PFO
B. Cerebral air embolism
C. Severe pulmonary regurgitation
D. Kinking or occlusion of coronary arteries
E. Global dysfunction due to cardiopulmonary bypass
33. A neonate is found to have d-TGA with VSD and ASD. The VSD is nonrestrictive, but there is severe left ventricular outflow obstruction. The patient’s oxygen saturation is 68% on room air. What is the most appropriate initial intervention for this patient?
A. Jatene arterial switch with Lecompte maneuver
B. Mustard operation
C. LV outflow tract balloon dilation
D. PDA stent
E. BT shunt
34. A 2-year-old child with L-TGA, large membranous VSD with outlet extension, and history of critical pulmonary stenosis has been palliated with a modified BT shunt in the neonatal period and a bidirectional cavopulmonary anastomosis at 6 months of age. His oxygen saturation is 70%. He has good biventricular size and function, and no AV valve straddling. He is presenting for surgical intervention. Which of the following is a reasonable alternative to a modified Fontan operation for this patient?
A. Closing the VSD to the pulmonary valve
B. Closing the VSD to the aortic valve (Rastelli-type repair) and placement of a pulmonary conduit
C. Closing the VSD to the pulmonary valve and baffling IVC to the tricuspid valve
D. Closing the VSD to the aortic valve, placement of a pulmonary conduit, and baffling of IVC to the tricuspid valve
E. Closing the VSD to the aortic valve, placement of a pulmonary conduit, and baffling of IVC to the mitral valve
35. You are performing an echocardiogram on a ductal-dependent newborn infant in the neonatal ICU. You diagnose double-outlet right ventricle with normally related great arteries and large doubly committed VSD, severe coarctation of the aorta, mild subaortic stenosis, and parachute mitral valve which straddles the VSD. What is the most appropriate initial surgery for this patient?
A. Patch VSD to aorta, repair coarctation
B. Repair coarctation, mitral valve annuloplasty, and chord lengthening
C. Repair coarctation only
D. Norwood palliation with Sano shunt
E. Patch VSD to aorta, repair coarctation, resection of subaortic stenosis
36. What is the surgical procedure of choice for patients with Taussig–Bing anomaly?
A. Pulmonary artery banding with enlargement of the VSD
B. Arterial switch with baffle closure of the VSD to the neo-aorta
C. Systemic to pulmonary (BT) shunt
D. Patch closure of the VSD
E. Aortopulmonary anastomosis and pulmonary artery banding
37. A term neonate with a harsh systolic murmur at birth is found to have double-inlet left ventricle with a hypoplastic subaortic right ventricle, a restrictive bulboventricular foramen, and severe subaortic stenosis. Prostaglandin-E1 infusion is started. A subsequent echocardiogram documents a large ductus arteriosus. Which of the following is the most appropriate initial operation for this child?
A. Enlargement of the VSD
B. Pulmonary artery banding
C. Bidirectional cavopulmonary anastomosis
D. PDA stent placement and banding of the PAs (hybrid Norwood)
E. Aortopulmonary anastomosis (DKS) with BT shunt
38. A 5-year-old female is found to have a murmur during a routine physical examination. Echocardiogram reveals a secundum ASD with continuous right-to-left shunt. Which of the following factors would be the strongest indication for surgical repair rather than percutaneous closure of the ASD?
A. Patient’s age
B. Deficient anterior septal rim
C. History of dyspnea on exertion
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


