Chapter 61 Obstructive Sleep Apnea
Clinical Features, Diagnosis, and Treatment*
Clinical Features
The clinical presentations of obstructive sleep apnea (OSA) are legion. Common clinical features can be divided into major and minor categories, as summarized in Box 61-1. Patients may present with daytime and/or nocturnal complaints, but commonly, spouses and living companions are the first to push for medical attention.
Excessive Daytime Sleepiness
Sleepiness is difficult to define and is a subjective feeling of impairment of concentration and increased craving for sleep. Excessive daytime sleepiness (EDS) is a nonphysiologic complaint that is not satisfied by a restorative sleep. Sleepiness is reported by 30% to 50% of the general population, so EDS alone is a poor predictor of OSA and requires a differential diagnosis to exclude many other medical conditions associated with this daytime symptom, such as depression, fibromyalgia, chronic insomnia, or hypothyroidism. Patients with OSA sometimes refer to EDS as abnormal daytime tiredness or lack of energy and convey the impression that they must make stringent efforts to remain alert and awake. It is believed that the loss of the restorative function of sleep due to repetitive arousals is the main mechanism to explain the presence of EDS in OSA. The Epworth Sleepiness Scale (Box 61-2) is the most popular tool for subjective evaluation (self-assessment) of EDS. A score above 10 of 24 is considered to be clinically relevant. The relationship between the Epworth score and the apnea-hypopnea index (AHI) (as a surrogate index of OSA severity) is relatively poor. In fact, 35% patients with severe OSA identified within sleep clinics do not complain of EDS. This discrepancy is partly due to underestimation or intentional underreporting the severity of sleepiness for personal gain, such as to avoid job loss. On the other hand, patients scoring high in the Epworth scale could have just mild to moderate OSA. EDS is the most disabling symptom among patients with OSA. One example is drowsiness while driving, which is associated with a three-fold increase in risk of accidents in patients with OSA. Poor school or job performance also is frequently reported.
Box 61-2 Epworth Sleepiness Scale
Patient Questionnaire
Sitting and reading __________
Sitting, inactive in a public place (e.g., a theater or a meeting) __________As a passenger in a car for an hour without a break __________
Lying down to rest in the afternoon when circumstances permit __________
Sitting and talking to someone __________
Sitting quietly after lunch without alcohol __________
In a car, while stopped for a few minutes in traffic __________
From Johns MW: A new method for measuring daytime sleepiness: the Epworth Sleepiness Scale, Sleep 14:540–545, 1991.
Physical Examination 
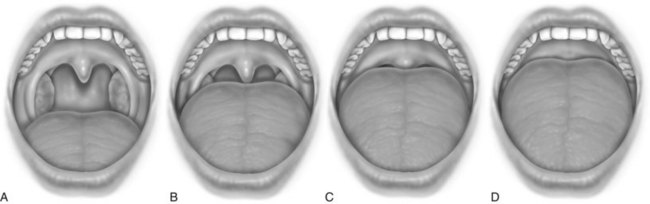
After a complete history has been obtained, a systematic examination should be performed. In nonobese patients (body mass index [BMI] less than 30 kg/m2), common physical findings can be observed in the craniofacial, nasal, pharyngeal, and dental areas (Box 61-3). Radiographic cephalometry is indicated if craniofacial abnormalities are suspected or if upper airway surgery is planned to treat the patient. The oropharynx must be examined, and the degree of oropharyngeal crowding can be scored using the Friedman Tongue Position, formerly called the modified Mallampati score. For this assessment, the patient is asked to open the mouth widely without protruding the tongue. The observer can assign scores as indicated in Figure 61-1. Higher scores suggest the presence of OSA.