Chapter 24 Community-Acquired Pneumonia
Risk Factors
Certain risk factors are associated with higher frequency of infections with particular pathogens.
Patient Evaluation/Diagnostics
Clinical presentation of CAP can be rather nonspecific, especially in elderly and debilitated persons. Risk factors for specific causative agents, such as history of recent travel into endemic areas, is an important part of the clinical history in a patient with suspected CAP. Because of the inaccuracy of a purely clinical diagnosis, additional investigations are required to confirm the diagnosis, identify the causative pathogen, and initiate appropriate treatment. These are discussed in Chapter 23. Table 24-1 summarizes the American Thoracic Society/Infectious Diseases Society of America (ATS/IDSA) recommendations of tests proven to be useful in different settings for investigating and treating CAP.
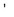 10 billion in Europe. According to British Thoracic Society guidelines, age-standardized rate of hospital admissions due to CAP rose by 34% from 1997 to 2004. CAP also is the most common cause of severe sepsis. Admission to the intensive care unit (ICU) is required in up to 20% of cases of CAP. Because the incidence of pneumonia is substantially higher among elderly persons, it is anticipated that in view of the aging population, the incidence and health care burden of pneumonia will only increase. In the United States, approximately 4.2 million outpatient clinic visits for pneumonia were recorded for 2006, and this number has been increasing ever since. At the same time, despite introduction of novel antimicrobials, imaging modalities, and biomarker testing, mortality attributable to CAP has not changed significantly since the introduction of penicillin.
10 billion in Europe. According to British Thoracic Society guidelines, age-standardized rate of hospital admissions due to CAP rose by 34% from 1997 to 2004. CAP also is the most common cause of severe sepsis. Admission to the intensive care unit (ICU) is required in up to 20% of cases of CAP. Because the incidence of pneumonia is substantially higher among elderly persons, it is anticipated that in view of the aging population, the incidence and health care burden of pneumonia will only increase. In the United States, approximately 4.2 million outpatient clinic visits for pneumonia were recorded for 2006, and this number has been increasing ever since. At the same time, despite introduction of novel antimicrobials, imaging modalities, and biomarker testing, mortality attributable to CAP has not changed significantly since the introduction of penicillin.