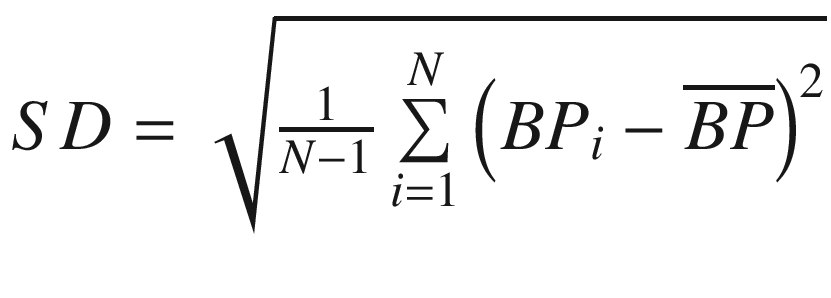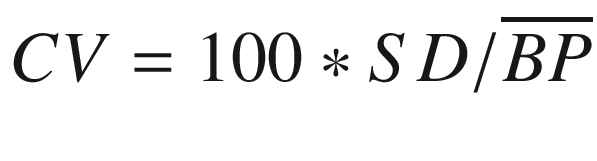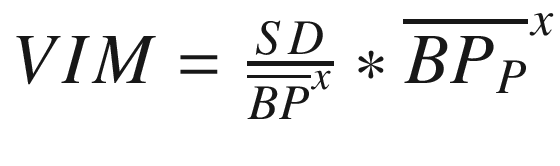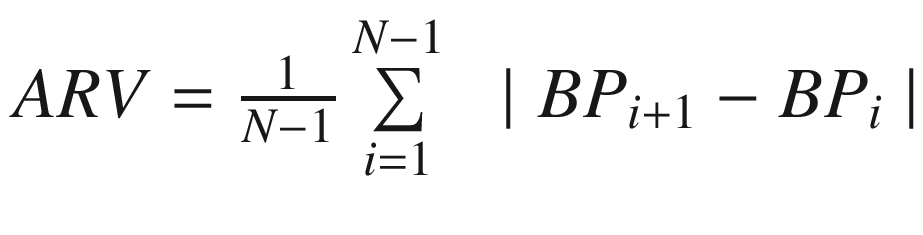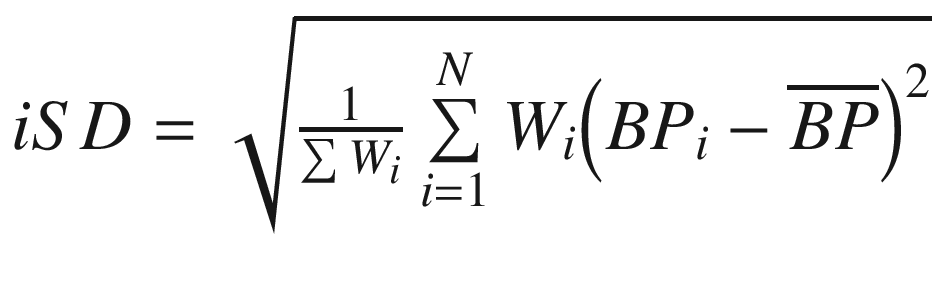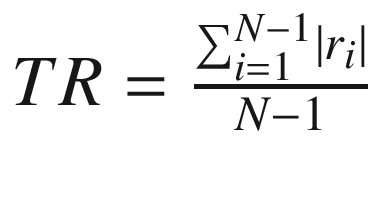Different types of blood pressure variability, their determinants, and prognostic relevance. Taken from [2] by permission. ∗Assessed in laboratory conditions; ‡cardiac, vascular, and renal subclinical organ damage; §blood pressure variability on a beat-to-beat basis has not been routinely measured in population studies. Abbreviations: AHT antihypertensive treatment, BP blood pressure, BPV blood pressure variability, ESRD end-stage renal disease, eGFR estimated glomerular filtration rate
The aim of this chapter is to review the available evidence regarding day-by-day home blood pressure variability, its mechanisms, the methodological aspects for its assessment based on home BP measurements as well as its clinical relevance for cardiovascular prognosis. Specific aspects relevant in the light of potential clinical application of home blood pressure variability will also be addressed, such as whether and how it should be assessed in addition to average BP levels, and whether and how antihypertensive treatment strategies should be targeted at reducing not only average BP levels but also the degree of day-by-day blood pressure variability in order to optimize cardiovascular protection. In view of the considerable semantic confusion in the field, in this chapter we will use the term home blood pressure variability in relation to blood pressure variability assessed on a day-to-day basis with self BP monitoring at home. In most cases this is equivalent to day-to-day blood pressure variability or midterm blood pressure variability, although there might be some exceptions (e.g., day-to-day variability of office BP or long-term variability of home BP).
14.2 Factors Associated with Increased Home BPV
When considering midterm blood pressure variability, behavioral factors such as job strain, levels of physical activity, sleep/wakefulness cycles, quality and duration of sleep, postural changes, and patterns of sodium intake have been shown to play an important role in determining the degree of day-by-day BP fluctuations (see Fig. 14.1 and Box 14.1). This is exemplified by studies in which significant changes in BP levels between working days and the weekend have been reported [3]. Population studies have identified several factors associated with increased values of day-by-day blood pressure variability in home measurements such as advanced age, female gender, increased arterial stiffness, elevated mean BP values, low body mass index, low heart rate, high heart rate variability, excessive alcohol intake, cigarette smoking, history of peripheral artery disease, cardiovascular disease, diabetes mellitus, diabetic nephropathy, and sedentary lifestyle [4–9]. Of note, a population study in elderly subjects showed higher values of midterm blood pressure variability among subjects with masked and sustained hypertension compared to those with sustained normotension and white-coat hypertension [10]. This study has also suggested that increasing degrees of day-by-day BP fluctuations might prevent the identification of sustained hypertension.
Studies focusing on treated hypertensive patients have found a higher day-by-day blood pressure variability among these individuals compared to untreated subjects [5, 7], also reporting higher values of home blood pressure variability in case of treatment with beta-blockers, short duration of treatment [11], and increasing number of antihypertensive drugs [8].
Box 14.1: Mechanisms and Factors Responsible for Midterm Blood Pressure Variability
Job strain/home stress
Levels of physical activity
Changes of sleep/wakefulness cycles
Quality and duration of sleep
Postural changes
Level of sodium intake
Smoking/alcohol
Inconsistent BP control
Poor patient’s adherence to prescribed drugs
Improper dosing/titration of antihypertensive drugs
Dose omission or delay in drug intake
Incorrect home BP monitoring conditions
Seasonal changes in ambient temperature
Changes in barometric pressure and altitude above sea level
14.3 Methodological Aspects in the Assessment of Midterm Blood Pressure Variability
Adequate implementation of a proper BP monitoring method, according to current hypertension guidelines recommendations, is critical to guarantee an accurate estimation of BP values and hence of blood pressure variability indices, either for research purposes or in a clinical setting [12–16] (Box 14.2).
Box 14.2: Methods of Day-by-Day Blood Pressure Variability Assessment
Devices: Use of validated automated oscillometric upper-arm cuff devices
Method for BP measurement: HBPM
Measurement intervals:
Day-by-day
From morning to evening
Number of measurements: For HBPM duplicate BP measurements (1 min apart) in the morning and in the evening for each day
Time of measurement:
Morning and evening before food and/or drug intake (some guidelines recommend only morning readings)
Perform HBPM during usual working days
Time of measurement in treated patients: Morning and evening BP measurements before drug intake (patients should be under stable treatment)
Duration of the recording period and measurement sequence:
HBP measurement schedule over several (preferably 7 and at least 3) working days is suggested as the optimal approach before each office visit, with this sequence repeated after weeks or months when assessing the effects of treatment
Duplicate morning and evening measurements, taken at 1-min interval after a 5-min rest (for the comparative assessment of morning vs. evening vs. morning-evening combination)
Editing. No editing is recommended at present (apart from discarding first day measurements)
Main indices of blood pressure variability: SD, CV, ARV, VIM, morning-evening changes, maximum-minimum values
Advantages inexpensive, well accepted by patients.
Possible disadvantages
Patients’ training required for HBPM
Possibility of measurements in selected conditions only and misreporting of readings
Data for blood pressure variability calculation must be entered manually, unless devices with data storage and transfer capabilities are used
The common approach for the evaluation of day-by-day blood pressure variability consists in its assessment from self BP measurements performed by patients at home over several days according to the current ESH recommendations [13, 16, 17]. Although HBPM cannot currently provide information on nighttime BP (except with few novel home BP monitors) nor on 24 h BP profiles (as ABPM does), it is widely available, it has rather low-cost, and is well accepted by patients, while providing adequate BP measures for estimation of day-by-day blood pressure variability, devoid of the white coat effect. Overall, HBPM schedule should consist of duplicate morning and evening BP measurements with validated devices for a 7-day period (at least 3 days required) before each office visit [16]. A recent report of the International Database of Home Blood Pressure in Relation to Cardiovascular Outcome (IDHOCO) study, based on analysis of morning HBP measurements, has indicated that indices of home blood pressure variability may retain their prognostic value even when calculated from a 3-day schedule as compared to the suggested 7-day [18]. Regarding the question on whether morning or evening HBP measures should be considered, evidence from outcome studies is in part controversial, with some studies indicating the superior prognostic value of day-by-day home blood pressure variability determined on the basis of morning BP measures as compared to morning-evening or evening home blood pressure variability [19, 20], while other studies (e.g., the HOMED-BP study) showed evening HBPV before treatment to be a better predictor of outcome [21].
Although the large heterogeneity among studies in terms of measurement schedules (number of readings, number of days, morning and/or evening), BP devices and blood pressure variability indices has not yet allowed to identify the ideal approach for assessment of midterm blood pressure variability based on HBPM [22], some recommendations based on available evidence are presented in Box 14.2.
14.3.1 Indices for Assessment of Midterm Blood Pressure Variability
Indices for estimation of midterm blood pressure variability
Type of index | Index | Formula |
|---|---|---|
Dispersion | Standard deviation (SD) |
|
Coefficient of variation (CV) |
| |
Variability independent of the mean (VIM) |
| |
Sequence | Average real variability (ARV) |
|
Interval weighted SD (wSD) |
| |
Time rate of BP variation |
| |
Instability | Range (maximum–minimum BP) | Range = Max – Min |
Peak size (maximum BP) | Peak = Max − mean | |
Trough size (mean-minimum BP) | Trough = Mean − Min |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree