Questions
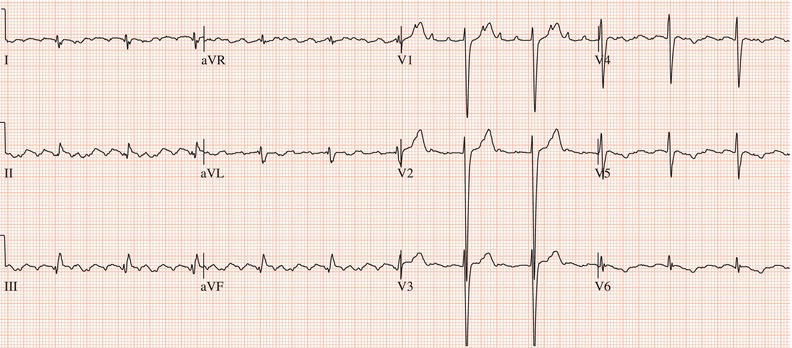
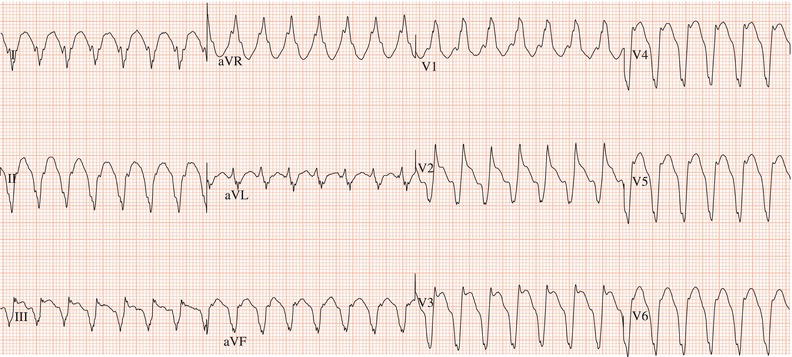
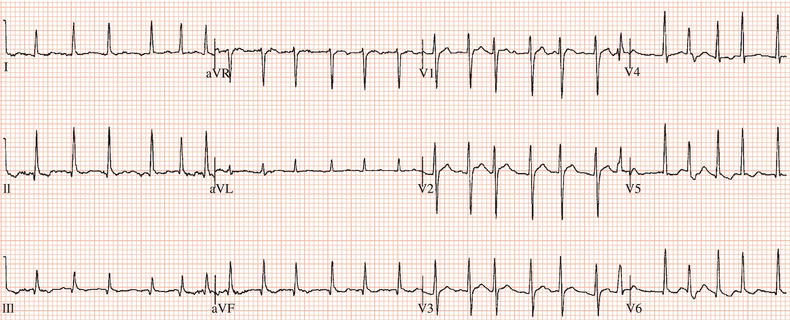
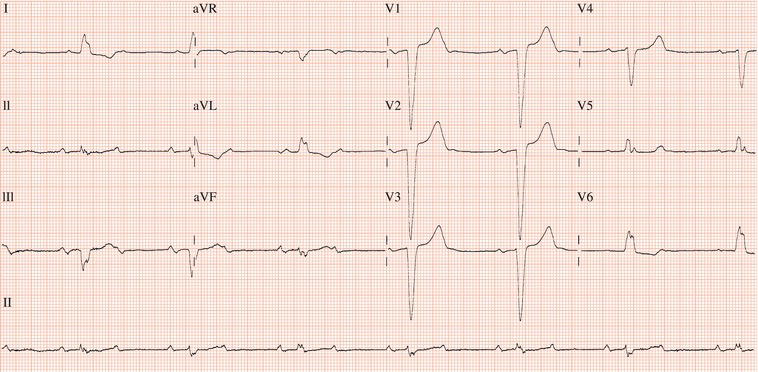
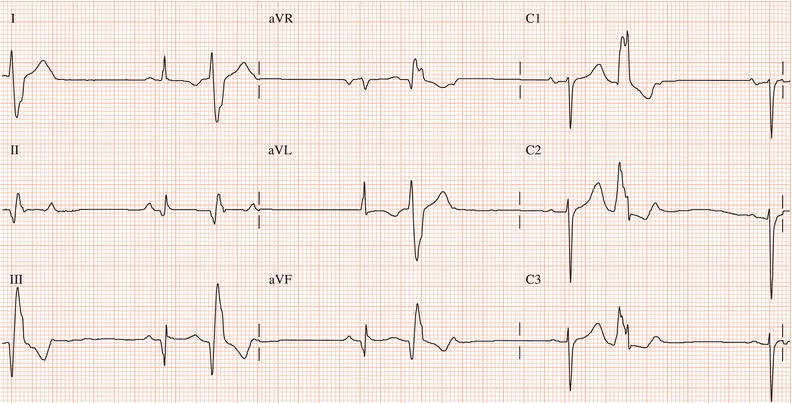
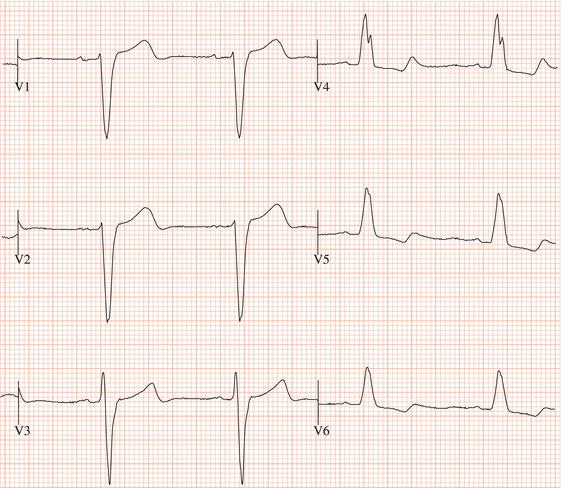
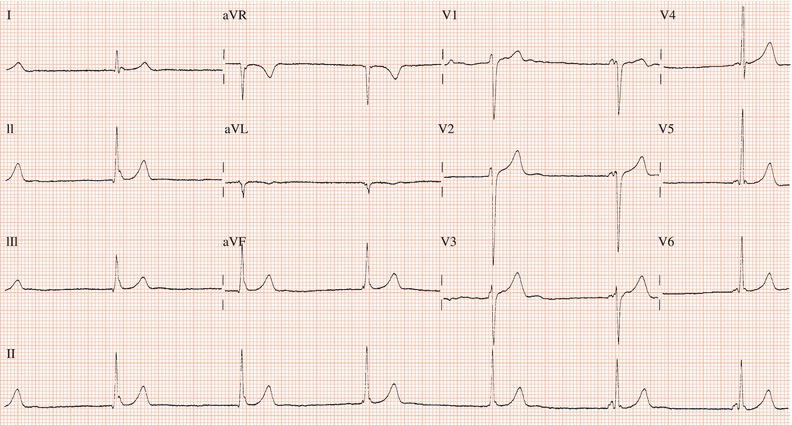
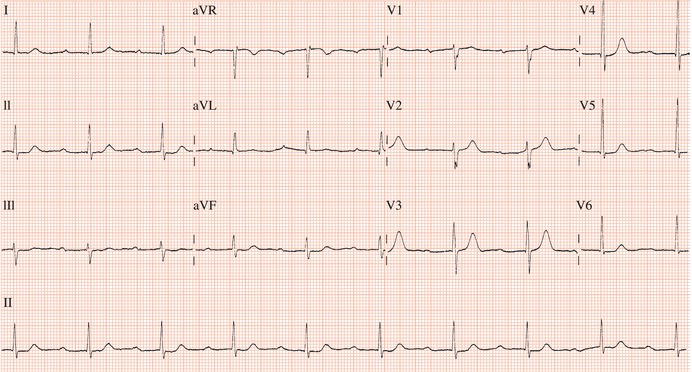
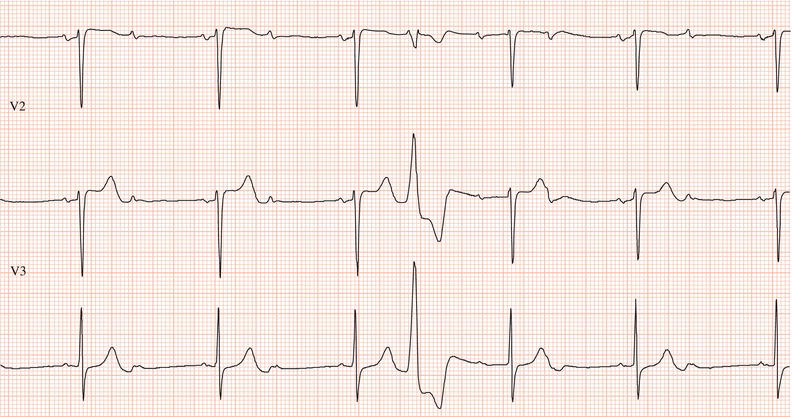
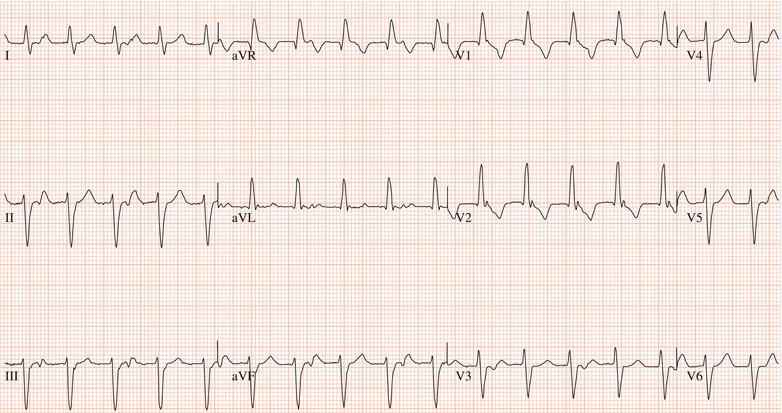
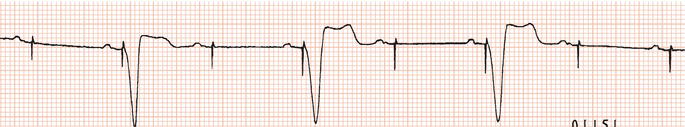
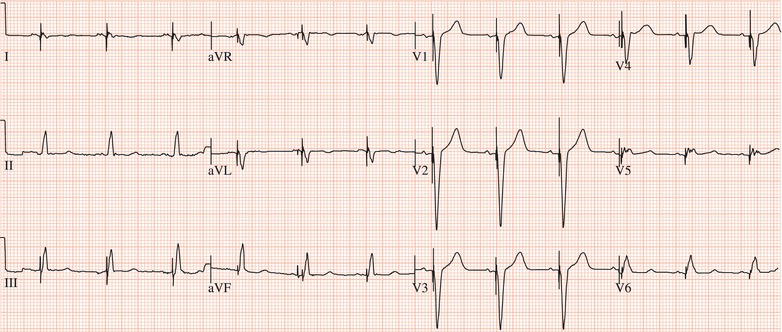
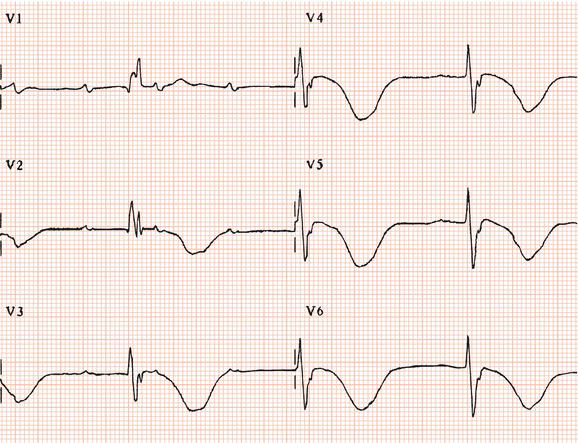
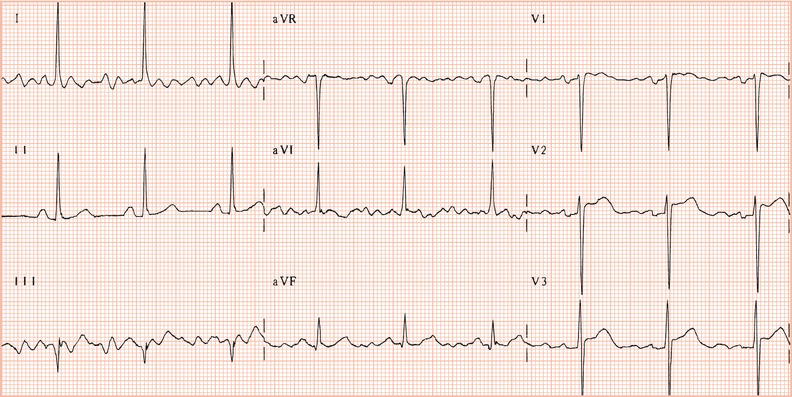
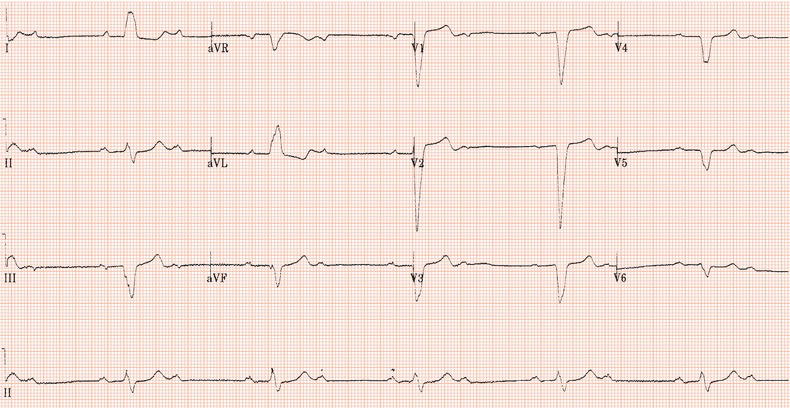
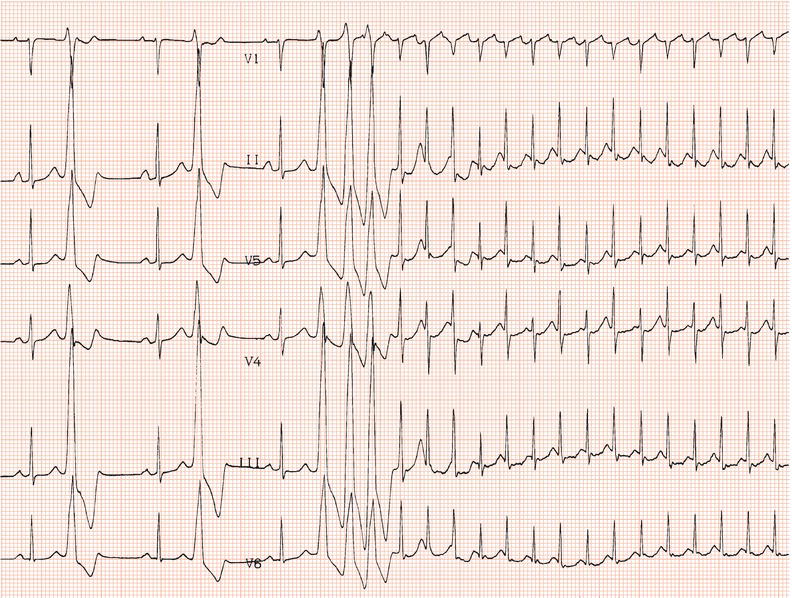
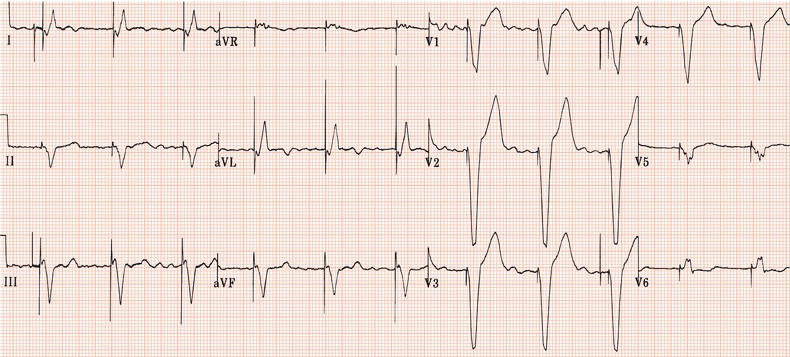
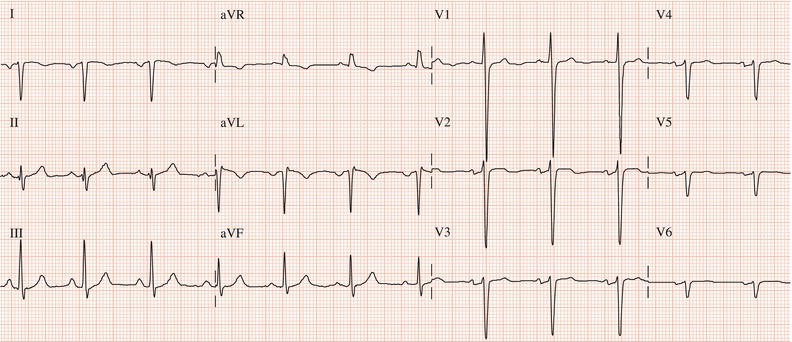
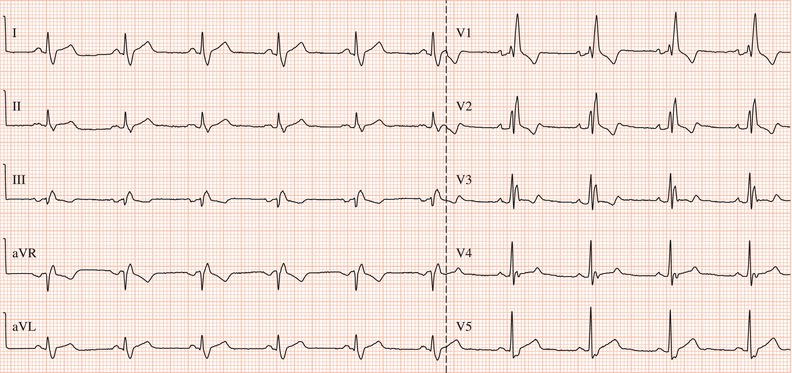
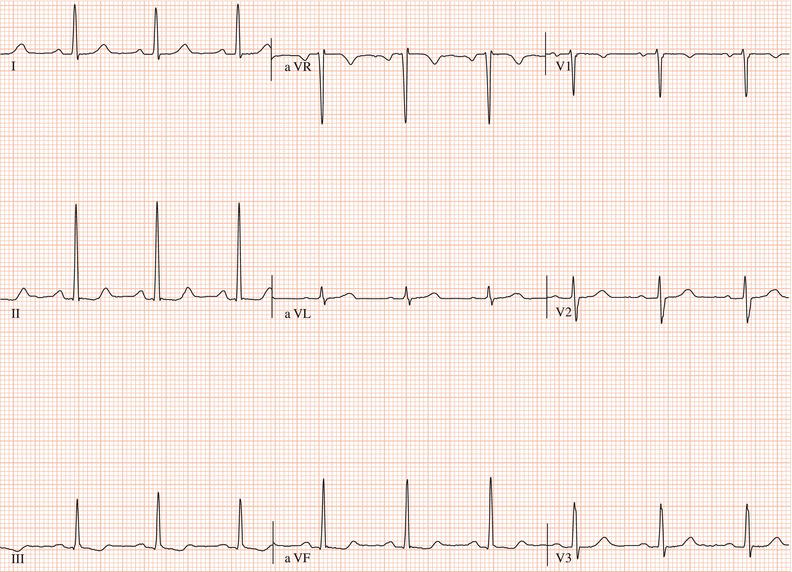
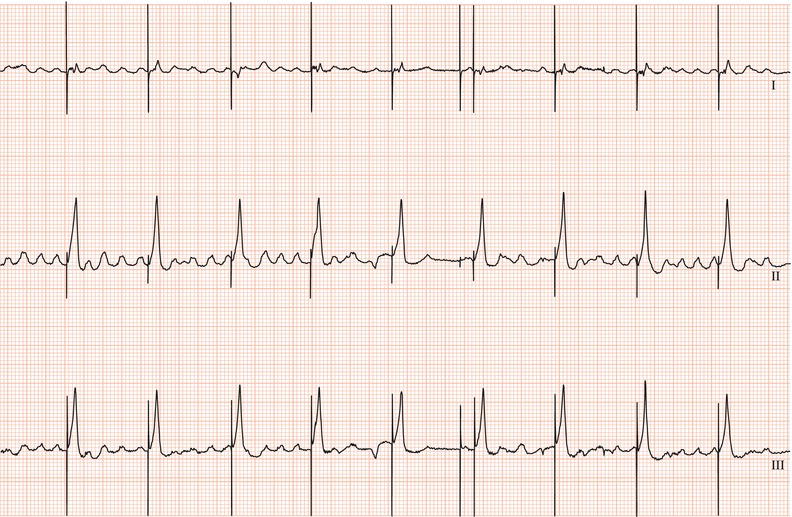
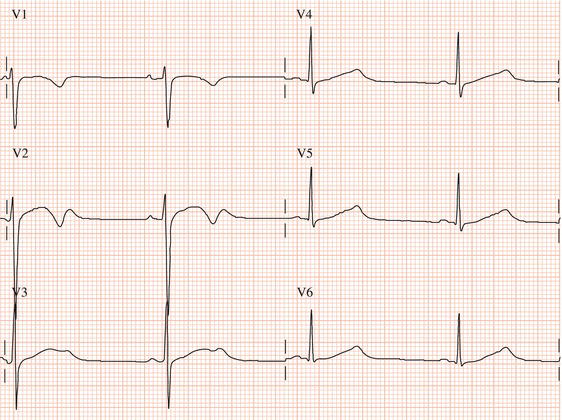
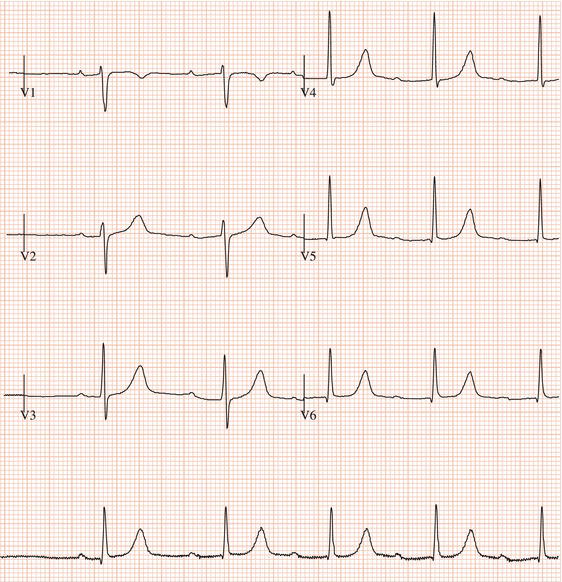
Figure 26.5 (a) Right bundle branch block? (b) Pre-excitation? (c) Right ventricular hypertrophy? (d) True posterior myocardial infarction?
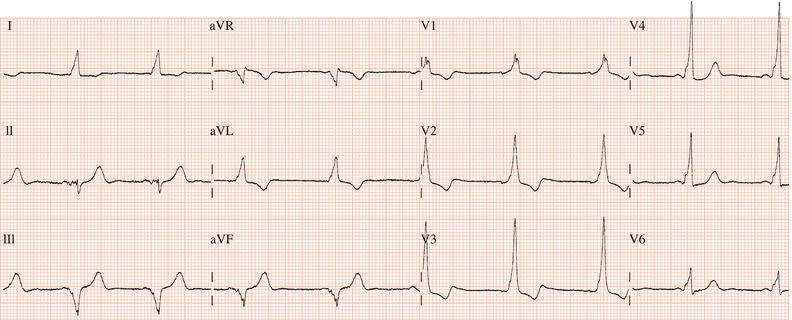
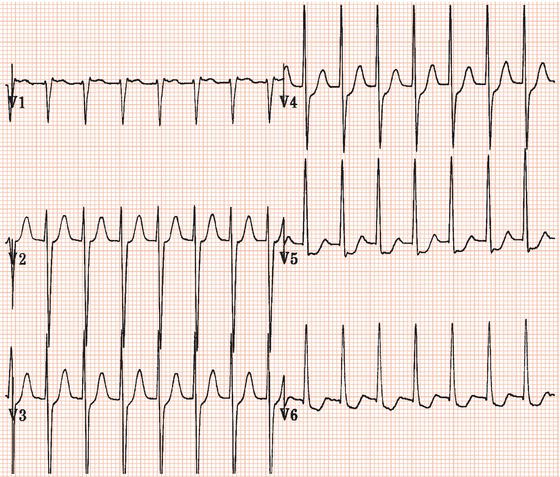
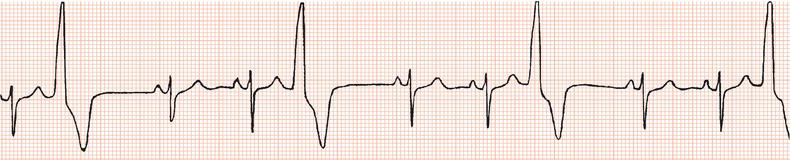
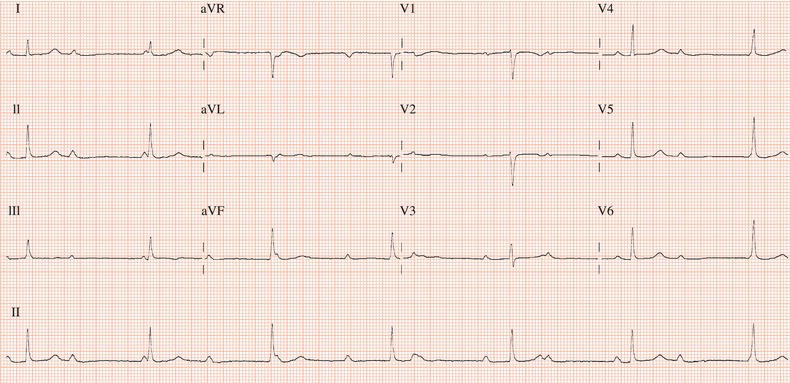
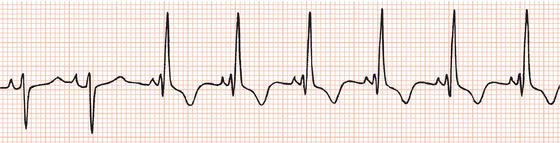
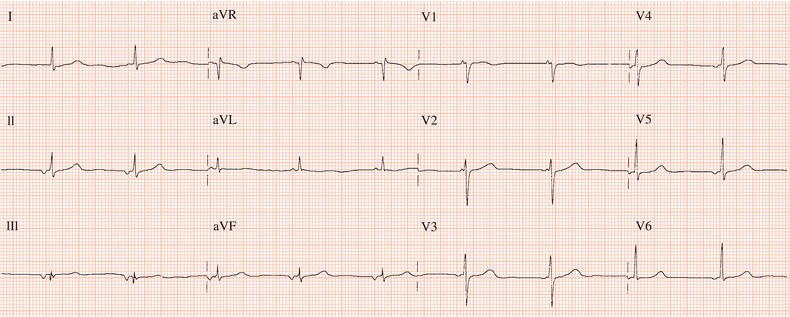
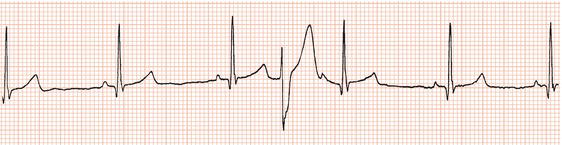
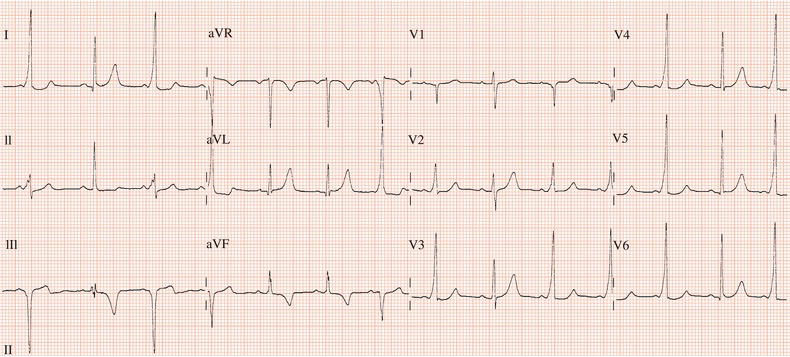
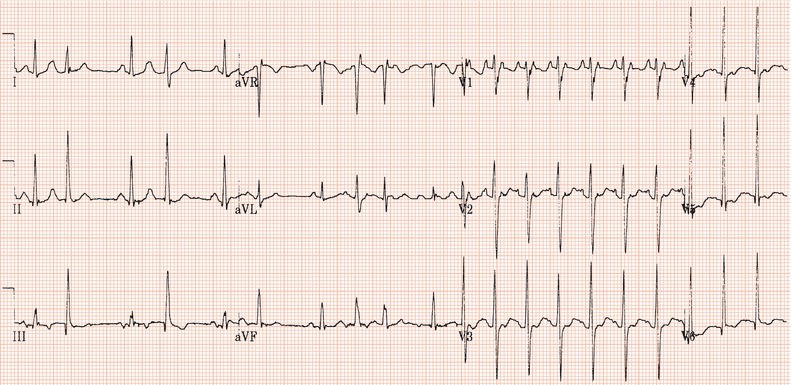
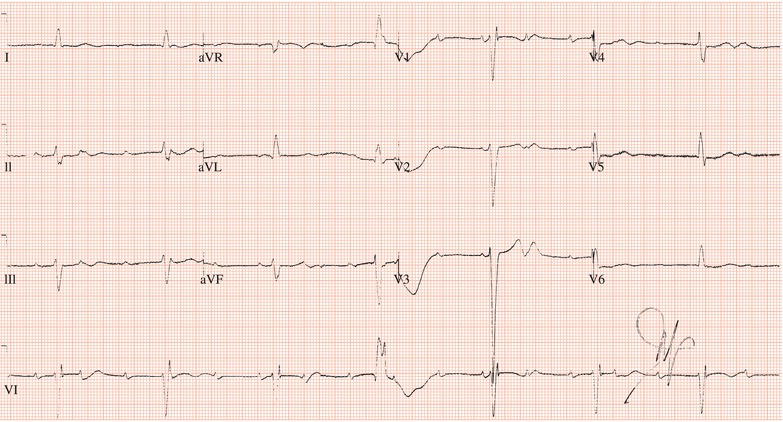
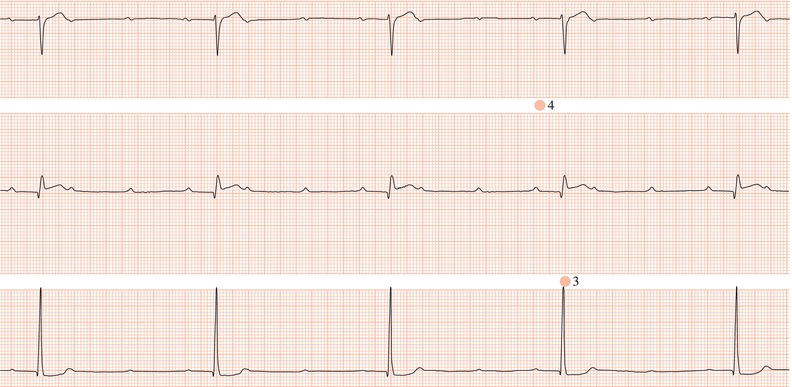
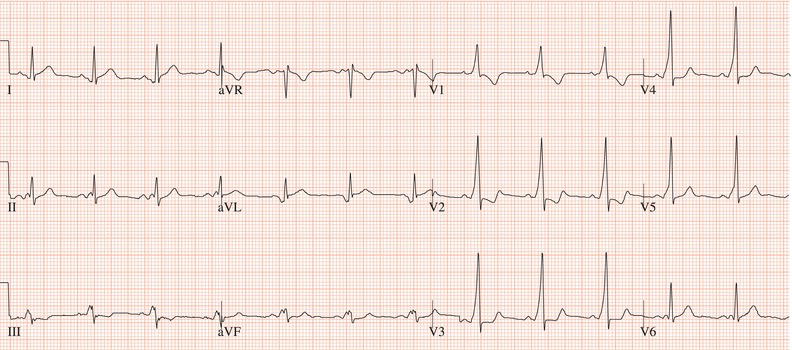
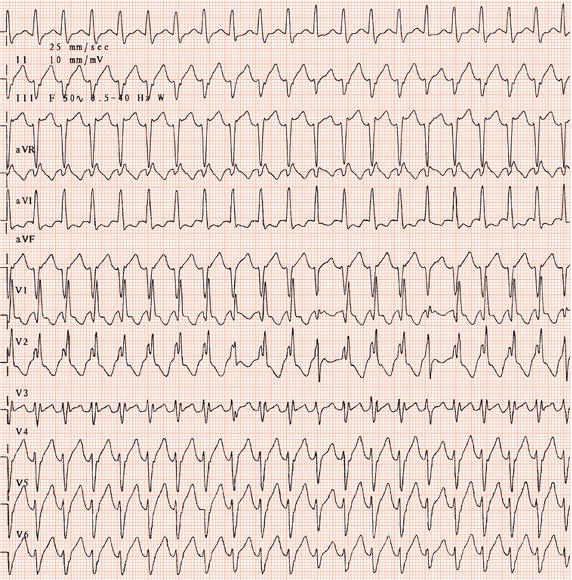
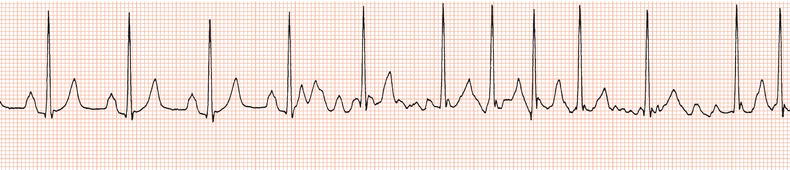
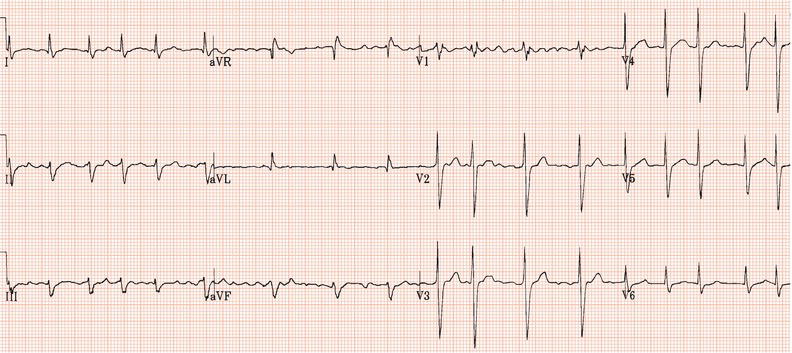
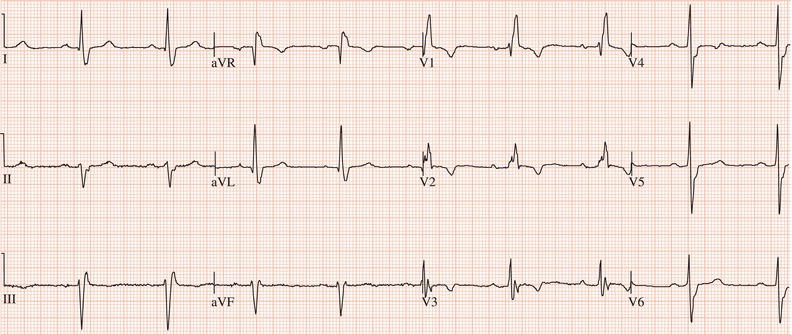
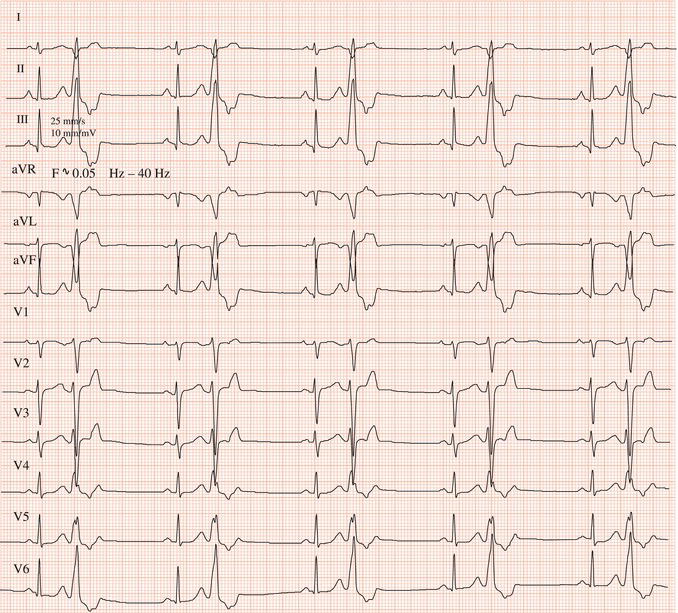
Figure 26.13 Which drug(s) might have been appropriately used? (a) Digoxin? (b) Flecainide? (c) Verapamil? (d) Sotalol? (e) Disopyramide
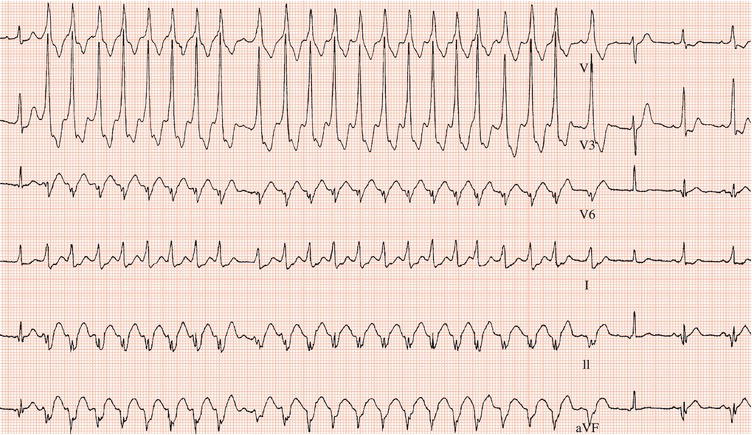
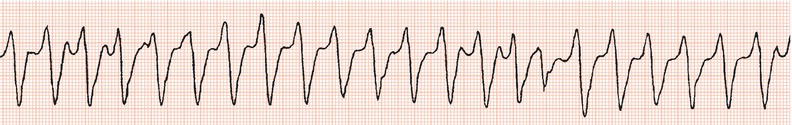
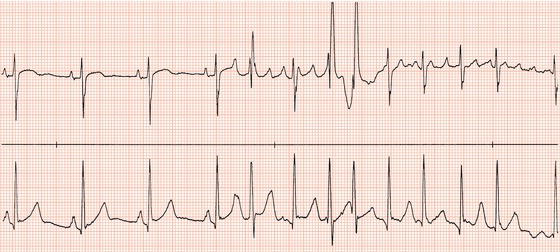
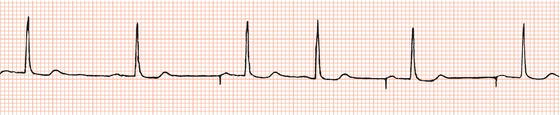
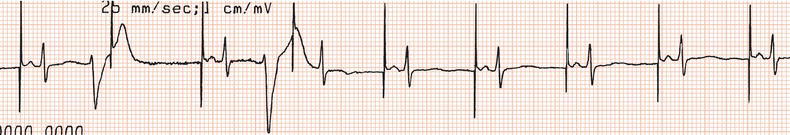
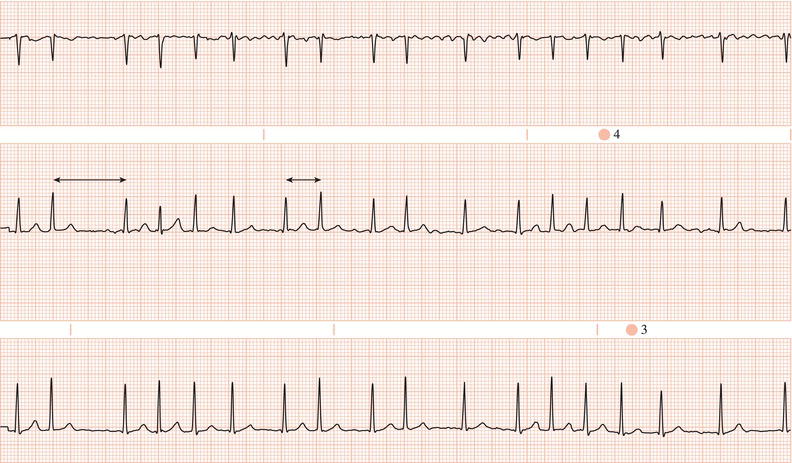
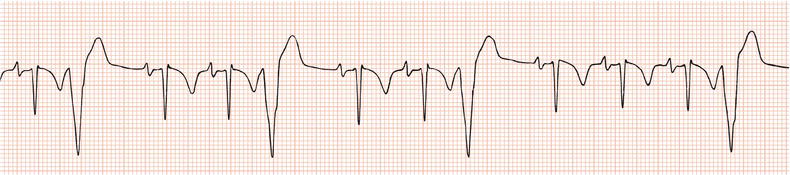
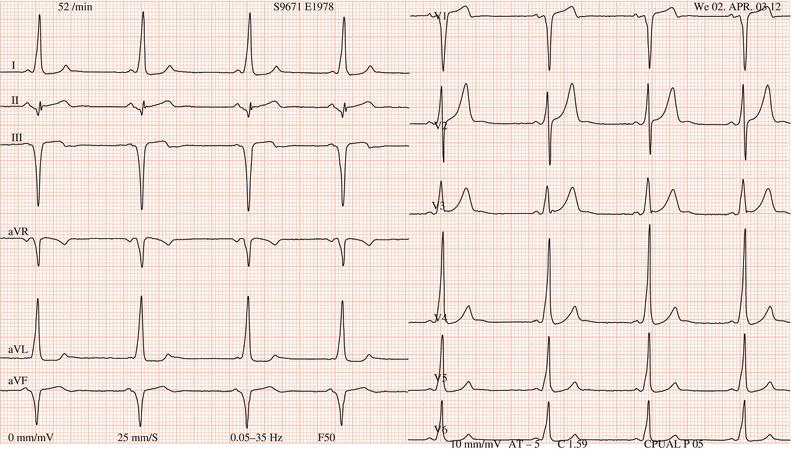
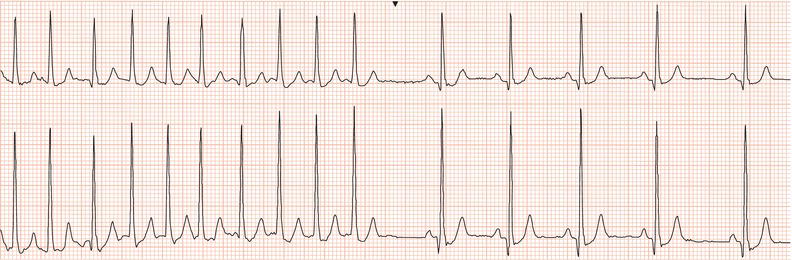
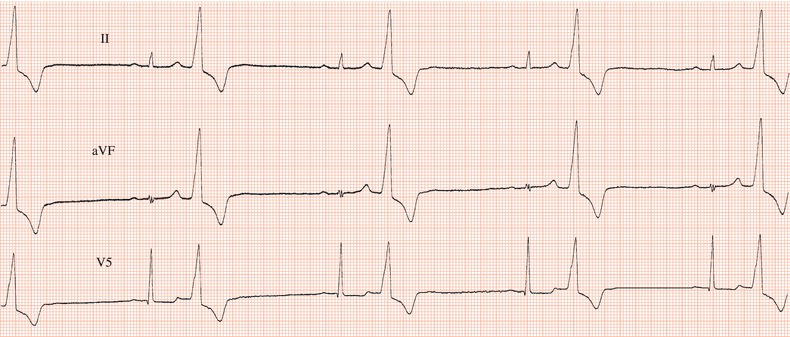
Figure 26.14 Why might have this patient complained of rapid heart beating preceding his ‘dizzy attacks’?
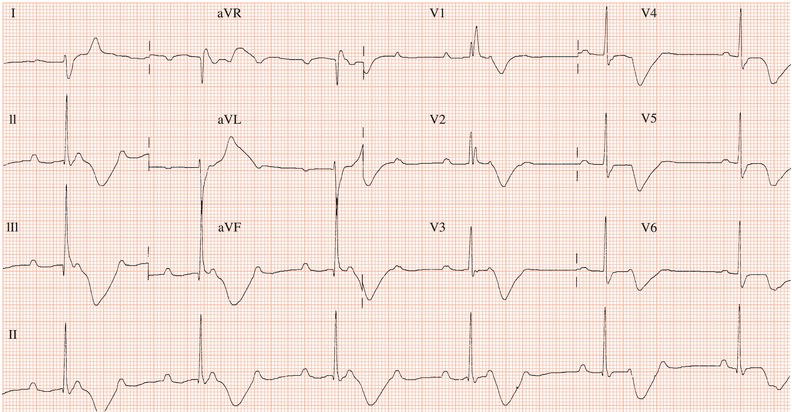
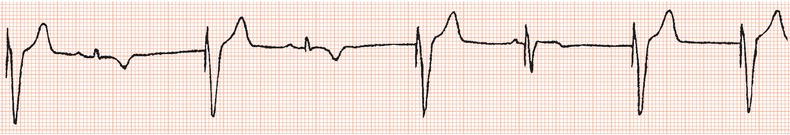
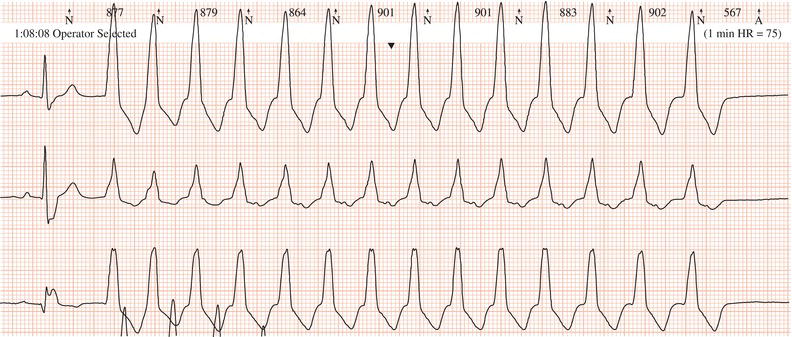
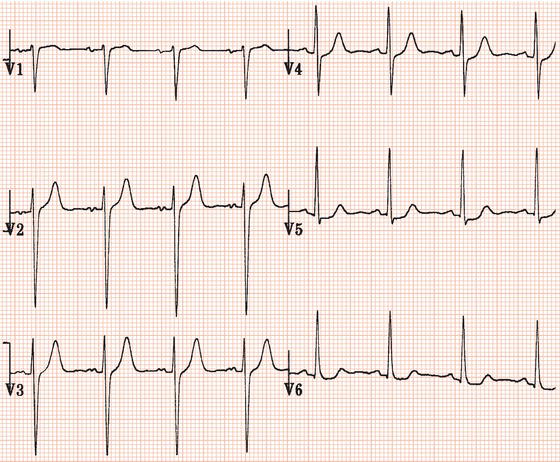
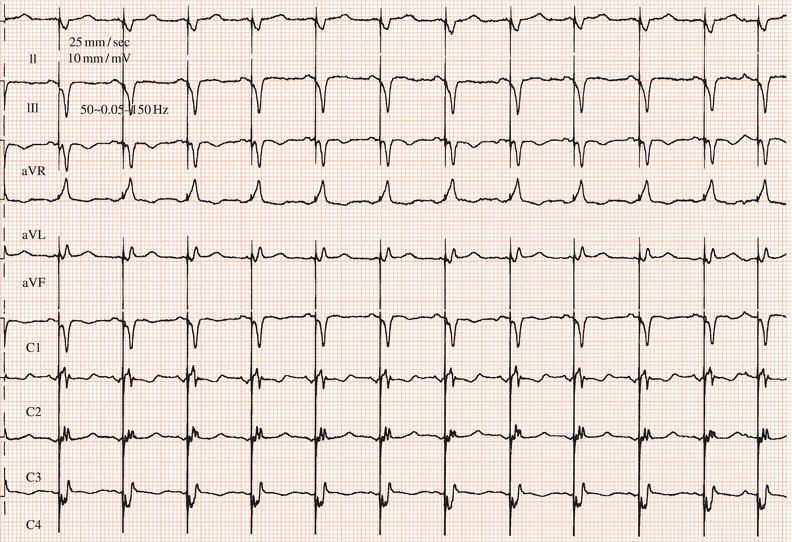
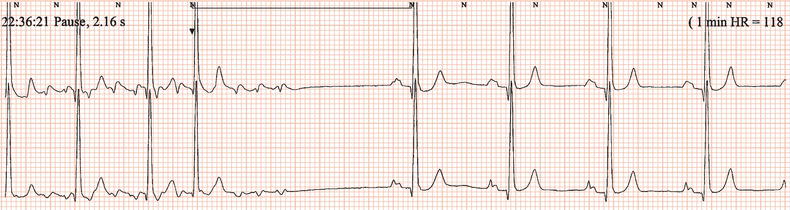
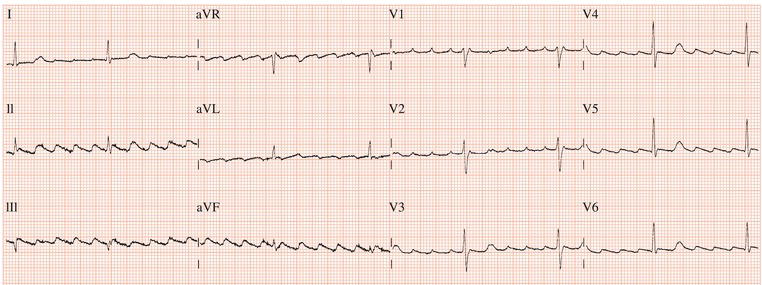
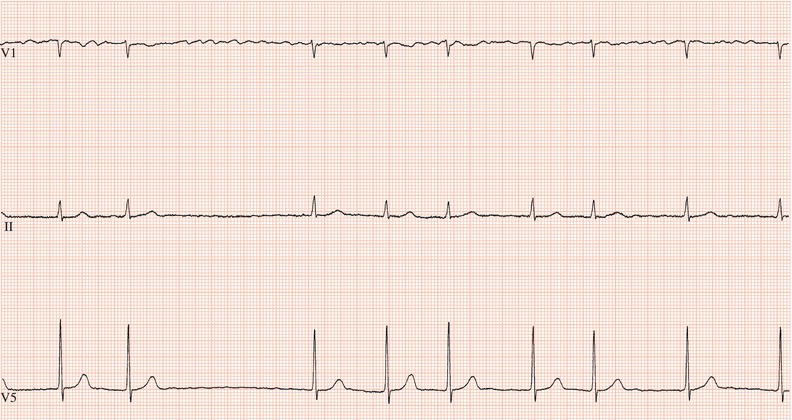
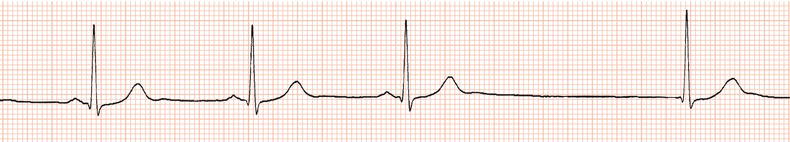
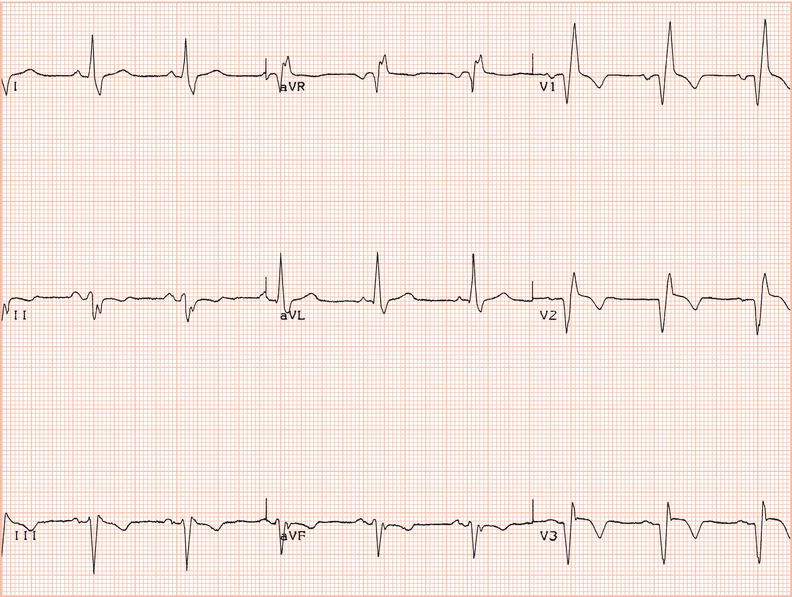
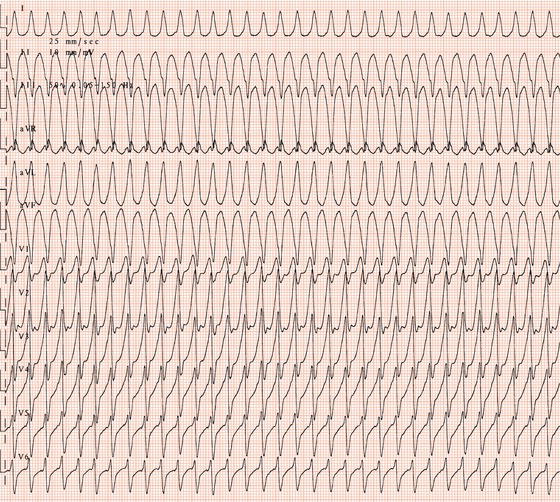
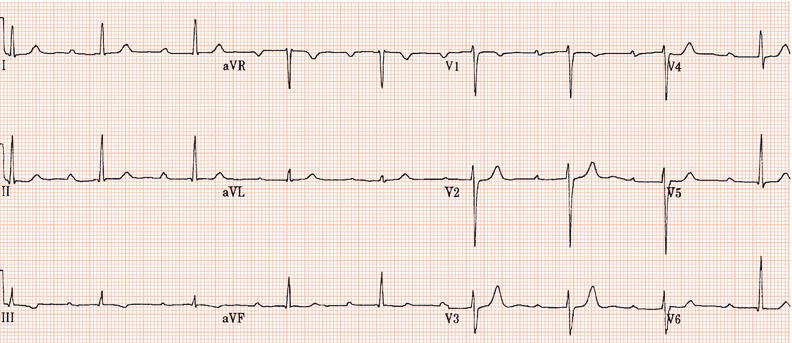
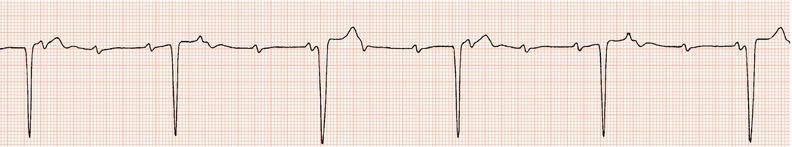
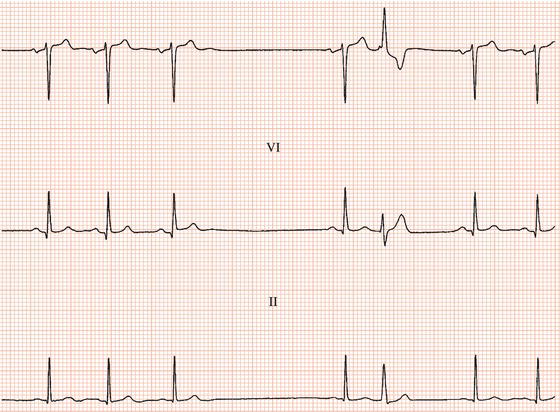
Figure 26.23 Which drug might the patient have been taking? (a) Flecainide? (b) Tetracycline? (c) Bisoprolol? (d) Clarithromycin? (e) Digoxin?
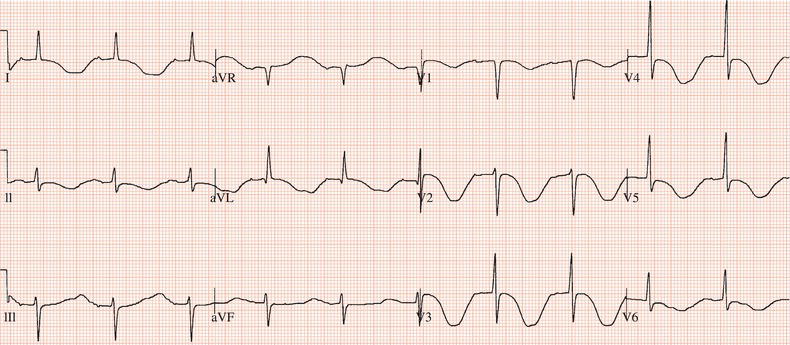
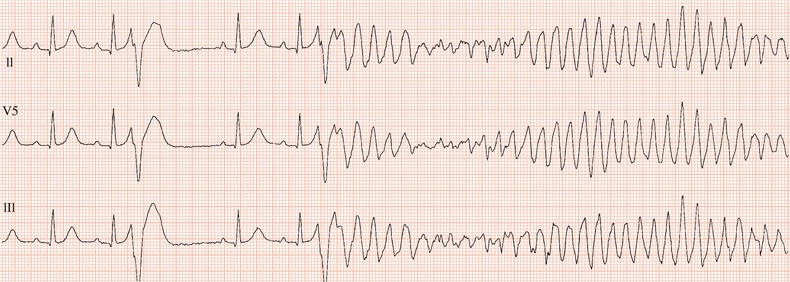
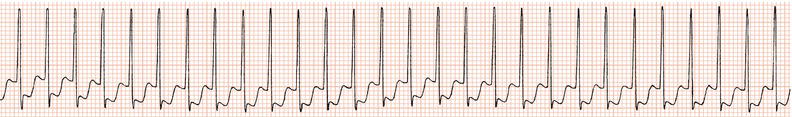
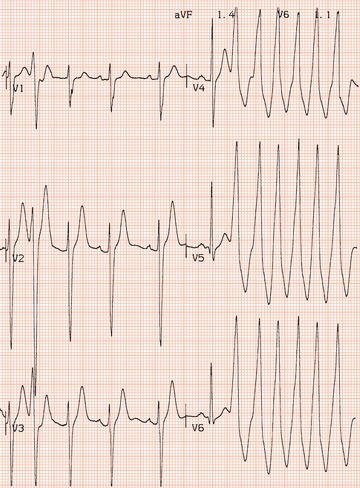
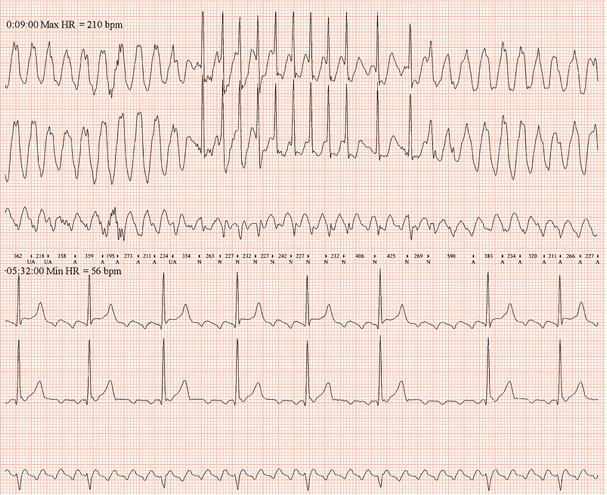
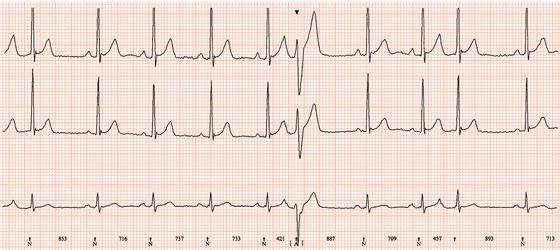
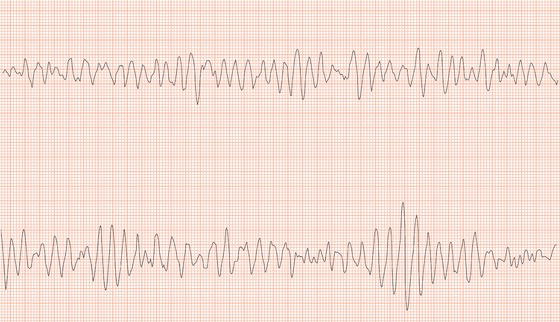
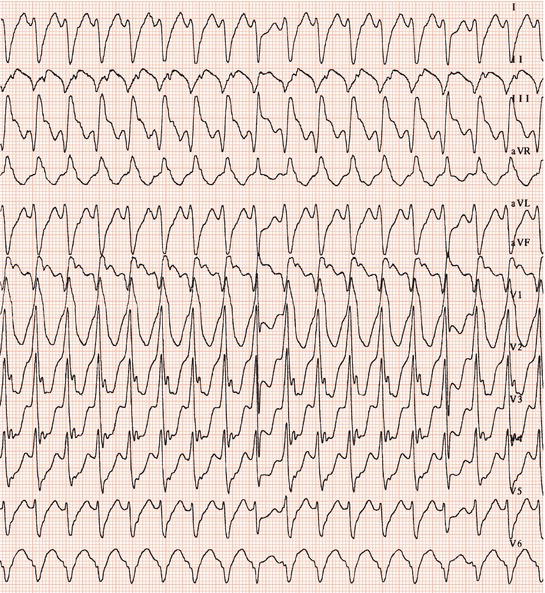
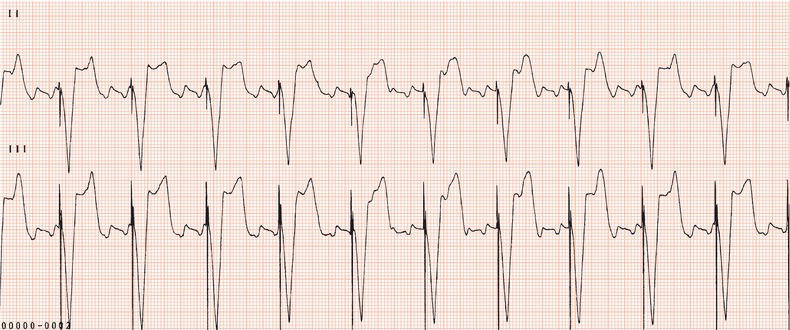
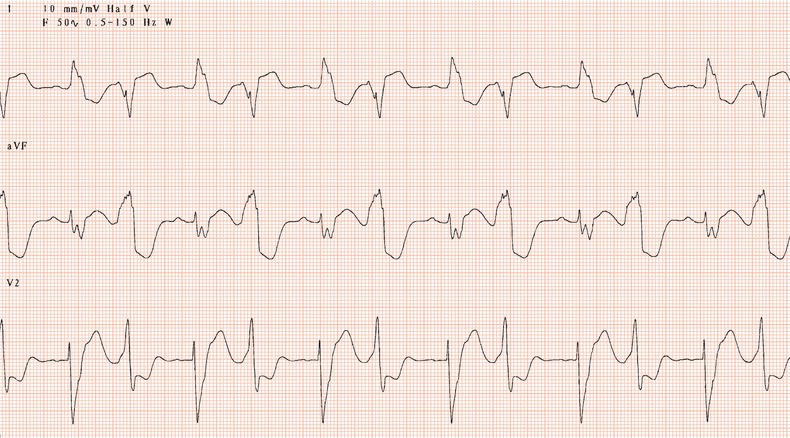
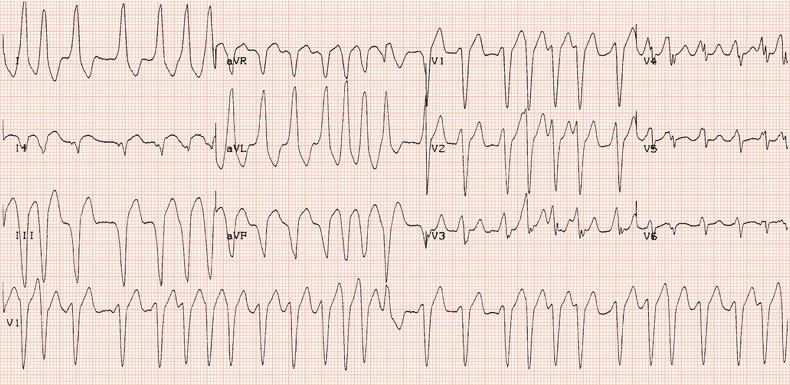
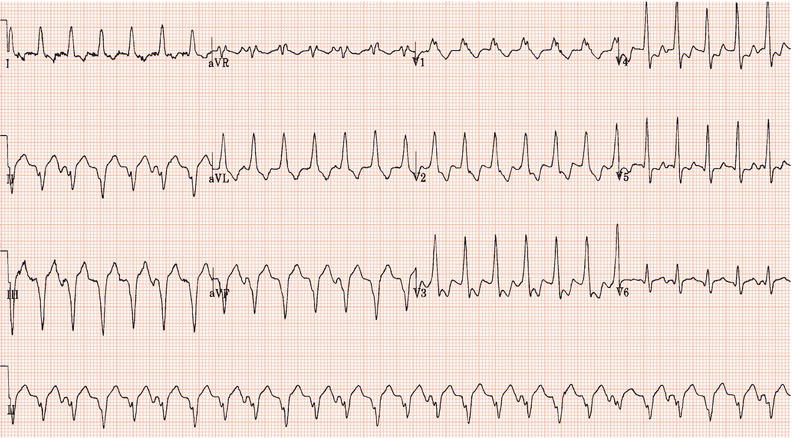
Figure 26.25 What is the arrhythmia? If catheter ablation were to be carried out, where should radiofrequency energy be delivered?
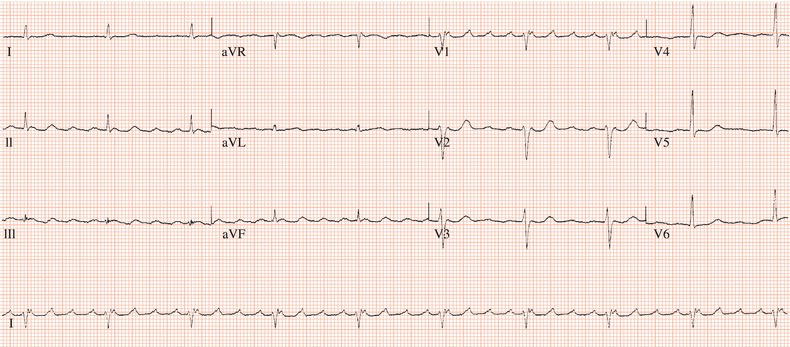
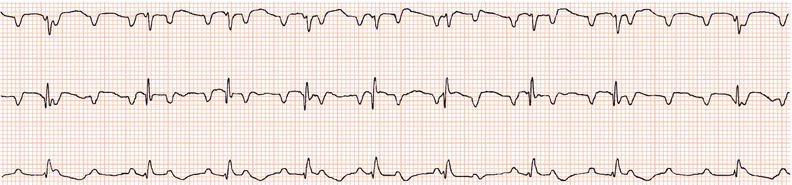
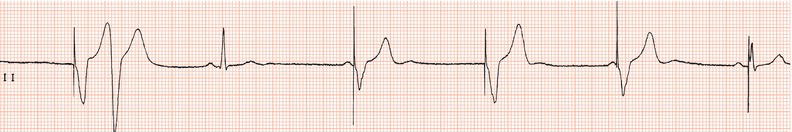
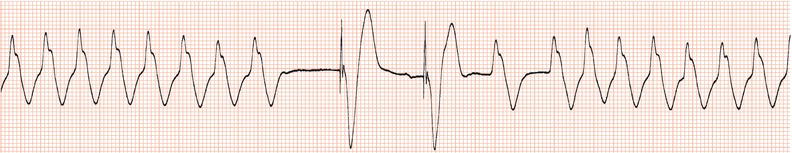
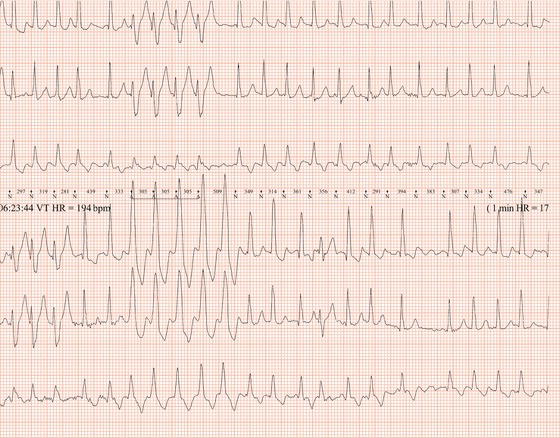
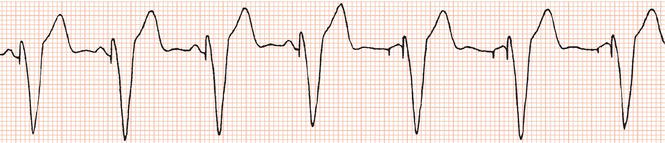
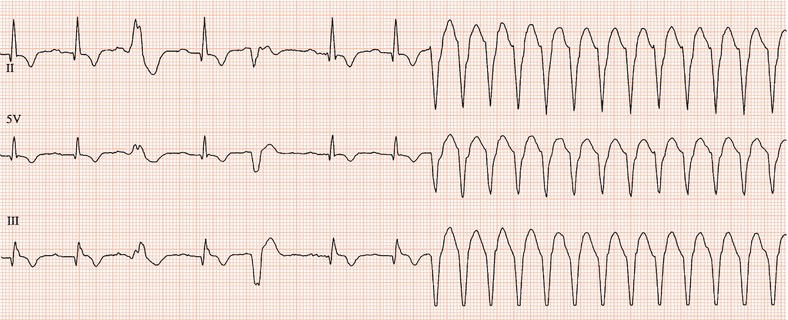
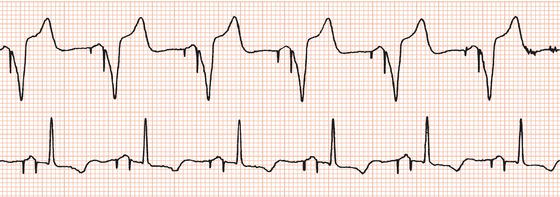
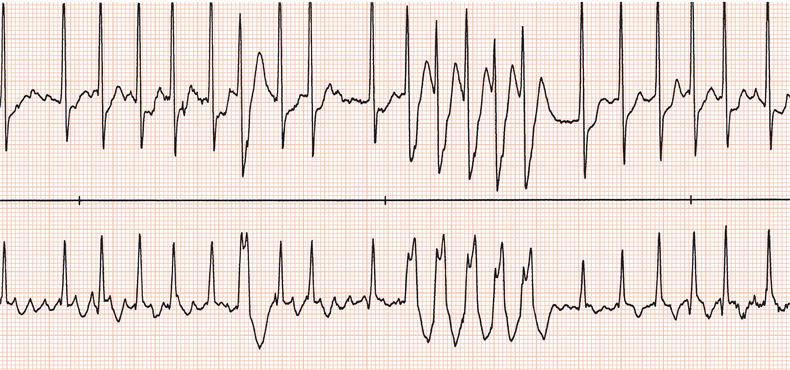
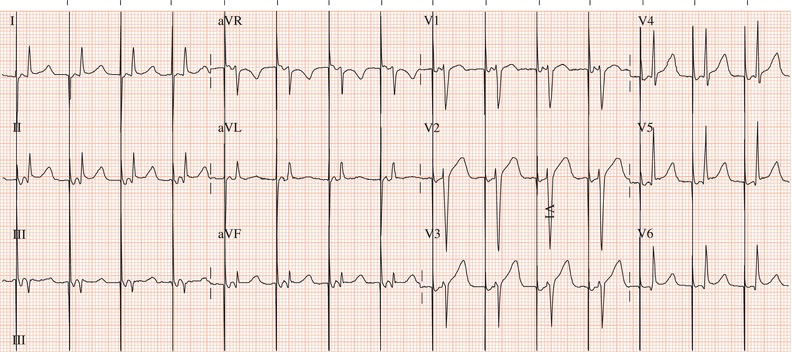
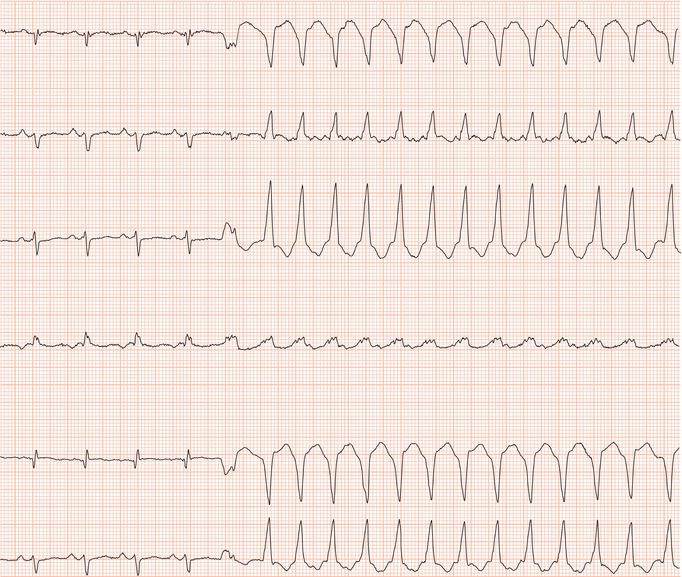
Figure 26.26 Leads V1 and V5. What is the arrhythmia? (Why is there changing morphology in lead V1?)
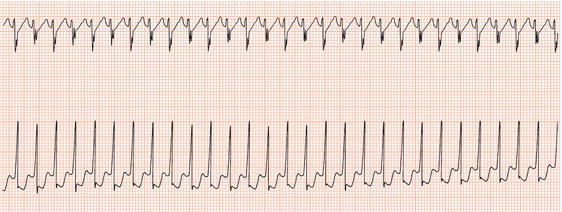
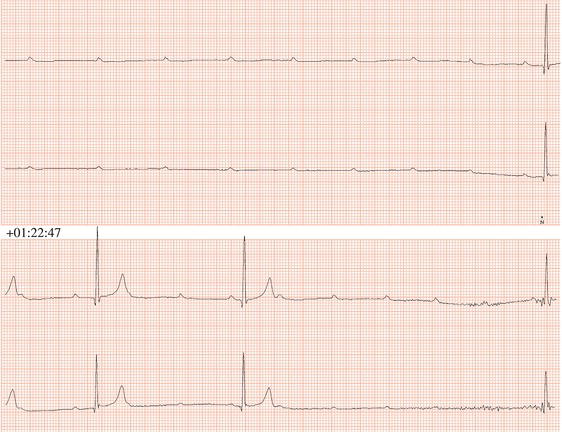
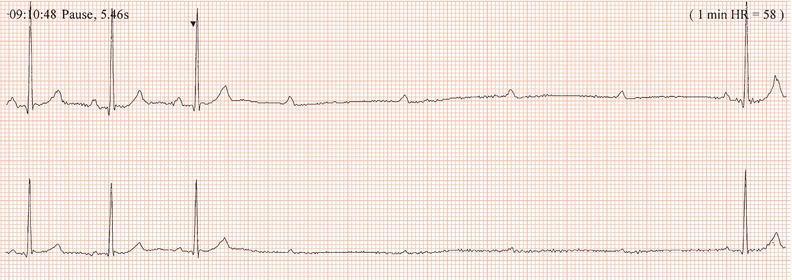
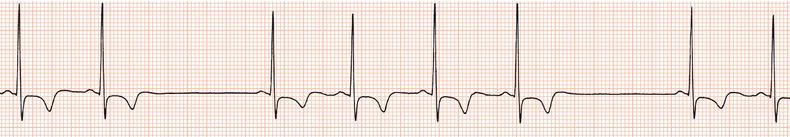
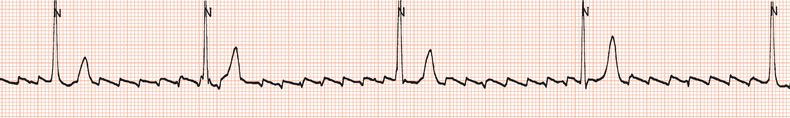
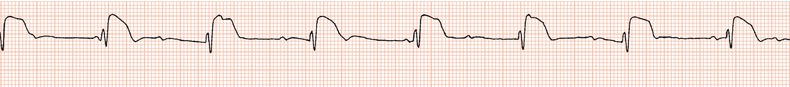
Figure 26.48 This patient had a very poorly functioning sinus node. How could an appropriate increase in heart rate during exercise be achieved?
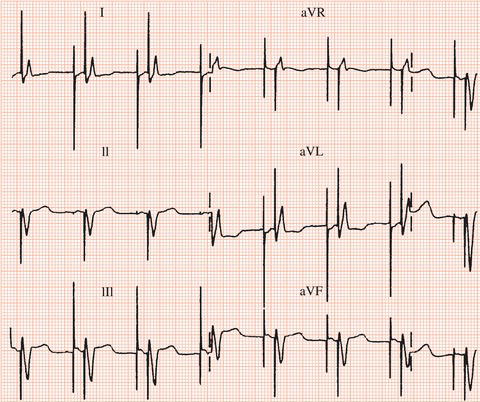
Figure 26.60 This patient experienced syncope but had a normal pulmonary artery pressure. What was the cause?
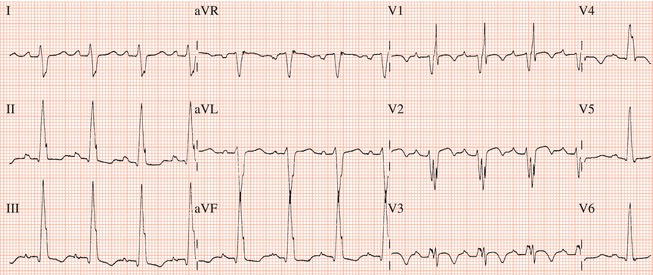
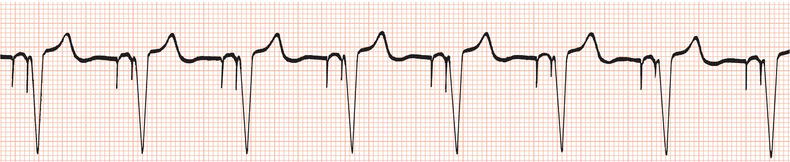
Figure 26.69 In spite of digoxin 0.125 mg daily with normal renal function and body weight. What should be done?
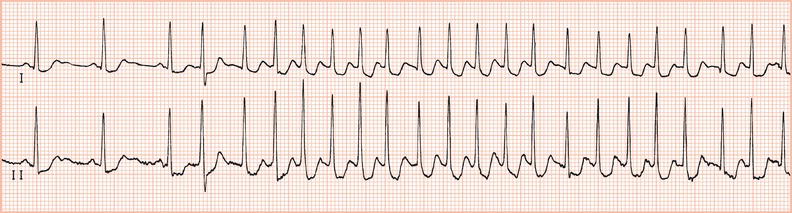
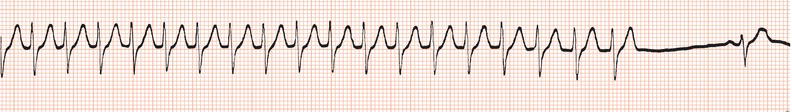
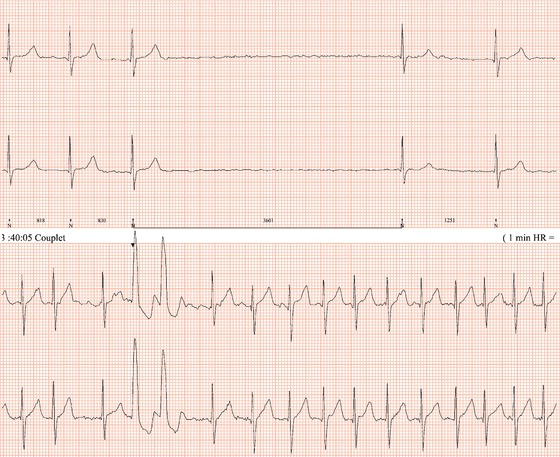
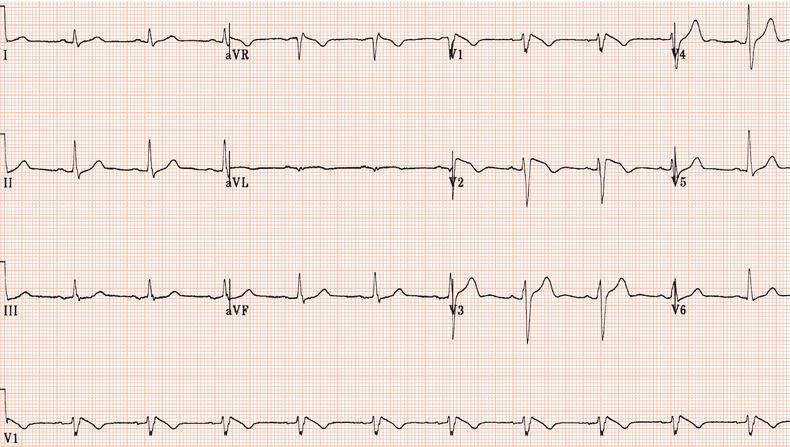
Figure 26.78 This patient had paroxysmal atrial fibrillation and good ventricular function and was prescribed flecainide.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree