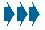Absent and Diminished Breath Sounds
1. Which conditions are associated with diminished or absent breath sounds?
2. How does each of these conditions cause diminished or absent breath sounds?
3. Does lung hyperinflation cause diminished or absent breath sounds?
4. How does positive end-expiratory pressure (PEEP) change the normal breath sound characteristics?
5. Does obesity change the normal breath sound characteristics?
SOUND PRODUCTION
Breath sounds are diminished or eliminated by conditions that limit airflow into lung segments. Slow inspiratory airflow rates decrease breath sound amplitude because less air movement occurs, resulting in less turbulent airflow.
Diminished or absent breath sounds can also occur when breath sounds are reflected at the visceral and parietal pleurae because of an impedance mismatch. A mismatch occurs when sounds are transmitted through two types of media with significantly different acoustical properties. For example, when breath sounds, which are normally transmitted through aerated lung tissue, are transmitted through a collection of fluid or air in the pleural space, sound transmission is halted or filtered. The same acoustical mismatch also occurs in patients with increased chest wall thickness. For example, in obese patients, breath sounds are diminished because they’re transmitted through a layer of adipose tissue.
Related conditions
Conditions associated with absent or diminished breath sounds include shallow breathing, diaphragmatic paralysis, airway obstruction, pneumothorax, pleural effusion, hyperinflated lungs, and obesity. The use of PEEP during assisted ventilation also is associated with diminished breath sounds.
Shallow breathing
During normal breathing in the upright position, a certain amount of air flows through the airways during inspiration and expiration; the distribution of ventilation is greater in dependent lung regions because more respiratory movement occurs. During shallow breathing, less respiratory movement occurs; consequently, less air flows through the airways during inspiration and expiration. Because of this reduced airflow, turbulence is decreased and breath sounds are diminished. (♦Sound 70)
Sound characteristics
Diminished breath sounds may be heard over the anterior, posterior, and lateral chest wall surfaces. Postoperative patients and patients with rib fractures commonly breathe shallowly because pain limits their depth of respiration. Patients with decreased levels of consciousness from central nervous system injuries or drug overdoses may also have shallow breathing.
Diaphragmatic paralysis
During inspiration in a healthy person, contraction of the domeshaped diaphragm expands the lower rib cage, forcing the abdominal contents downward and out and increasing the longitudinal lung size. Thoracic expansion lowers the intrapulmonary pressure, which allows air to flow into the airways.
When the diaphragm becomes paralyzed, as might happen with injury to the phrenic nerves, it no longer participates in normal breathing. The internal and external intercostal muscles, which also have a role in normal breathing, must take over the work of breathing. With only the chest wall muscles initiating the respiratory cycle, ventilation of the lung bases may be limited, resulting in diminished breath sounds.
Sound characteristics
Diminished sounds may be heard over the anterior, posterior, and lateral chest wall surfaces. (♦Sound 71)
In a patient with diaphragmatic paralysis, who has greatly diminished breath sounds, assess for respiratory distress and prepare for intubation and mechanical ventilation.
Airway obstruction
An obstruction in an airway blocks the flow of air and, therefore, changes the breath sounds heard during auscultation. The location of the obstruction determines where the changes in breath sounds are heard.
Sound characteristics
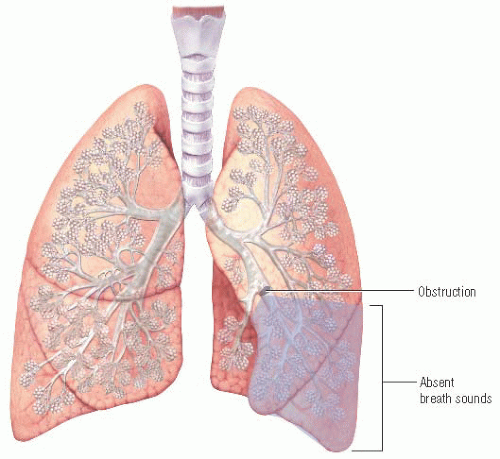
If a lobar or segmental bronchus becomes obstructed, as in a patient who has aspirated a foreign object or one who has a large mucus plug, airflow ceases distal to the obstruction; therefore, breath sounds are absent over the area distal to the obstruction.
If a mainstem bronchus is obstructed, breath sounds are absent throughout the entire affected lung. (See Mainstem bronchus obstruction, page 150.)
Aspirated foreign bodies are more likely to lodge in the right mainstem bronchus because it provides a more direct vertical passage than the left. For the same reason, endotracheal tubes are commonly misplaced in the right mainstem bronchus. If breath sounds are absent throughout the left lung field after intubation, the endotracheal tube must be repositioned.